Ca/P Homeostasis - Bone Builders' Blueprint
- PTH (Parathyroid Hormone): ↑ Serum $Ca^{2+}$, ↓ Serum $PO_4^{3-}$.
- Bone: ↑ Resorption (↑ $Ca^{2+}$, ↑ $PO_4^{3-}$ release).
- Kidney: ↑ $Ca^{2+}$ reabsorption, ↓ $PO_4^{3-}$ reabsorption, ↑ Vit D activation.
- Intestine (indirectly via Vit D): ↑ $Ca^{2+}$ & $PO_4^{3-}$ absorption.
- Vitamin D (Calcitriol): ↑ Serum $Ca^{2+}$, ↑ Serum $PO_4^{3-}$.
- Intestine: ↑ $Ca^{2+}$ & $PO_4^{3-}$ absorption.
- Bone: ↑ Mineralization (indirect), ↑ Resorption (high doses).
- Kidney: ↑ $Ca^{2+}$ & $PO_4^{3-}$ reabsorption.
- Calcitonin: ↓ Serum $Ca^{2+}$, ↓ Serum $PO_4^{3-}$. (Minor role in humans)
- Bone: ↓ Resorption.
- Kidney: ↑ $Ca^{2+}$ & $PO_4^{3-}$ excretion.
Normal Serum Levels:
- Total $Ca^{2+}$: 8.5‑10.5 mg/dL
- Ionized $Ca^{2+}$: 4.65‑5.25 mg/dL
- $PO_4^{3-}$: 2.5‑4.5 mg/dL
- ALP: 30‑120 U/L
- PTH: 10‑65 pg/mL
- 25(OH)Vit D: 30‑100 ng/mL

⭐ Ionized calcium ($Ca^{2+}$) is the physiologically active form and its level is affected by pH (acidosis ↑ $Ca^{2+}$, alkalosis ↓ $Ca^{2+}$).
Hypocalcemia - Calcium Crash Course
- Causes: Vitamin D deficiency, hypoparathyroidism (e.g., DiGeorge syndrome), pseudohypoparathyroidism, chronic renal failure, acute pancreatitis, massive blood transfusion (citrate toxicity).
- Clinical Features: 📌 CATS go numb:
- Convulsions
- Arrhythmias
- Tetany (Chvostek's sign, Trousseau's sign)
- Spasms, paresthesias (numbness, tingling)
- Symptomatic if Ionized Ca < 4.4 mg/dL or Total Ca < 7.5 mg/dL.
- ECG: Prolonged QT interval.
- Acute Management:
- Chronic Management: Oral Calcium supplements + Vitamin D.
⭐ DiGeorge syndrome (22q11.2 deletion) is a significant cause of neonatal hypocalcemia due to parathyroid hypoplasia.
Hypercalcemia - Calcium Overload Ops
- Causes: Hyperparathyroidism, Malignancy (rare peds), Vitamin D intoxication, Immobilization, Williams Syndrome, Granulomatous diseases (e.g., Sarcoidosis).
- Clinical Features: 📌 'Bones (pain), Stones (renal), Groans (abdominal pain), Psychiatric Overtones (confusion)'. Severe if Ca > 14 mg/dL.
- ECG: Short QT interval.

- Management:
- Hydration (IV Normal Saline), Furosemide (post-hydration).
- Bisphosphonates (e.g., Pamidronate), Calcitonin.
- Dialysis for severe/refractory cases.
⭐ Williams syndrome is associated with idiopathic infantile hypercalcemia.
Rickets & Osteomalacia - Bendy Bones Brigade
Defective bone mineralization: rickets (growing), osteomalacia (mature).
- Types:
- Nutritional: Vit D deficiency (commonest).
- Vit D Dependent: Type 1 ($1\alpha$-hydroxylase $\downarrow$), Type 2 (receptor defect).
- Hypophosphatemic: X-linked dominant.
- Renal osteodystrophy.
- CF: Delayed fontanelles, craniotabes, rachitic rosary, Harrison's sulcus, wide wrists/ankles, bowing.
- X-ray: Metaphyseal cupping, fraying, splaying. Widened physis.
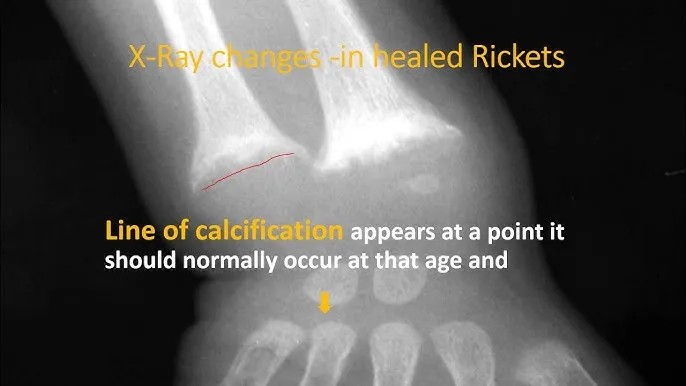
- Labs: $\downarrow$Ca, $\downarrow$P (not hypophosphatemic), $\uparrow$ALP, $\uparrow$PTH. 25(OH)D$\downarrow$ (nutritional), 1,25(OH)2D varies.
- Rx: Vit D (Stoss: 300,000-600,000 IU), Ca, P as needed.
⭐ Serum ALP is often elevated before X-ray changes in rickets.
Phosphate Imbalances - Phosphorus Patrol
- Hypophosphatemia (↓$PO_4^{3-}$):
- Causes: ↓Intake/absorption (malnutrition, antacids), ↑renal excretion (Fanconi syndrome), intracellular shift (refeeding syndrome, DKA).
- Features: Muscle weakness, rhabdomyolysis, respiratory failure, altered mental status. Severe < 1 mg/dL.
- Mgmt: Oral/IV phosphate replacement; treat underlying cause.
- Hyperphosphatemia (↑$PO_4^{3-}$):
- Causes: CKD (most common), hypoparathyroidism, tumor lysis syndrome, Vit D intoxication, ↑phosphate intake.
- Features: Often asymptomatic; symptoms of hypocalcemia (tetany), soft tissue/vascular calcification.
- Mgmt: Dietary phosphate restriction, phosphate binders, dialysis if severe.
⭐ Refeeding syndrome is a potentially fatal condition characterized by severe hypophosphatemia following re-introduction of nutrition in malnourished individuals, leading to cardiac, pulmonary, and neurological complications.
High‑Yield Points - ⚡ Biggest Takeaways
- Rickets: Vitamin D deficiency causes ↓Ca, ↓PO4, ↑ALP, ↑PTH; features craniotabes, rachitic rosary.
- Hypoparathyroidism: Presents with ↓Ca, ↑PO4, ↓PTH; Chvostek's/Trousseau's signs, DiGeorge association.
- Pseudohypoparathyroidism: PTH resistance leads to ↓Ca, ↑PO4, ↑PTH; Albright's osteodystrophy.
- Hypercalcemia causes: Consider immobilization, malignancy, hyperparathyroidism (MEN syndromes), or FHH (CaSR mutation, low urine Ca).
- VDDR: Type 1 (1α-hydroxylase defect), Type 2 (Vitamin D receptor defect).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

