Wilson's Disease - Copper Chaos Conundrum
- Etiology: Autosomal recessive; ATP7B gene mutation → impaired copper excretion.
- Pathophysiology: Copper accumulates: liver, brain, cornea, kidneys.
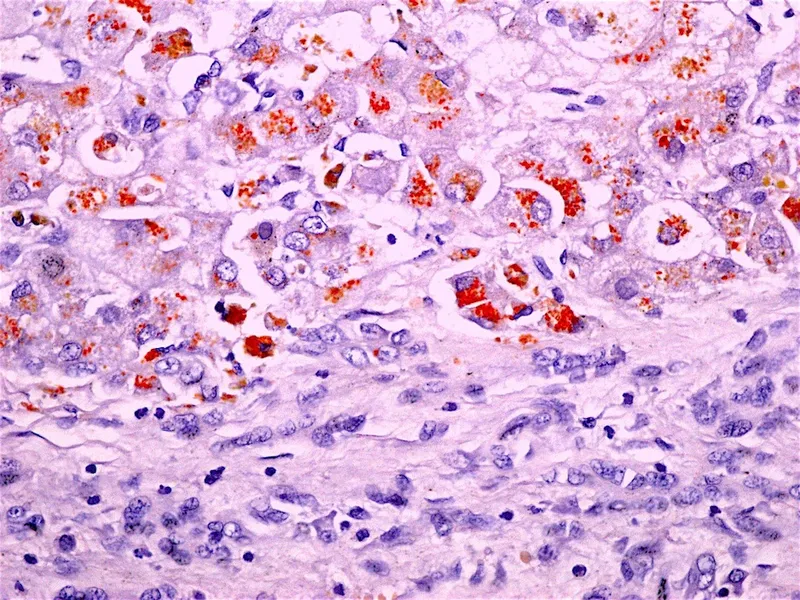
- Clinical Features:
- Liver: Hepatitis, cirrhosis, acute liver failure.
- Neuropsychiatric: Parkinsonism, dysarthria, psychiatric changes.
- Ocular: Kayser-Fleischer rings, sunflower cataracts.
- Other: Fanconi syndrome, hemolytic anemia.
- Diagnosis:
- ↓ Serum ceruloplasmin (< 20 mg/dL).
- ↑ Urinary copper (> 100 µg/24h).
- ↑ Hepatic copper (> 250 µg/g dry weight) - Gold standard.
- Treatment: Chelators (Penicillamine, Trientine), Zinc, Liver transplant.
⭐ Low serum ceruloplasmin is a key diagnostic marker, but it can be normal or even elevated in acute liver failure due to Wilson's disease or during an acute phase response.
Hereditary Hemochromatosis - Iron Overload Ordeal
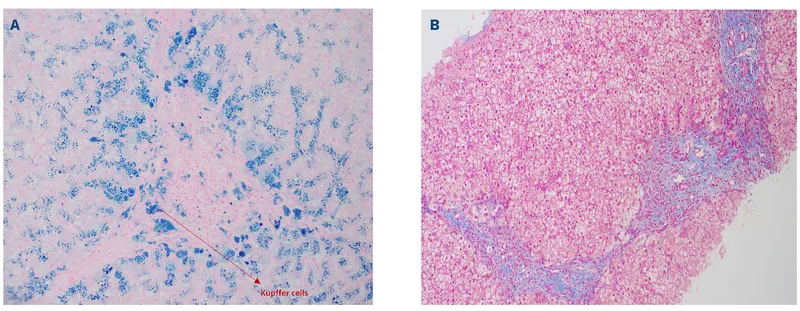
- Autosomal recessive disorder; ↑ intestinal iron absorption & deposition.
- Pathogenesis: Primarily HFE gene mutations (C282Y, H63D) → ↓ hepcidin synthesis → unregulated iron entry into plasma.
- Clinical Triad (Classic): Cirrhosis, diabetes mellitus, skin pigmentation ("Bronze Diabetes").
- Other organs: Heart (cardiomyopathy), joints (arthropathy, esp. 2nd/3rd MCPs), pancreas, gonads (hypogonadism).
- Diagnosis:
- ↑ Serum ferritin (>1000 ng/mL highly suggestive).
- ↑ Transferrin saturation (>45-50%).
- Genetic testing for HFE mutations.
- Liver biopsy: ↑ Iron (Perls' Prussian blue stain); quantification of hepatic iron concentration.
- Complications: Hepatocellular carcinoma (HCC), heart failure.
- Treatment: Therapeutic phlebotomy (mainstay); iron chelators (deferoxamine, deferasirox).
⭐ The most common mutation in Hereditary Hemochromatosis is C282Y in the HFE gene; homozygosity for C282Y is found in the majority of clinically affected individuals of Northern European descent.
📌 Mnemonic: "Heavy Fe Element" for HFE gene.
Alpha‑1 Antitrypsin Deficiency - Protein Misfold Peril
- Genetic Basis: Autosomal codominant, SERPINA1 gene mutation (PiZZ most severe).
- Pathophysiology: Misfolded A1AT protein (Z allele) polymerizes, accumulates in hepatocyte endoplasmic reticulum. Results in ↓ A1AT secretion, leading to ↓ lung protection (emphysema) and liver damage.
- Clinical (Liver): Neonatal hepatitis, cholestasis, jaundice. Later: chronic hepatitis, cirrhosis, ↑ hepatocellular carcinoma (HCC) risk.
- Diagnosis: ↓ Serum A1AT levels, phenotype testing (Pi typing), genotype testing.
⭐ Liver biopsy in Alpha-1 Antitrypsin Deficiency characteristically shows PAS-positive, diastase-resistant globules within hepatocytes, representing accumulated A1AT protein.
- Management: Supportive care. Liver transplant for end-stage liver disease. Avoid smoking.
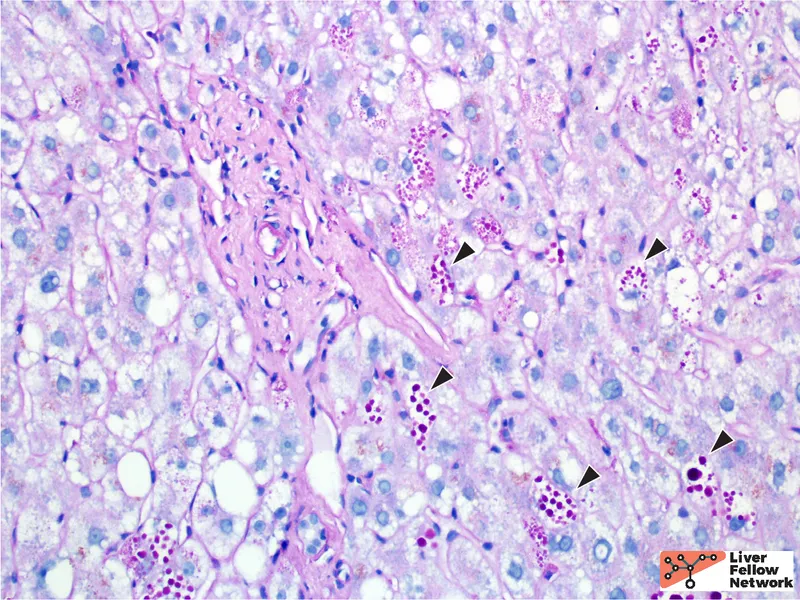
NAFLD/NASH - Fatty Liver Fallout
⭐ NAFLD is the hepatic manifestation of metabolic syndrome and is the most common cause of chronic liver disease in Western countries; insulin resistance is a key pathogenic factor.
- NAFLD: Hepatic steatosis; no significant alcohol.
- NASH: Steatosis + inflammation + hepatocyte injury (ballooning).
- Risk factors: Obesity, T2DM, dyslipidemia, metabolic syndrome.
- Pathogenesis: Insulin resistance key. "Multiple parallel hits" model.
- Dx: Imaging, LFTs (ALT > AST). Biopsy for NASH confirmation.
- Rx: Lifestyle (weight loss 7-10%), manage comorbidities.
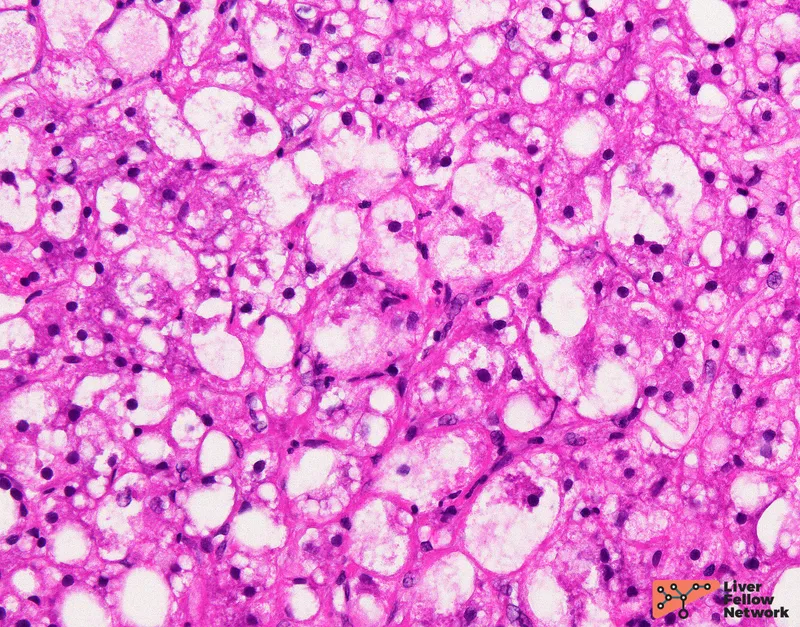
High‑Yield Points - ⚡ Biggest Takeaways
- Wilson's Disease: ATP7B defect, copper accumulation, Kayser-Fleischer rings, ↓ ceruloplasmin, ↑ urinary copper.
- Hereditary Hemochromatosis: HFE gene (C282Y), iron overload, ↑ ferritin, ↑ transferrin saturation, Prussian blue.
- Alpha-1 Antitrypsin Deficiency: SERPINA1 (PiZZ), PAS-D positive globules in periportal hepatocytes, cirrhosis & emphysema risk.
- NAFLD/NASH: Linked to insulin resistance & metabolic syndrome; spectrum from steatosis to cirrhosis.
- Galactosemia: GALT deficiency; galactose-1-phosphate accumulation causes liver damage, cataracts, E. coli sepsis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

