Definition & Pathophysiology - Drowning Depths
- Definition (WHO): Respiratory impairment from submersion/immersion in liquid.
- 'Near-drowning' obsolete; use 'drowning' with outcome (fatal/non-fatal).
- Epidemiology: Highest risk in toddlers (1-4 yrs) and adolescent males.
- Pathophysiology:
- Primary Insult: Hypoxia.
- Laryngospasm ('dry'): ~10-15%; glottic closure, no initial aspiration.
- Aspiration ('wet'): ~85-90%; fluid in lungs.
- Water Type:
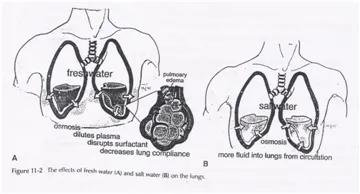
- Freshwater (hypotonic): Surfactant washout $\rightarrow$ atelectasis.
- Saltwater (hypertonic): Alveolar fluid influx $\rightarrow$ edema.
- Hypoxia is the dominant factor regardless of water type.
- Systemic: CNS (HIBI), CVS (arrhythmias), Resp (ARDS), Renal (ATN), metabolic acidosis.
⭐ The most significant consequence of drowning is hypoxic brain injury (HIBI), determining long-term outcome.
Clinical Features & Assessment - Gasping Signs
- Spectrum: Asymptomatic to cardiorespiratory arrest.
- Respiratory: Cough, dyspnea, tachypnea, cyanosis. Crackles, wheezes, apnea.
- Neurological: Altered sensorium (GCS), seizures. Assess for Hypoxic Ischemic Brain Injury (HIBI).
- Cardiovascular: Tachycardia/bradycardia, hypotension, arrhythmias.
- Hypothermia: Common, especially in children.
- Associated injuries: Head/cervical spine trauma (diving).
- Initial Assessment: ABCDE approach.
- Key history: Duration of submersion, water temp, type of water, bystander CPR.
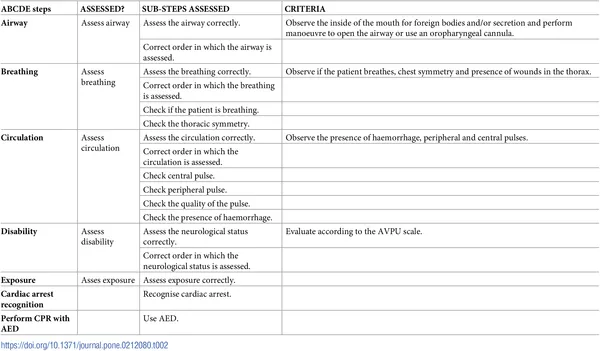
- Key history: Duration of submersion, water temp, type of water, bystander CPR.
⭐ Patients asymptomatic with normal oxygen saturation and lung sounds for 6-8 hours of observation are unlikely to develop significant respiratory complications.
Management - Rescue & Revive Protocol
-
Pre-hospital:
- Safe rescue from water.
- Immediate CPR: Compressions + Breaths.
- C-spine immobilization prn (if trauma suspected).
- Remove wet clothes, prevent heat loss.
-
ED & ICU Management:
- Oxygenation & Ventilation:
- Initiate high-flow O2. Consider CPAP/BiPAP for respiratory distress.
- For ARDS: Intubation & Lung Protective Ventilation (low tidal volume, optimal PEEP). PEEP is crucial.
- Circulation:
- Cautious IV fluid resuscitation, guided by clinical assessment.
- Vasopressors for persistent hypotension.
- Hypothermia:
- Gradual rewarming to normothermia.
- Consider therapeutic hypothermia (32-36°C) for neuroprotection if post-cardiac arrest (note: evidence in drowning is limited).
- Monitoring:
- Continuous: cardiac rhythm, SpO2, ETCO2, core temperature.
- Serial: neuro status, ABG, electrolytes, lactate.
- Avoid:
- NO routine prophylactic antibiotics.
- NO routine steroids. Surfactant not routinely recommended.
- Oxygenation & Ventilation:

⭐ Early and effective bystander CPR is one of the most important factors improving outcomes in pediatric drowning.
Prognosis & Complications - After the Splash
- Poor Prognostic Factors:
- Submersion duration >5-10 minutes.
- Time to effective BLS/ALS >10 minutes.
- Severe hypothermia on admission (unless rapid cooling, preserved circulation).
- Persistent apnea, CPR needed in ED.
- Glasgow Coma Scale (GCS) ≤5 on presentation.
- Severe metabolic acidosis (arterial pH <7.0-7.1).
- Fixed and dilated pupils.
- Complications:
- Acute Respiratory Distress Syndrome (ARDS).
- Hypoxic-Ischemic Brain Injury (HIBI): cerebral edema, seizures, long-term neurological deficits.
- Aspiration pneumonia.
- Multiple Organ Dysfunction Syndrome (MODS).
- Electrolyte imbalances (rarely severe).
⭐ The neurological status of the child after resuscitation is the most critical determinant of long-term prognosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Hypoxia is the central pathophysiological event, leading to multi-organ dysfunction.
- Pulmonary complications (ARDS, surfactant inactivation, aspiration pneumonitis) are critical.
- Neurological outcome (cerebral hypoxia/edema) is the primary determinant of long-term morbidity.
- Immediate bystander CPR and early advanced airway management are crucial for survival.
- Manage hypothermia aggressively; core rewarming for temperatures <32°C.
- Prophylactic antibiotics and corticosteroids are not routinely indicated post-submersion.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

