Inflicted Burns - Scalding Suspicion
- Pattern: Sharp demarcation lines ("tide mark"), uniform depth. Absence of splash marks.
- Distribution:
- Symmetrical burns on buttocks, perineum, or extremities.
- "Glove" or "stocking" distribution on hands/feet.
- "Donut" pattern on buttocks (spared area where skin touches cooler tub bottom).
- Forced immersion: Flexion sparing in popliteal, antecubital fossae, groin.
- Depth: Often full-thickness, uniform depth due to prolonged contact.
- History: Inconsistent or changing history, delay in seeking care.
⭐ Forced immersion scalds often show a clear upper level of the burn (water line) and sparing of skin creases that are flexed and pressed together, preventing water contact.
- Differential: Accidental scalds (irregular margins, splash marks, variable depth, history consistent with injury).
Skeletal Trauma - Bones Don't Lie
- High Specificity Fractures (NAI indicators):
- Metaphyseal Corner Fractures (MCF) / Bucket Handle Fractures (Classical Metaphyseal Lesions - CML).
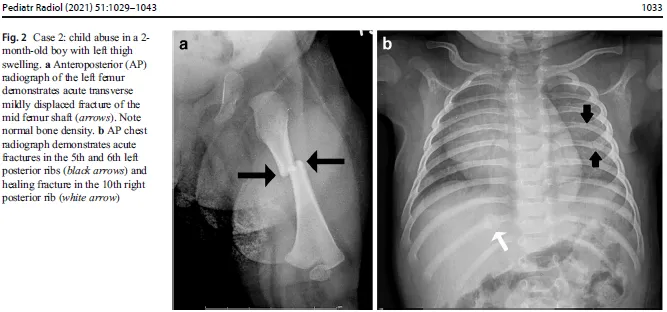
- Posterior Rib Fractures (due to squeezing/shaking).
- Scapular, Sternal, Spinous Process Fractures (high force).
- Other Red Flags:
- Multiple fractures in various stages of healing.
- Any fracture in a non-ambulatory infant (e.g., femur, humerus <1 year old).
- Complex skull fractures (e.g., depressed, diastatic, occipital, growing).
- Investigation:
- Skeletal survey for all suspected NAI < 2 years.
- Repeat survey in 2 weeks (detects occult/healing fractures).
- Differential Diagnosis: Osteogenesis Imperfecta (OI), Rickets. History often inconsistent with injury in NAI.
⭐ Metaphyseal corner fractures (CML) are virtually pathognomonic of non-accidental injury (NAI).
Head & Abdominal Trauma - Hidden Dangers
- Abusive Head Trauma (AHT) / Shaken Baby Syndrome:
- Violent shaking +/- impact.
- Triad: Subdural hematoma, retinal hemorrhages, encephalopathy.
- Also: Posterior rib, metaphyseal fractures.
- Signs: Irritability, lethargy, seizures, apnea.
- ⚠️ History-injury mismatch is key.
- Skull Fractures (Suspicious):
- Multiple, complex, bilateral, depressed, or crossing suture lines.
- Abdominal Trauma (Often occult):
- 2nd leading cause of death in abuse.
- Blunt force (punch, kick).
- Injuries: Liver laceration (most common), pancreas, duodenal hematoma, bowel perforation.
- Signs: Vomiting (bilious), pain, distension, shock.
⭐ Duodenal hematoma: specific inflicted injury; bilious vomiting, "double bubble" on X-ray.
 oka
oka
Evaluation & Reporting - Spotting & Acting
- Initial Approach: Maintain high index of suspicion. Prioritize child's immediate safety.
- History Taking:
- Inconsistent, vague, or changing explanations.
- Delay in seeking medical care.
- Mechanism of injury incompatible with developmental age.
- Physical Examination:
- Complete head-to-toe exam (child undressed).
- Note patterned injuries (e.g., belt marks, cigarette burns).
- Multiple injuries in different stages of healing.
- 📌 TEN-4 FACES-P bruising rule for concern:
- Torso, Ears, Neck in children < 4 years.
- Any bruise in an infant < 4 months old.
- Frenulum, Angle of jaw, Cheek, Eyelids, Sclera; Patterned bruises.
- Key Investigations:
- Skeletal survey: Mandatory for all suspected abuse cases < 2 years; repeat in 2 weeks.
- CT/MRI head: If suspected head trauma, seizures, or altered sensorium.
- Ophthalmology consultation: For retinal hemorrhages.
- Coagulation profile: To rule out bleeding disorders.
⭐ Retinal hemorrhages, especially bilateral and extensive, are highly suggestive of Abusive Head Trauma (AHT) or Shaken Baby Syndrome.
- Medico-legal Responsibilities & Reporting:
- Mandatory reporting to Child Welfare Committee (CWC) and local police (under JJ Act & POCSO Act).
- Detailed, objective documentation. Register as a Medico-Legal Case (MLC).
- Involve a multidisciplinary team (pediatrician, social worker, law enforcement).
High‑Yield Points - ⚡ Biggest Takeaways
- Patterned burns (cigarette, iron) and immersion scalds (glove/stocking, doughnut) strongly suggest inflicted trauma.
- Scalds with sharp demarcation, uniform depth, and flexural sparing are highly suspicious for abuse.
- Multiple fractures in varied healing stages are classic for Non-Accidental Injury (NAI).
- Metaphyseal corner fractures and posterior rib fractures are highly specific for child abuse.
- Abusive Head Trauma (Shaken Baby): subdural hematoma, extensive retinal hemorrhages, and encephalopathy.
- Inconsistent history, delayed presentation, or bruises in atypical sites/non-mobile infants are major red flags_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

