Neuromuscular Disorders - Wobbly Infant Workup
- History: Onset (birth, later), progression (static, progressive), milestones, family Hx.
- Examination: Tone (hypo/hypertonia), power (MRC scale), reflexes (absent, brisk), fasciculations, contractures, dysmorphism.
- Key Investigations:
- Creatine Kinase (CK): ↑ in muscular dystrophies.
- EMG/NCS: Differentiates myopathy vs. neuropathy.
- Genetic testing: SMA, DMD.
- Muscle biopsy: Specific dystrophies, myopathies.

⭐ Spinal Muscular Atrophy (SMA) Type 1 (Werdnig-Hoffmann) is the most common genetic cause of infant mortality; presents with severe hypotonia & weakness before 6 months.
- Red Flags: Rapid progression, respiratory distress, feeding difficulties, absent reflexes.
Neuromuscular Disorders - Motor Neuron Mayhem
- Spinal Muscular Atrophy (SMA)
- AR; SMN1 gene (Chr 5q) defect → anterior horn cell degeneration.
- LMN signs: Progressive symmetric weakness (proximal > distal), hypotonia, areflexia, tongue fasciculations.
- Type 1 (Werdnig-Hoffmann): Severe. Onset <6 months, death <2 years (untreated).
⭐ SMA Type 1: Classic "floppy baby", frog-leg posture; never sits.
- Rx: Nusinersen, Risdiplam, Onasemnogene abeparvovec.
- Poliomyelitis
- Poliovirus (Enterovirus). Fecal-oral. Infects anterior horn cells.
- Acute asymmetric flaccid paralysis, fever, myalgia. Sensation preserved.
- CSF: Early lymphocytic pleocytosis, later ↑protein, normal glucose.
- Prevention: IPV (Salk) & OPV (Sabin) vaccines.

Neuromuscular Disorders - Muscle Meltdown March
- Duchenne Muscular Dystrophy (DMD)
- X-linked recessive; Dystrophin absence.
- Onset 2-3 yrs; Gower's sign; calf pseudohypertrophy.
- Wheelchair by ~12 yrs; death by ~20s (respiratory/cardiac). ↑ CK.
- Becker Muscular Dystrophy (BMD)
- X-linked recessive; Dystrophin abnormal/reduced. Milder, later onset.
- Spinal Muscular Atrophy (SMA)
- Autosomal recessive; SMN1 gene mutation.
- LMN signs: hypotonia, weakness, fasciculations, absent reflexes.
- Type 1 (Werdnig-Hoffmann): severe, onset <6 months.
- Myasthenia Gravis (Juvenile)
- Autoimmune; ACh receptor antibodies.
- Fluctuating weakness, ptosis, diplopia; worse with exertion.
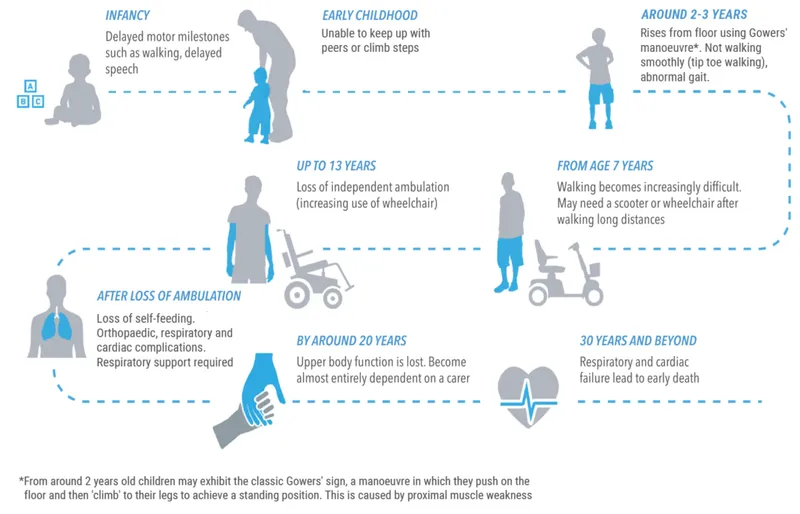
⭐ DMD is characterized by progressive proximal muscle weakness, with Gower's sign being a classic early indicator due to pelvic girdle muscle weakness. Calf pseudohypertrophy is also prominent due to fatty infiltration of gastrocnemius muscles.
Neuromuscular Disorders - Junction & Journey Jitters
-
Myasthenia Gravis (MG): Autoimmune (postsynaptic AChR Ab). Fatigable weakness (ptosis, diplopia, dysphagia). Worsens with activity, improves with rest. Ice pack test positive. Rx: Pyridostigmine, immunosuppressants (steroids, azathioprine), thymectomy.
- Neonatal MG: Transient, due to maternal IgG transfer; resolves in weeks.
-
Lambert-Eaton Myasthenic Syndrome (LEMS): Autoimmune (presynaptic P/Q-type VGCC Ab). Proximal muscle weakness, autonomic dysfunction (dry mouth). Strength ↑ with brief exercise. Often paraneoplastic (Small Cell Lung Cancer).
-
Infant Botulism: Clostridium botulinum spores (e.g., honey). Toxin blocks presynaptic ACh release. Descending flaccid paralysis, constipation, poor suck, hypotonia ("floppy baby"). Rx: Human Botulism Immune Globulin (BIG-IV).
-
Guillain-Barré Syndrome (GBS): Acute inflammatory demyelinating polyradiculoneuropathy. Ascending symmetric paralysis, areflexia. Often post-infectious (e.g., Campylobacter jejuni).
⭐ CSF analysis in GBS typically shows albuminocytologic dissociation (↑ protein, normal WBC count) after 1-2 weeks.
-
Spinal Muscular Atrophy (SMA): Degeneration of anterior horn cells. Autosomal recessive (SMN1 gene mutation). Progressive muscle weakness, hypotonia. "Floppy infant" with intact sensation, normal intellect. 📌 "SMA-shes motor neurons"
High‑Yield Points - ⚡ Biggest Takeaways
- DMD: X-linked, absent dystrophin, Gower's sign, calf pseudohypertrophy, ↑CK.
- SMA Type 1: AR SMN1 mutation, severe infantile hypotonia, tongue fasciculations, "frog-leg" posture.
- Myasthenia Gravis: AChR antibodies, ptosis, fatigable weakness, improves with rest/AchE inhibitors.
- GBS: Acute ascending paralysis, post-infectious (e.g., Campylobacter), CSF albuminocytologic dissociation.
- BMD: Milder X-linked dystrophinopathy (abnormal dystrophin), later onset than DMD.
- CMT Disease: Hereditary motor-sensory neuropathy, pes cavus, foot drop, distal atrophy_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

