Biliary Atresia - Bile Duct Blues
- Progressive, idiopathic, fibro-obliterative disease of neonatal intrahepatic and/or extrahepatic bile ducts, leading to biliary obstruction.
- Incidence: 1 in 10,000-15,000 live births; more common in East Asia.

- Types (Kasai Classification):
- Type I (~5%): Atresia of common bile duct (CBD); patent proximal ducts.
- Type II (~2%): Atresia of common hepatic duct (CHD).
- IIa: Cystic duct joins patent CHD.
- IIb: Cystic duct joins patent CBD.
- Type III (>90%): Atresia at porta hepatis (most common); no correctable extrahepatic ducts.
- Etiology (multifactorial, exact cause unknown):
- Viral infections (Reovirus 3, CMV).
- Immune-mediated inflammation (e.g., ↑Th1 response).
- Genetic predisposition (e.g., CFC1, ADD3 genes).
- Developmental malformation (e.g., Biliary Atresia Splenic Malformation [BASM] syndrome).
⭐ Type III biliary atresia is the most frequent, accounting for over 90% of cases, and involves atresia of ducts at the porta hepatis.
Biliary Atresia - Jaundice Jigsaw
- Patho: Progressive fibro-obliteration of extrahepatic biliary ducts. Most common: Type III (atresia at porta hepatis, ~90%).
- Classic Triad: Jaundice (conjugated, persistent >2 wks), acholic stools, dark urine.
- Signs: Firm hepatomegaly, failure to thrive (late).
- Labs: ↑ Direct bilirubin, ↑ GGT (key marker), ↑ ALP.
⭐ Kasai portoenterostomy performed before 60 days of life offers the best chance of establishing bile flow and native liver survival.
- Management:
- Kasai (hepatoportoenterostomy): Aim <60-90 days.
- Liver Transplant: If Kasai fails or late diagnosis.
- Supportive: Fat-soluble vitamins (A,D,E,K), UDCA.
- Prognosis: Guarded. 5-year native liver survival post-Kasai: 30-60%.
- Complications: Cholangitis (recurrent), portal HTN, cirrhosis, hepatopulmonary syndrome.
Biliary Atresia - Kasai & Beyond
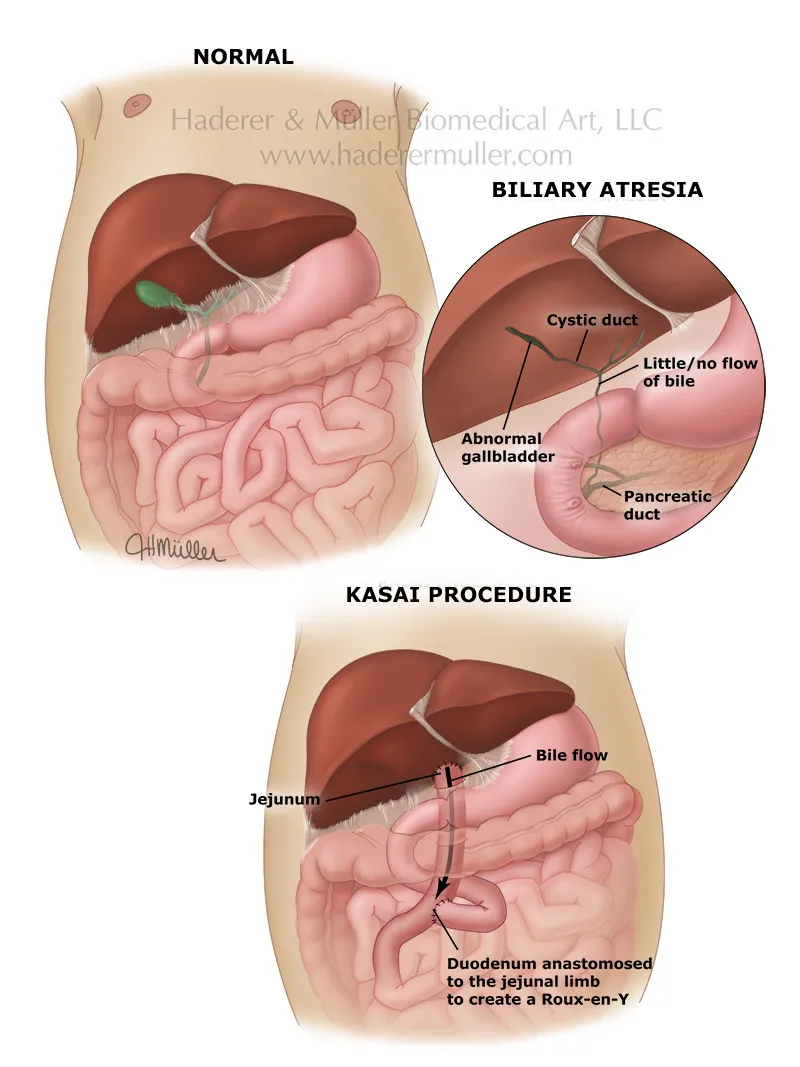
- Kasai Portoenterostomy (Hepatoportoenterostomy):
- Surgical treatment of choice.
- Anastomosis of a Roux-en-Y loop of jejunum to the porta hepatis.
- Goal: Achieve bile drainage.
- Optimal Timing for Kasai:
- Crucial for success: < 60-90 days of life.
- Best outcomes if performed < 45 days.
- Delayed surgery → progressive fibrosis, ↓ poorer prognosis.
- Post-Kasai Management:
- Ursodeoxycholic acid (UDCA) to promote bile flow.
- Fat-soluble vitamins (A, D, E, K) supplementation.
- Prophylactic antibiotics to prevent cholangitis.
- Nutritional support for growth.
- Complications Post-Kasai:
- Recurrent cholangitis (most common).
- Portal hypertension (e.g., varices, ascites).
- Progressive liver fibrosis/cirrhosis.
- Failure to drain bile / Kasai failure.
- Prognosis & Liver Transplantation (LTx):
- Native liver survival: ~30-50% at 5 years post-Kasai.
- Many require LTx by adulthood.
- LTx is definitive for failed Kasai or end-stage liver disease complications.
⭐ Majority of patients with biliary atresia will eventually require liver transplantation, even with an initially successful Kasai procedure.
High‑Yield Points - ⚡ Biggest Takeaways
- Biliary Atresia: Most common surgical cause of neonatal cholestasis; leading indication for pediatric liver transplant.
- Presents with persistent jaundice (>2 weeks), acholic stools, dark urine, and conjugated hyperbilirubinemia.
- Kasai portoenterostomy is the initial palliative surgery.
- Optimal Kasai timing: Before 60-90 days of age for better prognosis.
- Many patients ultimately require liver transplantation despite Kasai.
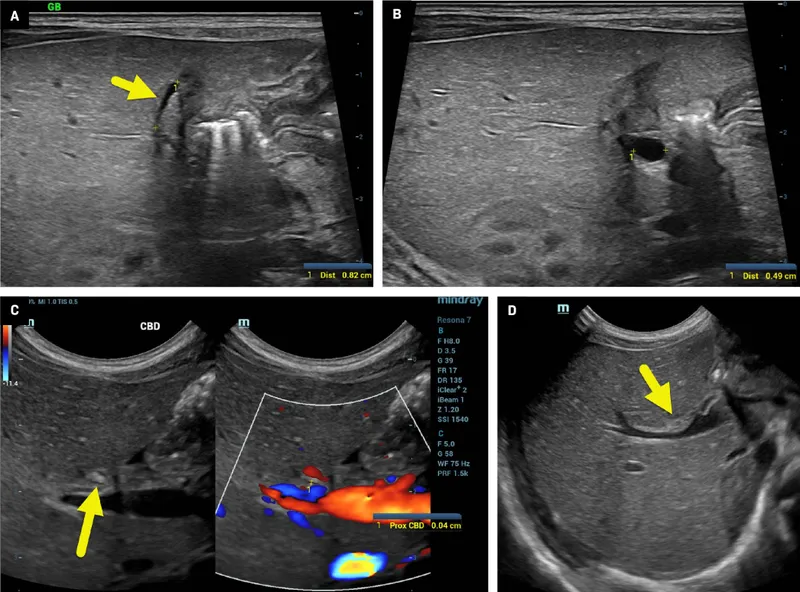
- Intraoperative cholangiogram is diagnostic; triangular cord sign on US is suggestive.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

