Diuretics in HF: The Basics - De-Puffing Power
- Primary Goal: Rapid symptomatic relief from fluid overload (congestion).
- Reduces dyspnea, orthopnea, edema, JVD.
- Mechanism: Promote renal sodium ($Na^+$) & water excretion.
- This ↓ plasma volume, ↓ preload, and ↓ pulmonary congestion.
- Clinical Use: Cornerstone for managing symptoms in acute & chronic HF.
- Crucial for "de-puffing" by removing excess body fluid.
- Generally no standalone mortality benefit (MRAs are an exception).
⭐ Diuretics offer the quickest relief of congestive symptoms in acute HF.
Loop Diuretics - Fluid Fighters
- MoA: Inhibit Na-K-2Cl cotransporter in thick ascending limb (TAL) of Loop of Henle. Most potent diuretics.
- Drugs: Furosemide, Torsemide, Bumetanide.
- Ethacrynic acid: for sulfa allergy (⚠️ higher ototoxicity risk).
- Use in HF: Rapid symptomatic relief of fluid overload (e.g., pulmonary/peripheral edema), reduces preload.
- IV for acute decompensation; oral for chronic management.
- Key Adverse Effects:
- Hypokalemia (monitor K+!), hypomagnesemia, hypocalcemia.
- Ototoxicity (dose-dependent, rapid IV admin).
- Hyperuricemia, dehydration.
- Dosing (Furosemide example): Oral 20-80 mg daily; IV 20-40 mg initial dose.
- Resistance: Consider ↑ dose, IV infusion, or add thiazide (sequential blockade).
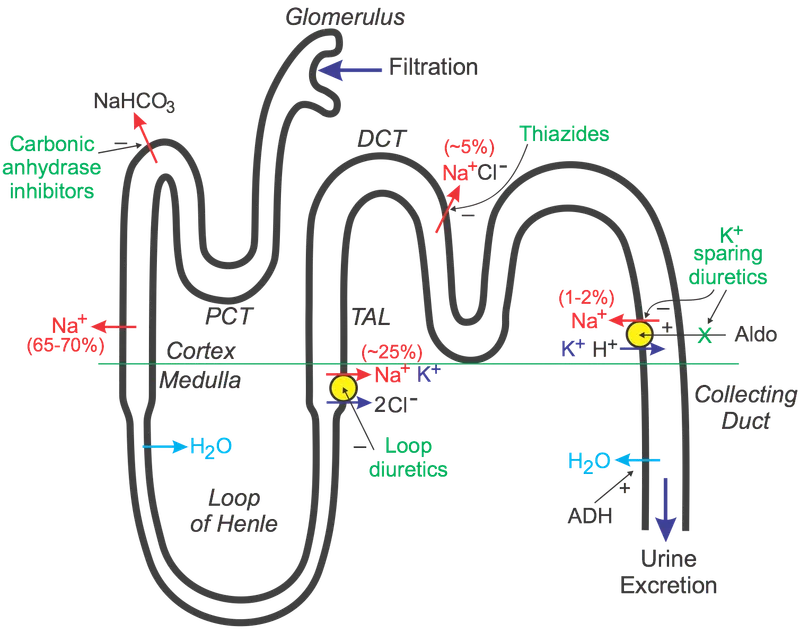
⭐ Loop diuretics are first-line for rapid symptomatic relief in acute decompensated heart failure (ADHF) with signs of fluid overload.
Thiazides & MRAs - Combo Kings
- Thiazides (e.g., Hydrochlorothiazide, Chlorthalidone, Metolazone)
- Mechanism: Inhibit Na-Cl cotransporter in Distal Convoluted Tubule (DCT).
- Role in HF:
- Synergistic effect with loop diuretics (sequential nephron blockade) to overcome diuretic resistance.
- Metolazone particularly useful in advanced HF or renal impairment.
- Adverse Effects: Hypokalemia, hyponatremia, hyperuricemia, hyperglycemia.
- Mineralocorticoid Receptor Antagonists (MRAs) (e.g., Spironolactone, Eplerenone)
- Mechanism: Aldosterone antagonists; K+-sparing diuretics. Act on principal cells of collecting duct.
- Role in HFrEF:
- Reduce mortality & morbidity (NYHA Class II-IV with LVEF ≤ 35%; or post-MI, LVEF ≤ 40% + HF symptoms/DM).
- Decrease cardiac fibrosis & remodeling.
- Adverse Effects: Hyperkalemia (monitor K+ & renal function). Spironolactone: gynecomastia. Eplerenone: more selective, fewer endocrine effects.
⭐ MRAs (Spironolactone, Eplerenone) are the only diuretics demonstrating mortality benefit in chronic HFrEF.
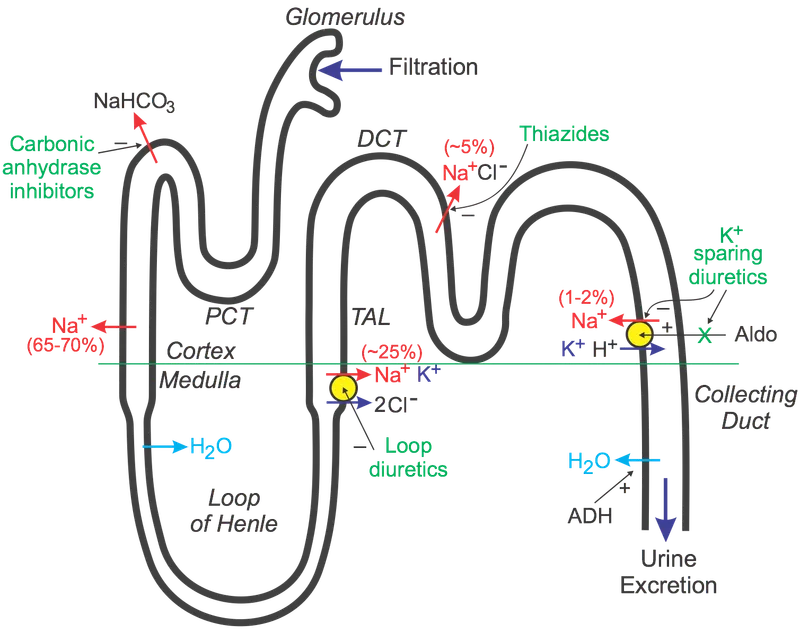
Diuretic Strategy & Resistance - The Flow Showdown
-
Goal: Achieve euvolemia, relieve congestion. Monitor daily weight, I/O, electrolytes (K+, Mg2+), renal function.
-
Initial: Loop diuretics (furosemide, torsemide). Titrate to response.
-
Diuretic Resistance: Persistent congestion despite escalating loop diuretic doses (e.g., > 80-160 mg IV furosemide equivalent/day).
- Causes: ↓Renal perfusion, nephron adaptation (distal hypertrophy), ↓oral absorption (gut edema).
-
Overcoming Resistance:
- Sequential Blockade: Add thiazide (e.g., metolazone 5-10 mg) 30 min before loop.
- MRAs (spironolactone, eplerenone) also useful, esp. if hypokalemia.
⭐ In diuretic resistance, adding a thiazide like metolazone 30 minutes before a loop diuretic can significantly enhance natriuresis by blocking sequential sodium reabsorption sites.
High‑Yield Points - ⚡ Biggest Takeaways
- Loop diuretics (e.g., furosemide) are first-line for symptomatic relief of volume overload in acute & chronic HF.
- Mechanism: Inhibit Na-K-2Cl cotransporter in thick ascending limb.
- Aldosterone antagonists (spironolactone, eplerenone) reduce mortality in HFrEF (NYHA II-IV).
- Thiazides are used for mild HF or synergistically with loops for refractory edema.
- Key adverse effects: hypokalemia (loops/thiazides), hyperkalemia (K-sparing), ototoxicity (loops), azotemia.
- Manage diuretic resistance with combination therapy or dose escalation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

