Principles of Pediatric Chemotherapy - Tiny Patients, Big Differences
- Pediatric physiology alters drug ADME (Absorption, Distribution, Metabolism, Excretion).
- Dosing: Primarily Body Surface Area (BSA) based ($mg/m^2$).
- Carboplatin: Calvert formula (Dose = Target AUC x (GFR + 25)).
- Generally higher chemo tolerance & tumor sensitivity vs. adults.
- Key focus: Minimizing long-term effects (growth, neurocognitive, fertility, secondary cancers).
- Aggressive supportive care vital (hydration, antiemetics, G-CSF).
- Multidisciplinary team (MDT) approach is crucial.
⭐ Pediatric cancers often show higher cure rates (e.g., ALL >80-90%) and better tolerance to intensive chemotherapy than adult cancers, but have a unique malignancy spectrum and long-term sequelae.
Principles of Pediatric Chemotherapy - Little Heroes' Weapons
- Pediatric cancers often highly chemosensitive. Goal: Cure with minimal long-term effects.
- Targets rapidly dividing cells. Combination regimens are standard.
- Key principles: cell cycle specificity, dose intensity, minimizing toxicity.
- 📌 Cell Cycle: M-phase (Vinca), S-phase (Antimetabolites, Etoposide), G2 (Bleomycin). Non-specific: Alkylating, Anthracyclines.

| Drug Class | MoA | Examples | Uses | Toxicities |
|---|---|---|---|---|
| Alkylating Agents | Cross-link DNA | Cyclophosphamide | Leukemias, lymphomas, solid tumors | Myelosuppression, hemorrhagic cystitis, 2° Malign |
| Antimetabolites | Block DNA/RNA synthesis | Methotrexate, 6-MP | Leukemias (ALL), lymphomas | Myelosuppression, mucositis, hepatotoxicity |
| Anthracyclines | DNA intercalation, Topo II inh., radicals | Doxorubicin | Leukemias, lymphomas, sarcomas, Wilms | Cardiotoxicity (cumulative), myelosuppression |
| Vinca Alkaloids | Inhibit microtubule assembly (M-phase) | Vincristine | Leukemias, lymphomas, solid tumors | Neurotoxicity, constipation, BM sparing |
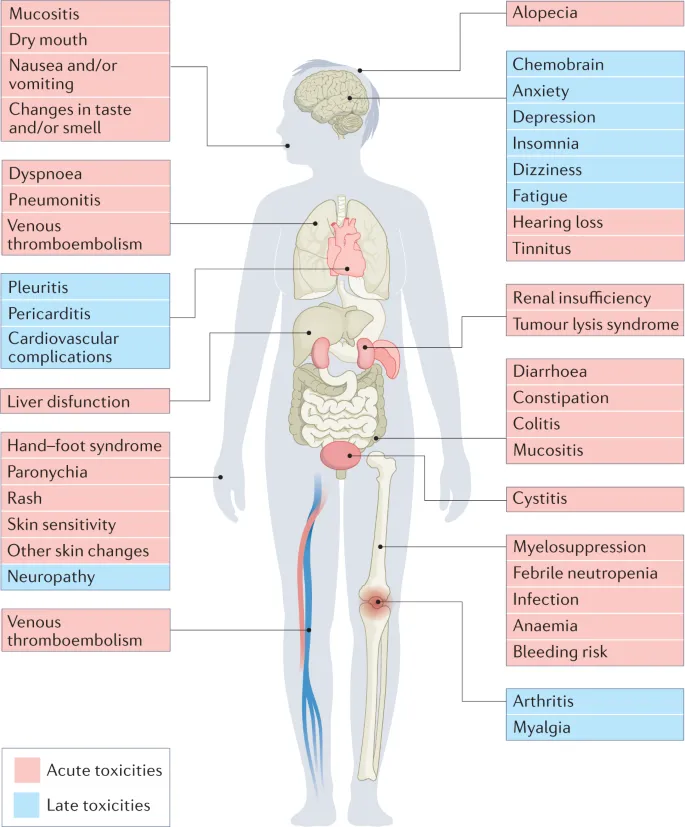
Principles of Pediatric Chemotherapy - Side Effect Battles
Chemotherapy targets rapidly dividing cells, affecting cancer and healthy tissues. Managing side effects is vital.
- Acute: Myelosuppression, nausea/vomiting, mucositis.
- Organ-Specific: Cardiac, renal, neurotoxicity.
- Long-Term: Growth issues, secondary cancers, infertility.
Key Side Effects & Management:
| System/Toxicity | Key Drugs | Peds Notes | Management Highlights |
|---|---|---|---|
| Myelosuppression | Most chemo | ANC < 500/µL critical | G-CSF, transfusions |
| Nausea/Vomiting | Cisplatin, Doxo | High anticipatory | Ondansetron, Aprepitant |
| Mucositis | MTX, 5-FU | Pain, poor nutrition | Hygiene, cryotherapy |
| Hemorrhagic Cystitis | Cyclophos, Ifos | Acrolein toxicity | Mesna, hydration |
| Cardiotoxicity | Anthracyclines | Cumulative dose | Dexrazoxane, LVEF monitoring |
| Neurotoxicity | Vincristine, Cisplatin | Foot drop (V), Ototoxic (Cis) 📌 CisPLATin | Dose adjust |
| Nephrotoxicity | Cisplatin, MTX | Monitor GFR | Hydration, Leucovorin (MTX) |
| Tumor Lysis (TLS) | ALL, Burkitt's | Metabolic emergency | Rasburicase, hydration |
Management of Febrile Neutropenia:
Principles of Pediatric Chemotherapy - Dose & Future Watch
- Dosing:
- Primarily Body Surface Area (BSA): $\text{BSA (m}^2\text{) = } \sqrt{(\text{Height (cm)} \times \text{Weight (kg)}) / 3600}$.
- Carboplatin: Calvert formula $\text{Dose (mg) = Target AUC} \times \text{(GFR + 25)}$.
- Age/weight bands for infants.
- Pediatric Pharmacokinetics:
- ↑ GFR, ↑ metabolism (MTX, cyclophosphamide).
- Larger Vd (water-soluble drugs), ↓ protein binding.
- Future Watch (Late Effects):
- Secondary malignancies (e.g., AML post-etoposide).
- Organ toxicities: cardiac (anthracyclines), pulmonary (bleomycin), renal (cisplatin), neuro (vincristine).
- Endocrine: growth issues, infertility.
- Long-term surveillance crucial.
⭐ Anthracyclines (e.g., Doxorubicin) cause dose-dependent cardiotoxicity, potentially years later, requiring long-term cardiac follow-up.
High‑Yield Points - ⚡ Biggest Takeaways
- BSA-based dosing is standard for most pediatric chemotherapy.
- Children exhibit higher chemosensitivity due to rapid cell proliferation.
- Altered PK/PD in children significantly impacts drug efficacy and toxicity.
- Long-term sequelae, including secondary malignancies and organ damage, are critical.
- Sanctuary sites (CNS, testes) often require specific therapeutic approaches.
- Aggressive supportive care is vital for managing treatment toxicities.
- Pediatric cancers show a unique spectrum (leukemias, lymphomas, embryonal tumors).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

