Psychosomatic Intro - Mind-Body Tango
- Psychosomatic disorders: Physical symptoms originating from or worsened by mental/emotional factors.
- Represents a true mind-body interaction; not feigning illness (malingering) or intentionally producing symptoms (factitious disorder).
- Stress, anxiety, or depression can manifest as real physical complaints.
- Common pediatric presentations: recurrent abdominal pain, headaches, fatigue, non-epileptic seizures.
- Diagnosis involves excluding organic causes and identifying psychosocial stressors.
⭐ Conversion disorder, a type of psychosomatic illness, is more common in females and often presents with neurological symptoms like pseudoseizures or paralysis after a stressor.
Common Syndromes - Physical Echoes
| Syndrome | Symptoms | Differentiators / Pointers |
|---|---|---|
| Recurrent Abdominal Pain (RAP) | Periumbilical pain, often stress-related; nausea | Normal growth & physical exam; Rome IV criteria; no alarm signs (fever, weight loss) |
| Psychogenic Headaches | Tension-type (band-like) or migraine-like; stress link | Normal neurological exam; no red flags; may disrupt school attendance |
| Conversion Disorder | Sudden motor/sensory loss (e.g., paralysis, blindness, aphonia) | Inconsistent findings (e.g., Hoover's sign); identifiable stressor; "la belle indifférence" (sometimes) |
| Psychogenic Non-Epileptic Seizures (PNES) | Seizure-like events; closed eyes; pelvic thrusting; asynchronous movements | Preserved awareness (often); normal ictal/interictal EEG; suggestibility; no true postictal state |
Etiological Web - Stress & Strain
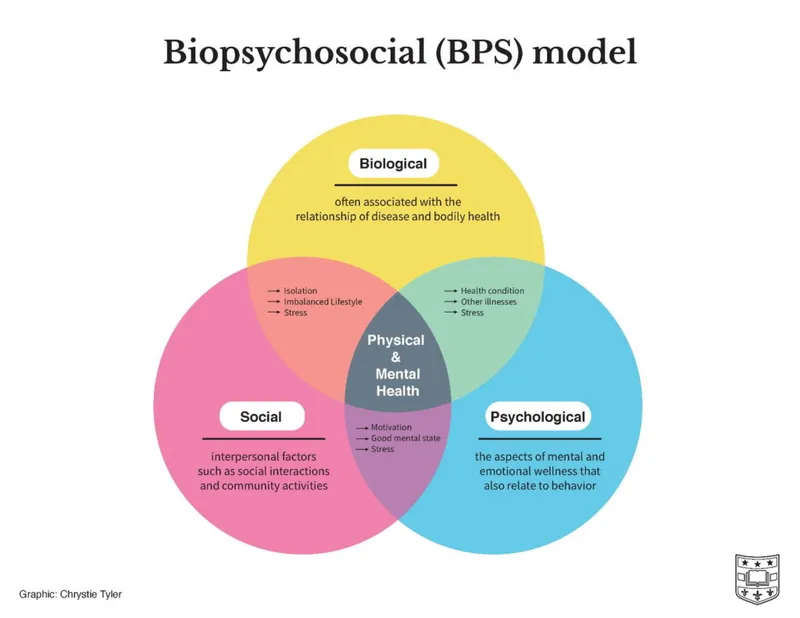
- Biopsychosocial Model: Interplay of factors.
- Biological: Genetic predisposition, HPA axis dysregulation, neurotransmitter imbalances.
- Psychological: Personality (alexithymia, anxiety), poor coping skills, trauma history, internal conflicts.
- Social: Family dysfunction (conflict, enmeshment, parental stress), academic/school pressures, peer issues, cultural factors.
- Stressors: Acute (e.g., exams, loss) or chronic (e.g., bullying, ongoing family discord).
- Strain: Individual's psychophysiological response to stressors, manifesting as physical symptoms.
⭐ Recurrent Abdominal Pain (RAP) is a common psychosomatic presentation; thorough medical workup is crucial before psychological attribution.
Diagnostic Approach - Unmasking Illusions
Systematic evaluation is crucial. Focus on excluding organic pathology first.
⭐ Key: Symptoms are real to the patient, not intentionally feigned (distinguishes from malingering/factitious disorder).
Therapeutic Toolkit - Restoring Balance
- Multimodal Approach: Cornerstone of care.
- Psychoeducation: Child & family; explain mind-body link, validate feelings.
- Psychotherapy:
- Cognitive Behavioral Therapy (CBT): Core.
- Family Therapy: Address dynamics.
- Relaxation techniques, Biofeedback.
- Pharmacotherapy (Judicious):
- Symptomatic relief (e.g., analgesics).
- SSRIs/Anxiolytics for comorbidities.
- Rehabilitation: Gradual return to school/activities; physiotherapy if indicated.
- Team Care: Pediatrician, mental health professionals, school.
⭐ CBT is the most evidence-based psychotherapy for pediatric psychosomatic disorders.
High‑Yield Points - ⚡ Biggest Takeaways
- Psychosomatic disorders: Real physical symptoms (e.g., pain, fatigue) from psychological distress, not feigned.
- Common: Recurrent abdominal pain (RAP), chronic headaches, non-epileptic seizures, conversion symptoms.
- Diagnosis: Exclude organic causes; identify psychosocial stressors (school, family).
- Conversion disorder: Neurological symptoms (e.g., paralysis, pseudo-seizures) without a neurological basis, often stress-linked.
- Management: Reassurance, CBT, family therapy; address underlying emotional issues.
- Crucial: Avoid excessive investigations once organic disease is ruled out_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

