Allergic Rhinitis - Nose Knows No Peace
- IgE-mediated inflammation of nasal mucous membranes.
- Types: Seasonal (SAR), Perennial (PAR). Classified by ARIA guidelines: Intermittent (<4 days/wk or <4 consecutive wks) vs. Persistent (>4 days/wk & >4 consecutive wks).
- Symptoms: Paroxysmal sneezing, watery rhinorrhea, nasal itching, congestion.
- Signs: Allergic shiners, transverse nasal crease (allergic salute), Dennie-Morgan infraorbital folds.

- Common Indian Triggers: Pollens (e.g., Parthenium), house dust mites, molds, animal dander, cockroach allergens.
⭐ Allergic rhinitis often coexists with asthma and atopic dermatitis, forming the "atopic march" (sequential development of allergic diseases).
Allergic Rhinitis - The IgE Mayhem
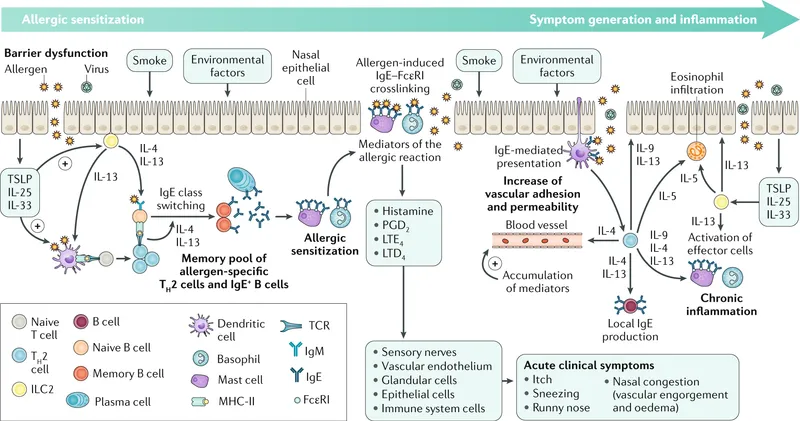
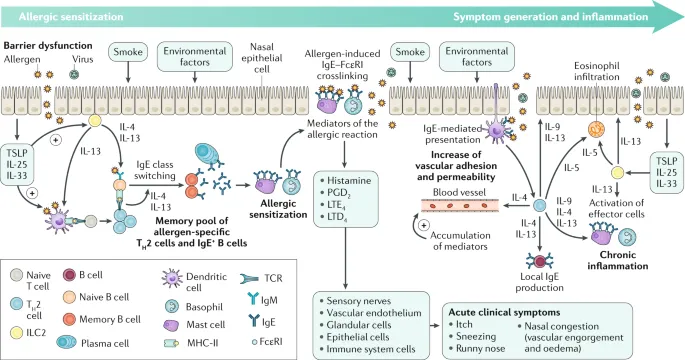
- Type I (IgE-mediated) hypersensitivity to aeroallergens (pollen, dust mites). Mast cells & basophils central.
- Pathogenesis:
- Sensitization: Allergen → Th2 cells → IL-4/IL-13 → B-cells produce IgE → IgE coats mast cells.
- Elicitation (Re-exposure): Allergen cross-links IgE → mast cell degranulation.
- Mediators & Phases:
- Early (minutes): Histamine, PGD2, Leukotrienes (LTC4/D4/E4) → acute symptoms.
- Late (4-8 hrs): Eosinophil influx (via IL-5), cytokines → sustained inflammation, hyperreactivity.
- Core Symptoms: Sneezing, watery rhinorrhea, nasal itching, congestion. Ocular symptoms common.
⭐ Part of the "Atopic March": often coexists/precedes asthma and atopic dermatitis. Risk for asthma development.
Allergic Rhinitis - Symptoms & Stages
- Core Symptoms:
- Paroxysmal sneezing
- Watery rhinorrhea (anterior/posterior)
- Nasal itching
- Nasal obstruction/congestion
- Associated Symptoms:
- Ocular: Itching, redness, tearing (allergic conjunctivitis)
- Palatal itching, cough, fatigue
- Signs:
- Allergic shiners (infraorbital edema & darkening)
- Dennie-Morgan lines (infraorbital folds)
- Nasal salute & transverse nasal crease
- Pale, boggy, bluish nasal turbinates

ARIA Classification:
- Duration:
- Intermittent: Symptoms < 4 days/week OR < 4 consecutive weeks
- Persistent: Symptoms > 4 days/week AND > 4 consecutive weeks
- Severity (QoL impact):
- Mild: Normal sleep & activities/work/school; no troublesome symptoms.
- Moderate-Severe: ≥1: Sleep disturbed; activities/work/school impaired; troublesome symptoms.
⭐ Eosinophils are the predominant inflammatory cells in nasal secretions in allergic rhinitis.
Allergic Rhinitis - Calming the Storm
IgE-mediated nasal mucosal inflammation by aeroallergens (pollens, dust mites, dander). Classified: Intermittent/Persistent; Mild/Moderate-Severe.
- Core Symptoms: Paroxysmal sneezing, watery anterior rhinorrhea, nasal pruritus, and nasal congestion.
- Associated signs: Allergic shiners, transverse nasal crease (allergic salute), Dennie-Morgan lines.
- Diagnosis:
- Primarily clinical, based on characteristic symptoms and allergen exposure history.
- Skin Prick Test (SPT): Preferred for identifying specific IgE sensitization. Rapid, sensitive.
- Serum specific IgE: Useful alternative if SPT is contraindicated (e.g., dermatographism).
- Management Approach:
- Key Pharmacotherapy:
- INCS (Intranasal Corticosteroids): Fluticasone, Mometasone. Most potent; reduce inflammation and all nasal symptoms.
- Antihistamines (Oral 2nd Gen): Cetirizine, Levocetirizine. Rapid relief of itching, sneezing, rhinorrhea. Less sedating.
- LTRAs (Leukotriene Receptor Antagonists): Montelukast. Beneficial for nasal congestion, especially with co-existing asthma.
- Allergen Immunotherapy (AIT): SCIT/SLIT. Disease-modifying; for selected patients with persistent mod-severe AR unresponsive to drugs, with confirmed sensitization.
⭐ Intranasal corticosteroids (INCS) are the cornerstone and most effective first-line treatment for persistent moderate-to-severe allergic rhinitis, improving all nasal symptoms.
High‑Yield Points - ⚡ Biggest Takeaways
- IgE-mediated Type I hypersensitivity reaction to common aeroallergens.
- Characterized by watery rhinorrhea, paroxysmal sneezing, nasal itching, and congestion.
- Look for allergic shiners, transverse nasal crease, and Dennie-Morgan lines.
- Key triggers include pollens, house dust mites, animal dander, and molds.
- Diagnosis: primarily clinical, supported by skin prick test or serum specific IgE.
- First-line: intranasal corticosteroids; antihistamines for symptomatic relief.
- Potential complications: ↑ risk of otitis media, sinusitis, and asthma exacerbation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

