Cholinergic Antagonists: Intro & Classes - ACh Blockade Basics
- Definition: Drugs competitively blocking acetylcholine (ACh) at muscarinic/nicotinic receptors.
- Antimuscarinics also termed parasympatholytics.
- ACh Blockade Basics:
- Prevent ACh binding, inhibiting cholinergic transmission.
- Effects are generally opposite to those of cholinomimetics.
- Major Classes:
- Antimuscarinic Agents: Selectively block muscarinic receptors (e.g., Atropine).
- Antinicotinic Agents:
- Ganglion Blockers (NN blockade).
- Neuromuscular Blockers (NM blockade).
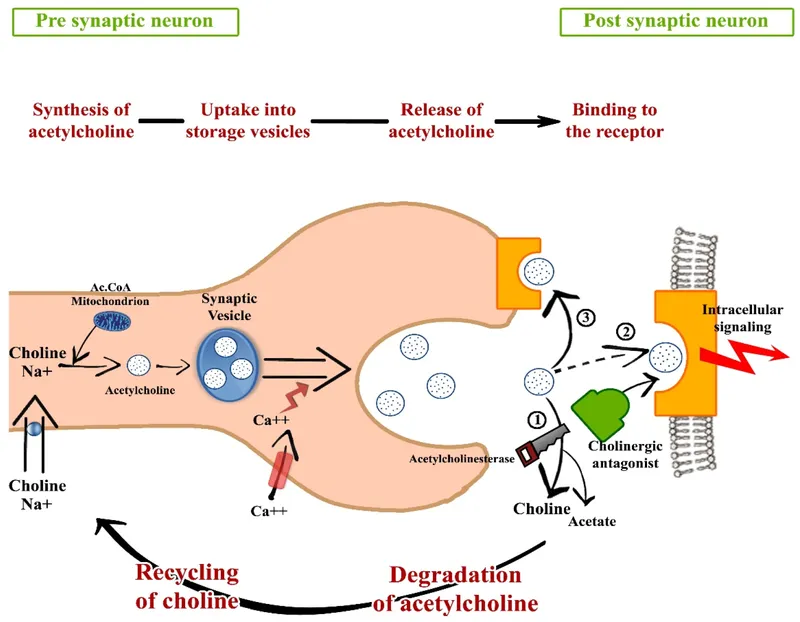
⭐ Atropine is a non-selective muscarinic antagonist; it blocks M1, M2, and M3 receptors.
Antimuscarinics: Actions & Uses - Parasympathetic Pause
- Core Action: Competitive blockade of muscarinic receptors (M1-M5) → ↓parasympathetic tone.
- 📌 Effects: Dry mouth, blurred vision, tachycardia, constipation, urinary retention, "atropine fever" (anhidrosis).
- CNS:
- Sedation, anti-motion sickness (Scopolamine).
- Parkinsonism (Benztropine, Trihexyphenidyl): ↓tremor, rigidity.
- Eye:
- Mydriasis, cycloplegia. Uses: Fundoscopy (Tropicamide), uveitis.
- ⚠️ Caution: Angle-closure glaucoma (↑IOP).

- CVS:
- Tachycardia (blocks M2). Uses: Symptomatic bradycardia, AV block (Atropine).
- Respiratory:
- Bronchodilation, ↓secretions. Uses: COPD, Asthma (Ipratropium, Tiotropium - inhaled).
- GIT:
- ↓Salivation, ↓motility (antispasmodic), ↓acid. Uses: IBS (Dicyclomine), pre-anaesthetic (Glycopyrrolate).
- GUT:
- ↓Bladder contractility. Uses: Overactive bladder (Oxybutynin, Tolterodine), ↓urgency.
- Crucial Use: Atropine in organophosphate poisoning (life-saving).
⭐ In organophosphate poisoning, atropine only blocks muscarinic effects. Pralidoxime is needed to regenerate AChE and reverse nicotinic effects (muscle weakness).
Antimuscarinics: ADRs & Toxicity - Dry Side Dangers
- ADRs (Anticholinergic Effects):
- Dryness: Mouth (xerostomia), eyes (blurred vision, mydriasis, cycloplegia), skin (anhidrosis, flushing).
- Systemic: Tachycardia, urinary retention, constipation.
- CNS: Confusion, delirium, hallucinations (elderly ↑ risk). 📌 "Dry as bone, blind as bat, red as beet, mad as hatter, hot as hare."
- Toxicity (Atropine Poisoning): Exaggerated ADRs; hyperthermia, agitation, seizures, coma.
- Management: Supportive care (ABC, cooling). Physostigmine for severe toxicity (monitor closely).
⭐ Physostigmine (cholinesterase inhibitor) reverses central & peripheral antimuscarinic effects; use cautiously due to potential for bradycardia/seizures.
- Contraindications: Narrow-angle glaucoma, benign prostatic hyperplasia (BPH), obstructive uropathy/GIT disease, tachyarrhythmias.

Nicotinic Antagonists: NMBs - Muscle Relax Masters
- Neuromuscular Blockers (NMBs): Act at nicotinic (Nm) receptors of the neuromuscular junction (NMJ).
- Classification & Mechanism:
- Depolarizing:
- Example: Succinylcholine
- MOA: Phase I (persistent depolarization, initial fasciculations), then Phase II (desensitization block, flaccid paralysis).
- Rapid onset, short duration.
- Non-Depolarizing (Competitive):
- Examples: "-curoniums" (Pancuronium, Vecuronium, Rocuronium); "-curiums" (Atracurium, Cisatracurium).
- MOA: Compete with Acetylcholine (ACh) for Nm receptors.
- Reversible by AChE inhibitors (e.g., Neostigmine, Sugammadex for Rocuronium/Vecuronium).
- Depolarizing:
- Clinical Uses: Anesthesia for surgical relaxation, endotracheal intubation, mechanical ventilation.
- Key Points:
- Atracurium: Undergoes Hofmann elimination (useful in renal/hepatic failure).
- Cisatracurium: Less histamine release than Atracurium.

⭐ Succinylcholine can cause significant hyperkalemia in patients with burns, crush injuries, or upper motor neuron lesions, potentially leading to cardiac arrest. Use is contraindicated >24-48 hours post-injury until risk subsides (months).
High‑Yield Points - ⚡ Biggest Takeaways
- Atropine: prototype muscarinic antagonist; treats bradycardia, organophosphate poisoning.
- Antimuscarinic toxidrome: "Dry as a bone, blind as a bat, red as a beet, mad as a hatter, hot as a hare".
- Ipratropium/Tiotropium: inhaled for COPD/asthma; poor systemic absorption.
- Scopolamine: for motion sickness; preanesthetic use.
- Contraindications: Narrow-angle glaucoma, BPH, bowel obstruction.
- Oxybutynin/Tolterodine/Solifenacin: treat overactive bladder.
- Benztropine/Trihexyphenidyl: for Parkinson's disease and drug-induced EPS.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

