Poisoning Principles - Detox Blueprint
1. Initial Management:
- Stabilize: ABCs (Airway, Breathing, Circulation), Vitals, GCS.
- History: 📌 AMPLE (Allergies, Medications, Past history, Last meal, Events).
- Examination: Identify toxidromes.
2. Decontamination (Reduce Absorption):
- Activated Charcoal: 1g/kg PO/NG. Contra: corrosives, hydrocarbons, poor GI motility, no bowel sounds.
- Gastric Lavage: Within 1 hr for life-threatening ingestions if airway protected. Contra: corrosives, hydrocarbons.
- Whole Bowel Irrigation (WBI): Polyethylene glycol for body packers, sustained-release/enteric-coated drugs.
3. Enhanced Elimination (Increase Excretion):
- Forced Diuresis: Alkaline (e.g., salicylates, phenobarbital) using $NaHCO_3$ for ion trapping ($pH = pKa + log([A^-]/[HA])$).
- Hemodialysis: For low MW, low Vd, water-soluble toxins (methanol, ethylene glycol, salicylates, lithium).
- Hemoperfusion: For drugs binding charcoal (theophylline, carbamazepine, phenobarbital).
⭐ Activated charcoal is not effective for heavy metals (Pb, Hg, As), iron, lithium, alcohols, and corrosives.
Toxidrome Titans - Syndrome Sleuth
Recognize patterns for diagnosis. Key differentiating features:
| Toxidrome | CNS | Pupils | Vitals | Skin | Bowel Sounds | Other / Secretions | Examples |
|---|---|---|---|---|---|---|---|
| Opioid | ↓Resp, Coma | Miosis | ↓HR,↓BP,↓RR,↓T | - | ↓ | - | Morphine |
| Sympathomimetic | Agitation | Mydriasis | ↑HR,↑BP,↑T | Diaphoretic | ↑ | - | Cocaine |
| Cholinergic | Confusion | Miosis | Bradycardia | Diaphoretic | ↑ | ↑↑ (📌DUMBELS), Killer Bs | Organophosphates |
| Anticholinergic | Delirium | Mydriasis | ↑HR,↑T | Hot,Dry,Red | ↓ | ↓↓ Dry (📌"Mad as...") | Atropine |
| Sedative-Hypnotic | Depression | Variable | ↓RR,↓BP (norm) | - | ↓ | - | Benzodiazepines |
- 📌 Anticholinergic: "Mad as a hatter (delirium), Blind as a bat (mydriasis), Red as a beet (flushed), Hot as a hare (hyperthermia), Dry as a bone (dry)."
⭐ Miosis is a key feature differentiating opioid toxidrome from sedative-hypnotic toxidrome (which usually has variable pupils, often normal).
Common Culprits - Poison Parade
-
Organophosphates (OPC)
- Mech: Irreversible AChE inhibitor → ↑ACh.
- Features: 📌 DUMBELS/SLUDGE-M (Cholinergic crisis); muscle fasciculations, paralysis.
- Antidote: Atropine (2-5 mg IV q 5-15 min); Pralidoxime (PAM) (1-2 g IV).
- Mgmt: Decontamination, airway support.
-
Paracetamol (Acetaminophen)
- Mech: Toxic metabolite NAPQI depletes glutathione → liver damage.
- Features: N/V (early); ↑LFTs, jaundice, encephalopathy (late).
- Antidote: N-acetylcysteine (NAC) IV loading dose 150 mg/kg.
- Mgmt: Activated charcoal (<4h). Rumack-Matthew nomogram ($[Paracetamol]_{serum}$ vs. time).
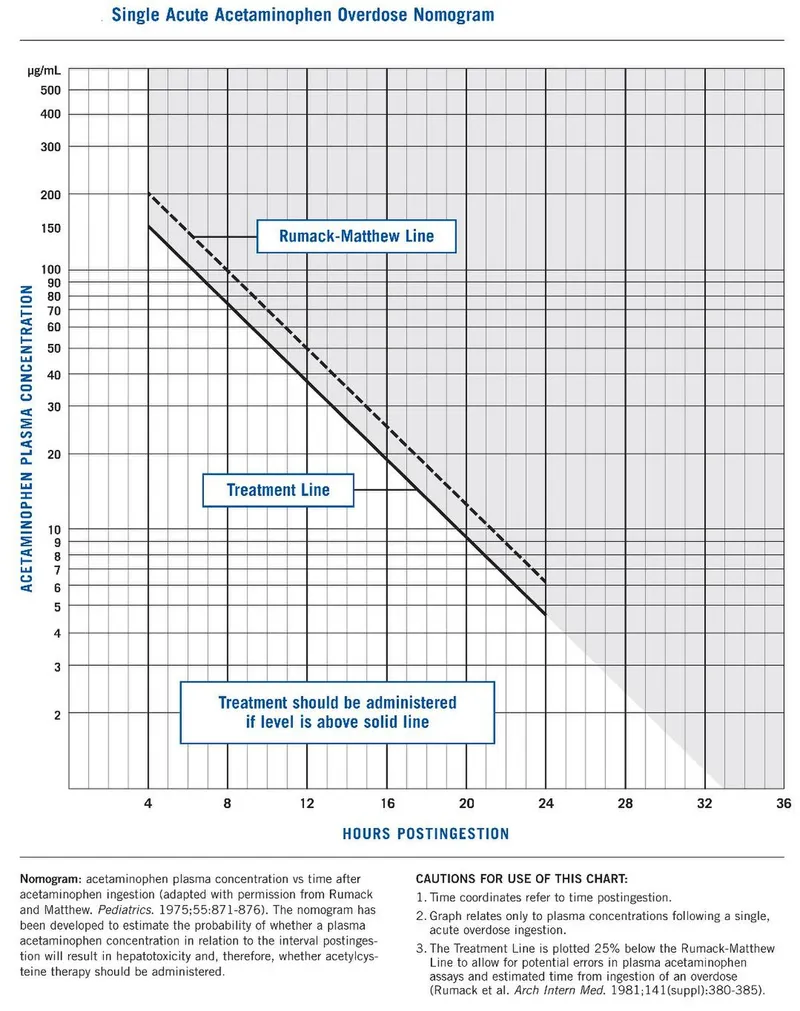
⭐ In paracetamol poisoning, N-acetylcysteine is most effective if given within 8 hours of ingestion.
-
Opioids
- Mech: Mu-receptor agonist.
- Features: Triad: miosis, respiratory depression, ↓LOC.
- Antidote: Naloxone (0.4-2 mg IV/IM/SC).
- Mgmt: Airway, ventilation.
-
Salicylates (Aspirin)
- Mech: Uncouples oxidative phosphorylation, resp. center stimulation.
- Features: Tinnitus, hyperthermia, tachypnea; resp. alkalosis → metabolic acidosis. 📌 MUDPILES.
- Antidote: Sodium bicarbonate (urinary alkalinization, target urine pH 7.5-8.0).
- Mgmt: IV fluids, glucose. Hemodialysis if severe (e.g., level >80-100 mg/dL acute).
Antidote Arsenal - Remedy Roster
| Antidote | Poison(s) | MoA | Dose/Note |
|---|---|---|---|
| N-acetylcysteine | Paracetamol | Glutathione precursor, hepatoprotective | 150mg/kg IV (1hr), then 50mg/kg (4hrs) |
| Naloxone | Opioids | Competitive opioid antagonist | 0.4-2mg IV/IM/SC, repeat PRN |
| Flumazenil | Benzodiazepines | GABA-A antagonist | 0.2mg IV (15s), repeat (Max 3mg) ⚠️ |
| Atropine | OPC, Carbamates | Muscarinic antagonist (dries secretions) | 2-5mg IV q5-10min till atropinization |
| Pralidoxime (PAM) | OPC (early) | AChE reactivator (reverses muscle weakness) | 1-2g IV (30min), then infusion |
| $NaHCO_3$ | Salicylates, TCAs | Alkalinization (urine/plasma), $Na^+$ channel blockade (TCAs) | 1-2mEq/kg IV bolus, then infusion |
| Fomepizole/Ethanol | Methanol, Ethylene Glycol | Inhibits alcohol dehydrogenase (prevents toxic metabolites) | Fomepizole: 15mg/kg LD |
| Glucagon | Beta-blocker, CCB OD | $\uparrow cAMP$, bypasses beta-receptors, +ve inotropy/chronotropy | 5-10mg IV bolus, then 1-5mg/hr |
High‑Yield Points - ⚡ Biggest Takeaways
- Organophosphate poisoning: Atropine for muscarinic effects, Pralidoxime reactivates cholinesterase.
- Paracetamol poisoning: N-acetylcysteine is the specific antidote, best within 8-10 hours.
- Opioid overdose: Naloxone reverses respiratory depression, miosis, and coma.
- Cyanide poisoning: Treat with hydroxocobalamin or sodium nitrite + sodium thiosulfate.
- Methanol/Ethylene glycol: Fomepizole or ethanol for HAGMA; consider hemodialysis.
- Salicylate toxicity: Mixed acid-base disturbance; manage with alkaline diuresis, hemodialysis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

