Abdominal Wall Defects - Sealed With A Sac
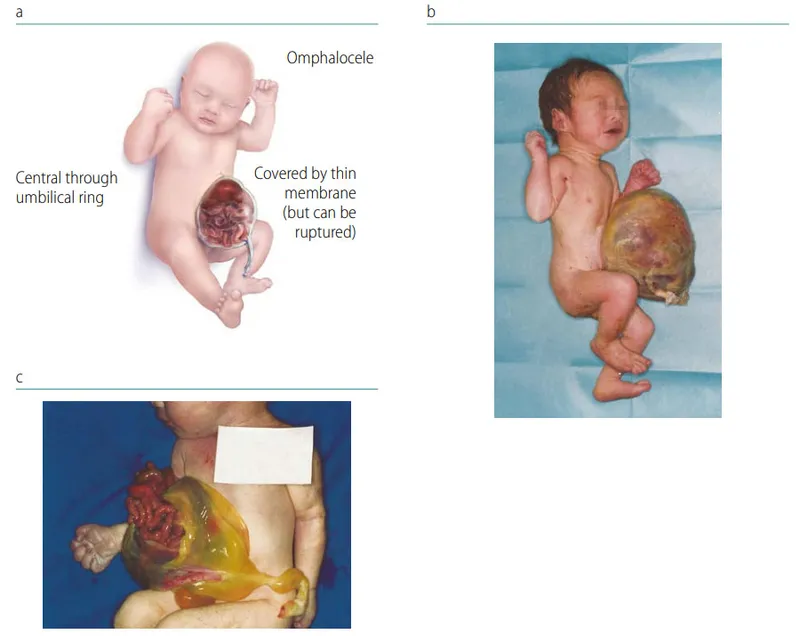
- Omphalocele: Midline defect at umbilical cord insertion; herniated viscera covered by a sac (amnion-peritoneum).
- Embryology: Failure of embryonic midgut to return to abdomen by 10th-12th week.
- Contents: Bowel, frequently liver, spleen.
- Associated Anomalies: Common (~50-70%); crucial to screen.
- Cardiac defects (e.g., VSD, ASD, Tetralogy of Fallot).
- Chromosomal: Trisomies 13 (Patau), 18 (Edwards), 21 (Down).
- Beckwith-Wiedemann syndrome (macroglossia, macrosomia, omphalocele, hypoglycemia).
- Maternal Serum AFP: Typically ↑ elevated.
- Delivery: Vaginal delivery possible for small defects; C-section for large defects or liver herniation to prevent sac rupture.
- 📌 Mnemonic: Omphalocele: Organs in sac, Often Other anomalies, Ombilicus is the site.
⭐ Exam Favourite: Omphalocele's association with chromosomal abnormalities (esp. Trisomy 18, 13) is significantly higher than gastroschisis.
Abdominal Wall Defects - Guts Out, No Sac!
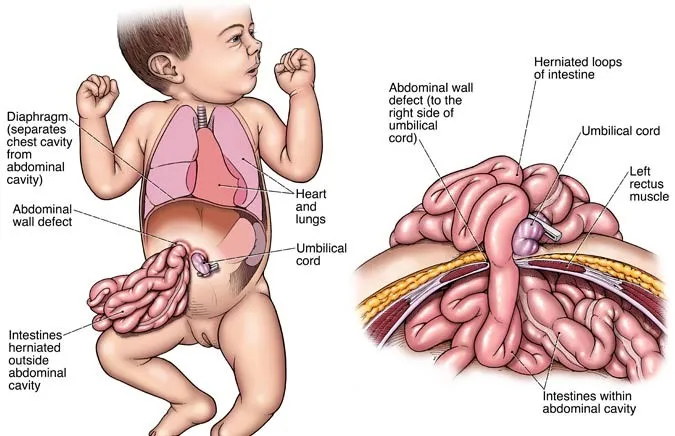
- Definition: Full-thickness paraumbilical abdominal wall defect with evisceration of abdominal contents.
- Embryology: Vascular accident theory (e.g., involution of right umbilical vein or omphalomesenteric artery).
- Location: Paraumbilical, typically to the right of a normally inserted umbilical cord.
- Covering Sac: Absent; "Guts Out, No Sac!"
- Contents: Primarily bowel (small & large intestine); rarely liver or stomach.
- Bowel Appearance: Exposed to amniotic fluid → thickened, edematous, matted, foreshortened, often with an inflammatory peel.
- Associated Anomalies: Less common than omphalocele (~10-15%); primarily intestinal atresia/stenosis, malrotation.
- Maternal AFP: Markedly elevated (↑↑) due to exposed bowel.
- Maternal Factors: Young maternal age (<20 years), smoking, vasoconstrictor drug use.
- 📌 Mnemonic: Gastroschisis: Guts out, Generally to the Right, Generally good prognosis if isolated.
⭐ Gastroschisis is NOT associated with chromosomal abnormalities, unlike omphalocele, and generally has a better prognosis if isolated without significant bowel damage or atresia.
Abdominal Wall Defects - Spot The Difference!
| Feature | Omphalocele | Gastroschisis |
|---|---|---|
| Location | Midline, umbilical | Right of umbilicus (paraumbilical, full-thickness defect) |
| Sac | Present (amnion-peritoneum membrane) | Absent |
| Cord Insertion | Onto sac | Normal, lateral to defect |
| Contents | Bowel, liver, spleen | Bowel, rarely stomach/gonads; liver rare |
| Bowel Appearance | Normal | Edematous, matted, inflamed, foreshortened |
| Associated Anomalies | Common (50-70%), cardiac, chromosomal (e.g., Trisomy 13, 18, Beckwith-Wiedemann) | Less common (10-15%), intestinal atresia |
| Maternal AFP | ↑ | ↑↑ (higher than omphalocele) |
| Prognosis | Depends on associated anomalies | Depends on bowel damage, better if isolated |
📌 Mnemonic: Omphalocele = Outside but Organized (in sac); Gastroschisis = Guts Spilling (no sac).
Abdominal Wall Defects - Tiny Tummy Fix-Up
- Prenatal Management:
- Diagnosis via USG.
- Parental counseling.
- Delivery planning (tertiary center).
- Immediate Postnatal Care:
- Thermoregulation (prevent heat loss).
- IV fluids: 1.5-2x maintenance.
- Sterile covering (bowel bag) for viscera.
- NG decompression (prevent distension).
- IV antibiotics (prophylaxis).
- Surgical Repair:
- Primary closure (small defect, low tension).
- Staged (Silo) for large defects.
- Post-operative Care:
- TPN initially.
- Gradual enteral feeds.
⭐ Gastroschisis typically occurs to the right of an intact umbilical cord and lacks a protective sac, leading to significant fluid and heat loss compared to omphalocele which has a sac and is midline.
High‑Yield Points - ⚡ Biggest Takeaways
- Gastroschisis: Right of umbilicus, no sac, exposed bowel; associated with bowel atresia.
- Omphalocele: Midline defect at umbilical base, sac present (amnion/peritoneum), contains organs.
- Both show ↑ maternal serum AFP.
- Omphalocele frequently linked to chromosomal abnormalities (e.g., Trisomies, Beckwith-Wiedemann).
- Gastroschisis often isolated, generally better prognosis if no severe bowel damage.
- Initial management: Silo for gastroschisis; protect sac in omphalocele, often staged repair.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

