EEG Fundamentals - Brain's Electric Chat
- EEG: Non-invasive recording of brain's spontaneous electrical activity using scalp electrodes; measures voltage fluctuations.
- Signal Origin: Primarily summated postsynaptic potentials (PSPs) from synchronously active cortical pyramidal neurons.
- Excitatory Postsynaptic Potentials (EPSPs)
- Inhibitory Postsynaptic Potentials (IPSPs)
- Volume Conduction: Signals travel through brain tissue, CSF, skull, and scalp to reach electrodes.
- Electrode Placement: Standardized International 10-20 system (e.g., Fp1, Fz, C3, Pz, Oz) ensures reproducibility.
- Montages: Define how electrode pairs are connected for recording.
- Bipolar: Between two active scalp electrodes.
- Referential: Between an active electrode and a designated, relatively inactive reference point (e.g., earlobe, mastoid).
- Amplitude: Typically 10-100 $\mu V$.
⭐ EEG primarily reflects the summated excitatory and inhibitory postsynaptic potentials (EPSPs & IPSPs) of vertically oriented pyramidal neurons in the superficial layers of the cerebral cortex, not action potentials directly.
Normal EEG Rhythms - Wave Watching 101
The primary EEG rhythms are categorized by their frequency, amplitude, typical scalp location, and associated physiological or behavioral states:
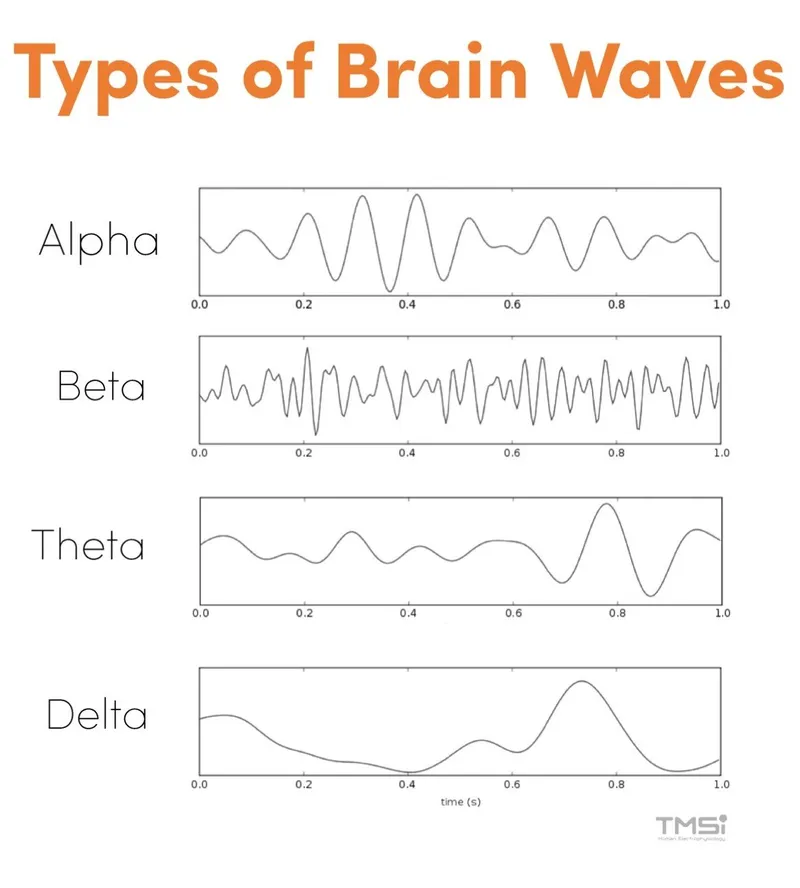
| Wave | Frequency (Hz) | Amplitude | Location | Physiological State |
|---|---|---|---|---|
| Alpha | 8-13 | 20-60 µV | Occipital (post.) | Awake, relaxed, eyes closed. |
| Beta | >13-30 | <20 µV | Frontal (ant.) | Alert, active thinking, anxiety, REM sleep. |
| Theta | 4-7.5 | 20-100 µV | Temporal, Parietal | Drowsiness, light sleep; normal in children. |
| Delta | 0.5-4 | >75 µV | Diffuse (frontal) | Deep sleep (NREM 3/4), infancy; pathological if awake adult. |
📌 Mnemonic (frequency ↑): Deep Thoughts Are Best (Delta, Theta, Alpha, Beta).
Provoking Patterns - Stirring Up Waves
-
Sleep Stages & Associated EEG Waveforms:
- N1 (Drowsiness): ↓ Alpha, ↑ Theta; Vertex sharp waves (V waves).
- N2 (Light Sleep): Sleep spindles (12-14 Hz bursts); K-complexes (large biphasic waves).

- N3 (Deep/SWS): Delta waves (0.5-2 Hz, >20% epoch); high amplitude, slow waves.
- REM Sleep: Low voltage, mixed frequency (theta, beta); characteristic sawtooth waves. EEG resembles awake state.
-
Provocative Maneuvers (Activation Procedures):
- Hyperventilation (HV): Deep breathing for 3-5 minutes.
- Mechanism: ↓PaCO₂ (hypocapnia) → cerebral vasoconstriction → relative hypoxia → diffuse EEG slowing (delta).
- Utility: Effectively provokes typical absence seizures (generalized 3 Hz spike-wave).
- Intermittent Photic Stimulation (IPS): Stroboscopic light flashes at varying frequencies (e.g., 1-30 Hz).
- Responses: Photic driving (occipital rhythm entrainment); photoparoxysmal response (PPR - generalized epileptiform discharges).
- Sleep Deprivation: Significantly lowers seizure threshold, unmasking abnormalities.
- Utility: Increases yield of Interictal Epileptiform Discharges (IEDs), aids epilepsy diagnosis.
- Hyperventilation (HV): Deep breathing for 3-5 minutes.
⭐ Hyperventilation is a key activator for typical absence seizures, often eliciting the characteristic 3 Hz spike-and-wave discharges.
Abnormal EEG - Decoding Distress Calls
- Epileptiform Discharges: Hallmark of seizure predisposition.
- Spikes: Brief (<70 ms), sharply contoured.
- Sharp waves: Longer duration (70-200 ms), less sharp.
- Spike-and-wave complexes:
- Generalized 3 Hz: Typical absence seizures.
- Slow spike-wave (<2.5 Hz): Lennox-Gastaut syndrome.
- Non-Epileptiform Abnormalities:
- Slowing (focal/generalized): Indicates cerebral dysfunction (ischemia, tumor, metabolic).
- Periodic Patterns:
- PLEDs (Periodic Lateralized Epileptiform Discharges): Acute destructive lesions (stroke, HSV encephalitis).
- Triphasic Waves: Characteristic of metabolic encephalopathy, especially hepatic.
- Burst Suppression: Severe encephalopathy, anoxia, deep anesthesia; ominous sign.
- Specific Patterns:
- Hypsarrhythmia: Disorganized, high-voltage slow waves and spikes; seen in Infantile spasms (West syndrome).
- GPEDs/PSIDDs (Generalized Periodic Epileptiform Discharges): Often in Creutzfeldt-Jakob Disease (CJD).
- PLIDDs (Periodic Long-Interval Diffuse Discharges): Associated with Subacute Sclerosing Panencephalitis (SSPE).
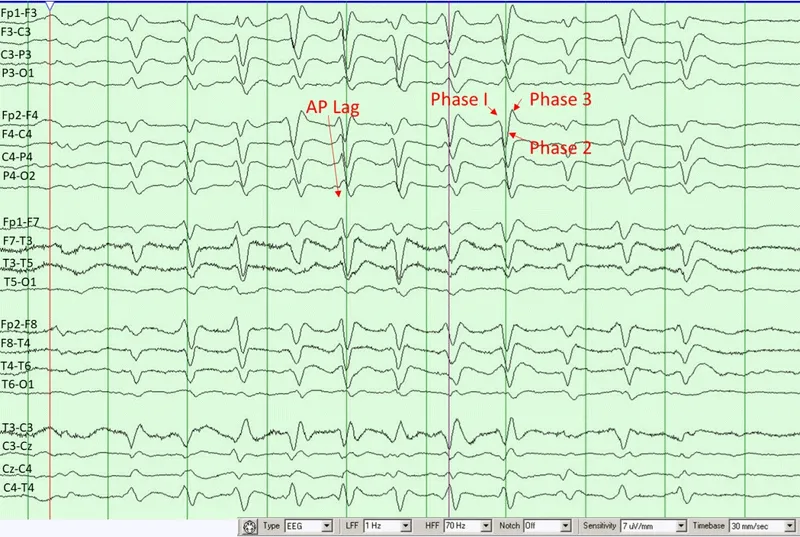
⭐ Triphasic waves, classically seen in hepatic encephalopathy, are high-amplitude (>70 μV) positive deflections, preceded and followed by negative waves, repeating periodically at 1-2 Hz.
High‑Yield Points - ⚡ Biggest Takeaways
- Alpha waves (8-13 Hz): Characteristic of awake, relaxed adults with eyes closed; primarily occipital.
- Beta waves (>13 Hz): Associated with alertness, active thinking, and REM sleep; mainly frontal.
- Theta waves (4-7 Hz): Seen in drowsiness, light sleep, and emotional stress in adults.
- Delta waves (<4 Hz): Indicate deep sleep (NREM 3 & 4), infancy, or significant brain pathology.
- Sleep spindles & K-complexes: Definitive hallmarks of Stage N2 sleep.
- Hypsarrhythmia: A chaotic EEG pattern pathognomonic for infantile spasms (West syndrome).
- Triphasic waves: Often indicative of metabolic encephalopathy (e.g., hepatic encephalopathy).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

