Pediatric ECG & Arrhythmia Basics - Tiny Tickers Tune-Up
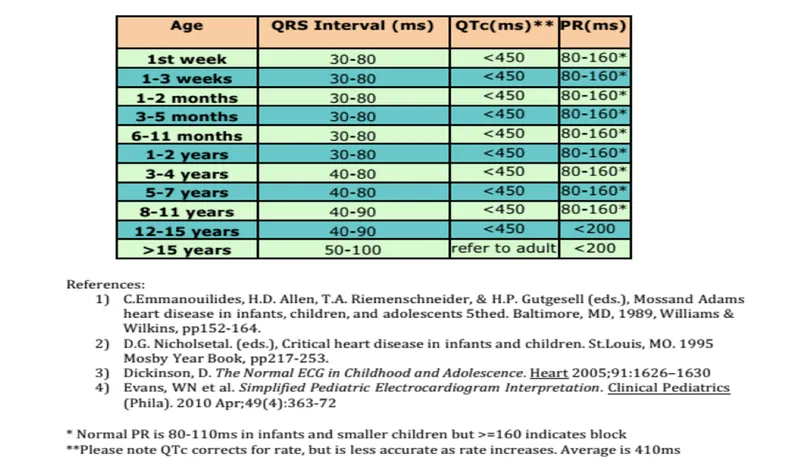
- Normal ECG (Age-Dependent):
- HR: Neonate 100-180 bpm, ↓ with age.
- PR: 0.08-0.18s; QRS: <0.09s (both ↑ with age).
- Axis: Neonatal RV dominance (right axis +30° to +180°), shifts left.
- Arrhythmia Classification:
- By Rate: Tachyarrhythmias vs. Bradyarrhythmias.
- By QRS: Narrow (supraventricular) vs. Wide (ventricular/SVT with aberrancy).
⭐ Sinus arrhythmia is a common, benign finding in children, varying with respiration.
Supraventricular Tachycardias (SVT) - Speedy Heartbeats Sleuth
- Most common pediatric tachyarrhythmia; narrow QRS (<0.09s).
- Types:
- AV Re-entrant Tachycardia (AVRT): e.g., WPW syndrome. Most common.
- AV Nodal Re-entrant Tachycardia (AVNRT).
- Atrial Flutter: "Sawtooth" waves.
- Atrial Fibrillation: Irregularly irregular.
- Ectopic Atrial Tachycardia (EAT).
- ECG: Rate often >220/min (infants), >180/min (children). P-waves often absent/retrograde.
⭐ Most SVT in neonates and infants is AVRT due to an accessory pathway.
- Acute Management:
- Stable:
- Vagal maneuvers (ice to face <6mo, Valsalva).
- Adenosine: 0.1 mg/kg (max 6mg), then 0.2 mg/kg (max 12mg). 📌 A-den-O-sine: AV N Ode slowdown!
- Unstable: Synchronized cardioversion (0.5-1 J/kg, then 2 J/kg).
- Stable:
- Long-term: β-blockers, digoxin (avoid in WPW if AF/flutter), ablation.

Ventricular Arrhythmias - Ventricle Voltage Vibes
- Ventricular Tachycardia (VT)
- ECG: Wide QRS (>0.09s child), AV dissociation.
- Causes: Structural heart disease, channelopathies.
- Rx (Stable): Amiodarone.
- Premature Ventricular Complexes (PVCs)
- ECG: Wide, bizarre QRS. Often benign.
- Worry: Frequent, multiform, R-on-T.
- Torsades de Pointes (TdP)
- ECG: Polymorphic VT, QT prolongation.
- Causes: $↓K⁺$, $↓Mg²⁺$, drugs. Rx: IV $MgSO_4$.

⭐ For TdP in children, IV Magnesium Sulfate is crucial; avoid drugs prolonging QT interval.
Bradycardias & Conduction Blocks - Slow-Mo Heart Signals
- Sinus Bradycardia: HR < age normal (Neonate <100, Infant <90, Child 1-6y <80, >6y <60 bpm).
- AV Blocks:
- 1st Degree: Prolonged PR interval.
- 2nd Degree Mobitz I (Wenckebach): Progressive PR↑ → dropped QRS.
- 2nd Degree Mobitz II: Intermittent non-conducted P waves, fixed PR.
- 3rd Degree (Complete Heart Block/CHB): Complete AV dissociation.
- Causes: Hypoxia, acidosis, drugs (β-blockers, digoxin), ↑ICP, hypothyroidism, post-op cardiac surgery.
- Pacing Indications: Symptomatic bradycardia, CHB, Mobitz II.

⭐ Maternal SLE (anti-Ro/SSA antibodies) is a key cause of congenital complete heart block (CHB).
Channelopathies & Syndromic Arrhythmias - Faulty Wiring Woes
- Long QT Syndrome (LQTS): Genetic ion channel defect. QTc >460ms prolonged. Risk of Torsades de Pointes (TdP). Rx: β-blockers, ICD.
- 📌 Jervell and Lange-Nielsen: LQTS + sensorineural deafness. (AR inheritance).
- Brugada Syndrome: SCN5A mutation. ECG: Coved ST ↑ V1-V3 (Type 1). Risk of VT/VF, SCD. Rx: ICD.
- CPVT (Catecholaminergic Polymorphic VT): RYR2/CASQ2 mutations. Exercise-induced bidirectional/polymorphic VT. Rx: β-blockers, ICD.
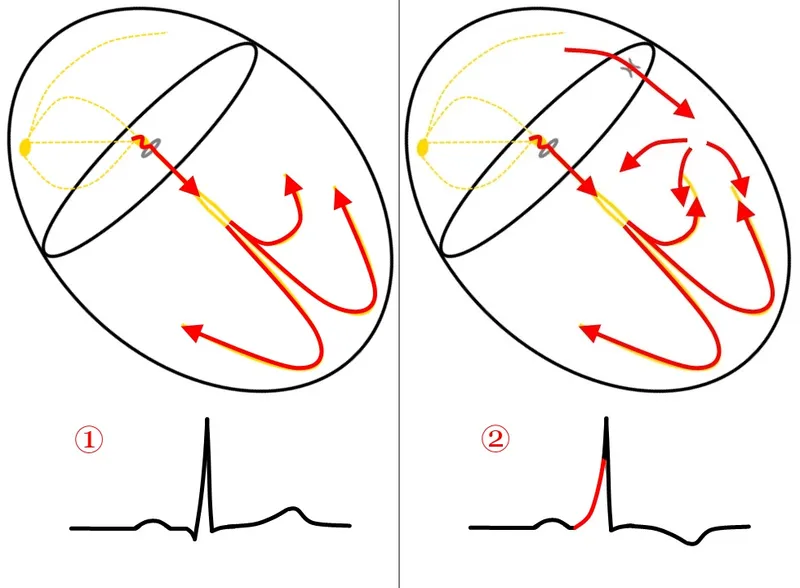
- WPW (Wolff-Parkinson-White): Accessory pathway (Bundle of Kent). ECG: Short PR, Delta wave. Risk of SVT. Rx: Ablation.
⭐ WPW + AF can lead to VF if AV nodal blockers (e.g., digoxin, verapamil) are used.
High‑Yield Points - ⚡ Biggest Takeaways
- Supraventricular Tachycardia (SVT) is the most common symptomatic tachyarrhythmia in children; initial treatment includes vagal maneuvers, then adenosine.
- Wolff-Parkinson-White (WPW) syndrome ECG shows a delta wave, short PR interval, and wide QRS; predisposes to SVT.
- Long QT Syndrome (LQTS) can present with syncope, seizures, or sudden cardiac death; beta-blockers are first-line therapy.
- Congenital Complete Heart Block (CHB) in neonates is strongly associated with maternal SLE (anti-Ro/SSA antibodies).
- Sinus arrhythmia is a normal physiological variant in children, characterized by heart rate changes with respiration.
- Atrial arrhythmias are frequent long-term sequelae in patients with uncorrected Atrial Septal Defects (ASD).
- Ventricular tachycardia (VT) is rare but life-threatening; consider myocarditis, cardiomyopathy, or channelopathies as causes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

