K+ Basics - The Great Balancer
- $K^+$ is the predominant intracellular cation.
- Normal plasma $K^+$ range: 3.5-5.0 mEq/L.
- Total body $K^+$: Approximately 50 mEq/kg.
- Distribution: Vast majority (98%) resides in Intracellular Fluid (ICF); only 2% in Extracellular Fluid (ECF).
- Crucial for establishing Resting Membrane Potential (RMP).
- Modulates neuromuscular excitability and cardiac function.
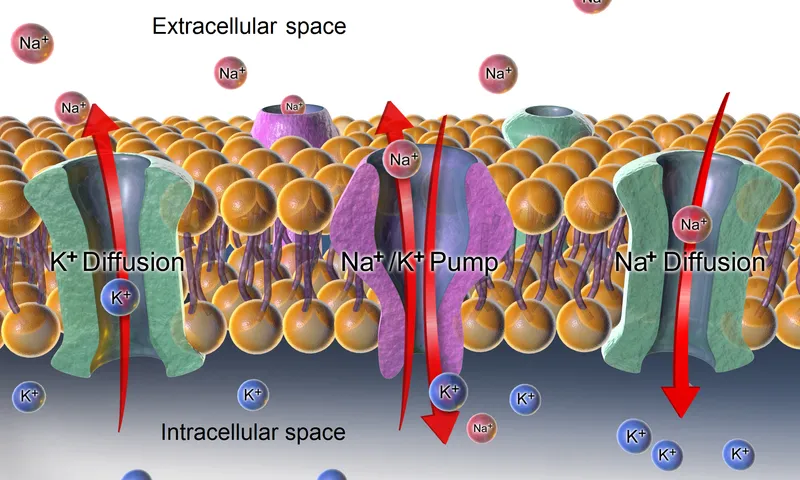
⭐ Over 98% of total body potassium is located in the intracellular compartment.
K+ Shifters - In & Out Game
Internal potassium balance involves rapid transcellular K+ shifts, primarily regulated by the $Na^+/K^+$ ATPase pump.
| K+ IN (↓ Serum K+) | K+ OUT (↑ Serum K+) |
|---|---|
| * Insulin | * Acidosis (mineral) |
| * Aldosterone | * Hyperosmolality |
| * Beta-2 agonists | * Alpha-agonists |
| * Alkalosis | * Beta-blockers |
| * Cell lysis (rhabdomyolysis, tumor lysis) | |
| * Succinylcholine, Digitalis toxicity |
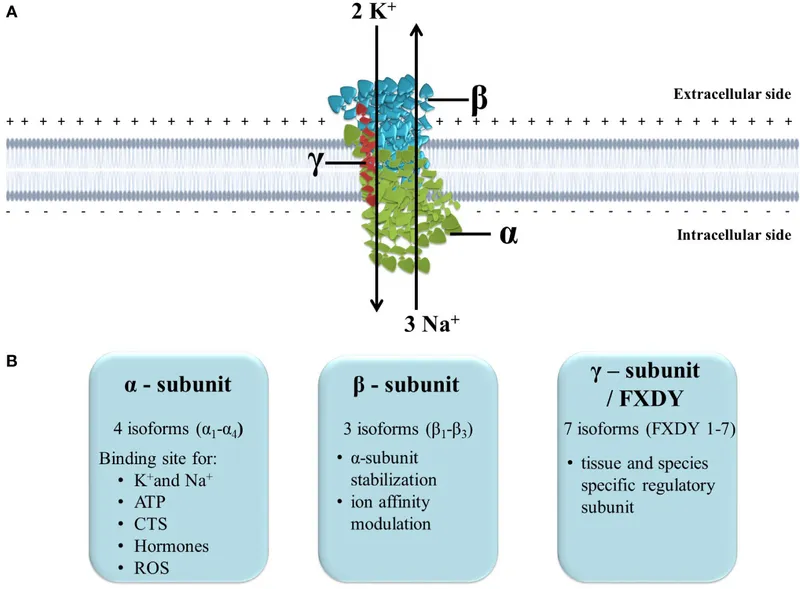
⭐ Insulin promotes K+ uptake into cells by stimulating the sodium-potassium ATPase pump.
Kidney's K+ Dance - Renal Rhapsody
- External K+ balance: Primarily via kidneys.
- Renal Journey:
- Freely filtered at glomerulus.
- PT & LOH: ~90% reabsorbed.
- DT & CD: Fine-tuning.
- Principal cells: Secrete K+ ($ROMK$, $BK etta channels$).
- Intercalated cells: Reabsorb K+ ($H^+/K^+$ ATPase).
⭐ Aldosterone is the major hormonal regulator of urinary potassium excretion, acting on principal cells in the late distal tubule and collecting duct to increase K+ secretion.
K+ Ups & Downs - Too Little, Too Much
| Feature | Hypokalemia | Hyperkalemia |
|---|---|---|
| Definition | $K^+ < \textbf{3.5} \text{ mEq/L}$ | $K^+ > \textbf{5.0-5.5} \text{ mEq/L}$ |
| Key Causes | ↓intake, ↑entry into cells, ↑losses (renal/GI) | ↑intake, ↓excretion (renal failure, drugs), shift out of cells (acidosis, cell lysis) |
| Key Clinical | Muscle weakness, fatigue, cramps, ileus, arrhythmias, polyuria | Muscle weakness, paralysis, paresthesias, cardiac arrhythmias |
| Key ECG | Flattened T wave, U wave, ST depression, prolonged QT. 📌 "U see a flat T" | Peaked T waves, prolonged PR, wide QRS, sine wave, asystole. 📌 "Peaked T, Wide QRS" |
⭐ Peaked T waves are the earliest and most common ECG finding in hyperkalemia.
K+ Fixes - Emergency Toolkit
-
Hypokalemia Management:
- Treat cause. Oral/IV KCl (rate: 10-20 mEq/hr; monitored: up to 40 mEq/hr).
- Monitor K+. Correct Mg deficiency.
-
Hyperkalemia Management (Emergency): 📌 "C BIG K Drop"
- Calcium gluconate/chloride (cardiac membrane stabilization).
- Beta-2 agonists / Bicarbonate (shift K+ into cells).
- Insulin (+ Glucose) (shift K+ into cells).
- Kayexalate / K+ binders (remove K+).
- Diuretics / Dialysis (remove K+).
⭐ In severe hyperkalemia with ECG changes, intravenous Calcium gluconate is administered first to stabilize the cardiac membrane, even before measures to lower serum potassium.
High‑Yield Points - ⚡ Biggest Takeaways
- Aldosterone is the main regulator of renal K+ excretion.
- Insulin & β2-agonists shift K+ into cells (↓ serum K+).
- Acidosis (↓pH) shifts K+ out of cells (↑ serum K+); alkalosis (↑pH) shifts K+ in.
- ECG changes are crucial: hyperkalemia (peaked T, wide QRS); hypokalemia (U waves, flat T).
- Principal cells (late DCT/CD) are key for K+ secretion.
- α-intercalated cells reabsorb K+ in K+ depletion.
- Hyperosmolarity shifts K+ out of cells.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

