Pediatric Dosing Principles - Tiny Patients, Big Challenges
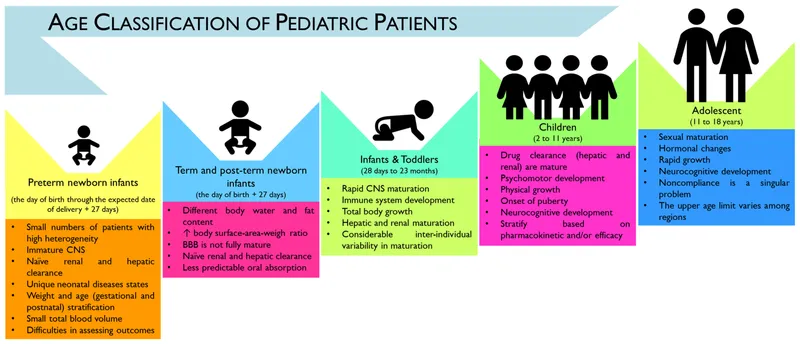
- Dosing: weight (mg/kg), BSA ($mg/m^2$), formulas. NOT "small adult" doses.
- Pharmacokinetic (PK) Variations:
- Absorption: Gastric pH ↑, emptying delayed. IM erratic. Percutaneous ↑ (↑ toxicity risk).
- Distribution: TBW ↑ (70-80%; ↑ Vd water-soluble), fat ↓ (↓ Vd lipid-soluble). Protein binding ↓ (↑ free drug). BBB immature.
- Metabolism: Hepatic enzymes immature (CYP450 ↓, glucuronidation ↓) → prolonged $t_{1/2}$. 📌 "Slow Liver Metabolism".
- Excretion: Renal (GFR ↓, ~30-40% adult at birth) → prolonged elimination. Matures 1-2 yrs.
- PD Variations: Receptor sensitivity/number differ. Paradoxical effects (e.g., benzodiazepines).
⭐ Neonates and infants have a higher percentage of total body water and lower body fat compared to adults, affecting drug distribution.
Pediatric Pharmacokinetics - Absorb & Distribute
Absorption
- Gastric pH: Neonates ↑ (alkaline, 6-8), adult pH (1-3) by 2-3 yrs.
- Impacts acid-labile (↑ penicillin) & weak-acid drugs (↓ phenobarbital).
- Gastric Emptying: Prolonged in neonates (adult by 6-8 mo); affects absorption rate.
- Percutaneous: ↑ in neonates (thin skin, ↑ Surface Area to Body Weight ratio). ⚠️ High systemic toxicity risk.
- IM: Erratic (↓ muscle mass/flow).
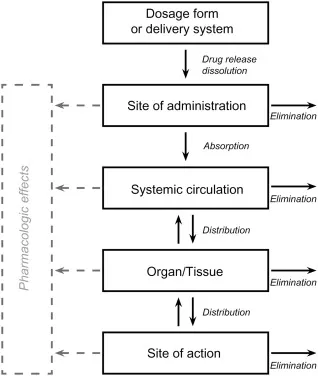
Distribution
- Body Water: Neonates ↑ Total Body Water (TBW ~75-80%), ↑ Extracellular Fluid (ECF).
⭐ Neonates: ↑ Volume of distribution (Vd) for water-soluble drugs (e.g., gentamicin); ↓ Vd for lipid-soluble drugs (e.g., diazepam) due to body composition.
- Protein Binding: Neonates ↓ albumin, ↓ affinity.
- ↑ free drug (e.g., phenytoin). ⚠️ Kernicterus risk (e.g., sulfonamides).
- Blood-Brain Barrier (BBB): More permeable in neonates; ↑ CNS drug entry & potential toxicity.
Pediatric Pharmacokinetics & Dynamics - Metabolize, Excrete & Respond
-
Metabolism (Liver): Immature pathways in neonates.
- Phase I (CYP450s): Activity generally ↓.
- CYP3A4, CYP1A2: Slow maturation.
- CYP2D6: Variable; can exceed adult levels in childhood.
- Phase II (Conjugation):
- Glucuronidation (UGT): Markedly ↓. 📌 Risk: Toxicities (e.g., chloramphenicol).
- Sulfation (SULTs): Relatively more developed.
- ⭐ > Glucuronidation pathway is significantly immature in neonates, leading to risks like Gray Baby Syndrome with chloramphenicol due to deficient UGT activity.
- Phase I (CYP450s): Activity generally ↓.
-
Excretion (Kidney): Immature renal function.
- GFR: Neonates ~20-40% adult; adult levels by 6-12 months.
- Tubular secretion & reabsorption: ↓, prolongs drug half-life.
-
Pharmacodynamics (Response):
- Receptor sensitivity & density: Altered.
- Blood-Brain Barrier (BBB): ↑ Permeability.
- Body Composition: ↑ Total Body Water (TBW), ↓ Body Fat.
Pediatric Dose Calculation - Formulas & Safety First
- Goal: Safe, effective drug levels in children, considering unique physiology.
- Dosing Methods & Formulas:
- Weight-based (e.g., Clark's Rule): $Pediatric Dose = Adult Dose \times \frac{Weight (kg)}{70}$
- Age-based (Less accurate):
- Young's Rule (>1yr): $Adult Dose \times \frac{Age (yrs)}{Age (yrs) + 12}$
- Fried's Rule (<2yr): $Adult Dose \times \frac{Age (months)}{150}$
- BSA-based (Often most accurate): $Adult Dose \times \frac{Child's BSA (m²)}{1.73 m²}$
- Mosteller Formula: $BSA (m^2) = \sqrt{\frac{Height (cm) \times Weight (kg)}{3600}}$
- Safety First: Prioritize mg/kg or BSA. Double-check calculations. Monitor vigilantly.
⭐ BSA-dosing is superior for accuracy with narrow therapeutic index drugs (e.g., chemotherapy, certain renally excreted drugs).
High‑Yield Points - ⚡ Biggest Takeaways
- Body Surface Area (BSA) is the most accurate method for pediatric dose calculation.
- Neonates exhibit ↓ GFR, immature liver enzymes (e.g., glucuronidation), and ↑ total body water.
- ↓ Plasma protein binding in neonates can lead to ↑ free drug concentrations.
- Key drugs to avoid: Sulfonamides (kernicterus), Tetracyclines (teeth/bone), Aspirin (Reye's syndrome), Chloramphenicol (Gray baby syndrome).
- CYP450 enzyme activity matures gradually, significantly impacting drug metabolism.
- Age-based formulas (e.g., Young's Rule, Clark's Rule) are less reliable than BSA-based dosing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

