Basics of Transplantation - Mismatch Mayhem
- Graft Types:
- Autograft: Self tissue (e.g., skin).
- Isograft (Syngeneic): Identical twin.
- Allograft: Same species, genetically different.
- Xenograft: Different species (e.g., pig valve).
- Major Histocompatibility Complex (MHC) / HLA System:
- Genes on Chromosome 6p. Highly polymorphic.
- Class I (HLA-A, B, C): On all nucleated cells. Present to CD8+ T cells.
- Class II (HLA-DP, DQ, DR): On Antigen Presenting Cells (APCs). Present to CD4+ T cells.
⭐ HLA matching is most critical for kidney & bone marrow transplants; HLA-DR is key.
- Minor Histocompatibility Antigens: Non-MHC proteins; can cause slower rejection despite HLA match.
- Allorecognition Pathways:
- Direct: Recipient T-cells recognize intact donor MHC on donor APCs.
- Indirect: Recipient APCs process donor MHC, present peptides to recipient T-cells.
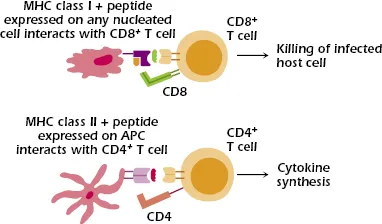
Graft Rejection - Immune System Strikes
Host immune response to foreign donor tissue (allograft), mainly via mismatched Major Histocompatibility Complex (MHC) antigens (HLAs in humans).
-
Pathways:
- Cell-mediated: Primarily CD8+ CTLs (direct cytotoxicity); CD4+ Th1 cells (cytokine release, e.g., IFN-γ, activating macrophages).
- Humoral: Donor-Specific Antibodies (DSA) activate complement cascade & Antibody-Dependent Cell-mediated Cytotoxicity (ADCC).
-
Types & Timeline:
- Hyperacute: Mins-hrs. Pre-formed antibodies (e.g., ABO, HLA). Type II Hypersensitivity Reaction (HSR). Results in thrombosis, ischemia.
- Acute: Days-weeks (can extend to months). Primarily T-cell driven (cellular rejection); humoral mechanisms (antibody-mediated rejection) can also occur.
⭐ Acute cellular rejection (T-cell mediated) is the most common form of graft rejection, typically occurring within the first 6 months post-transplant.
- Chronic: Months-years. Slow, progressive graft damage leading to fibrosis and vascular abnormalities (e.g., graft arteriosclerosis). Involves mixed T-cell/antibody roles, and non-immune factors. Type III & IV HSR elements.

📌 Mnemonic: "Hot ACid Chills" for rejection types: Hyperacute, Acute, Chronic.
Graft vs Host Disease - When Grafts Attack
- Immune attack by donor T-lymphocytes (graft) against recipient tissues (host).
- Common complication of allogeneic Hematopoietic Stem Cell Transplantation (HSCT).
- Prerequisites (Billingham's Postulates):
- Graft contains immunocompetent T cells.
- Host possesses antigens foreign to donor T cells.
- Host is immunoincompetent, unable to reject graft cells.
- Types:
- Acute GvHD: Occurs < 100 days post-transplant.
- Targets: Skin (maculopapular rash), Liver (jaundice, ↑LFTs), GIT (diarrhea, abdominal pain).
- Chronic GvHD: Occurs > 100 days post-transplant.
- Features resemble autoimmune disorders: Skin (sclerosis, lichenoid changes), eyes/mouth (sicca syndrome), lungs (bronchiolitis obliterans).
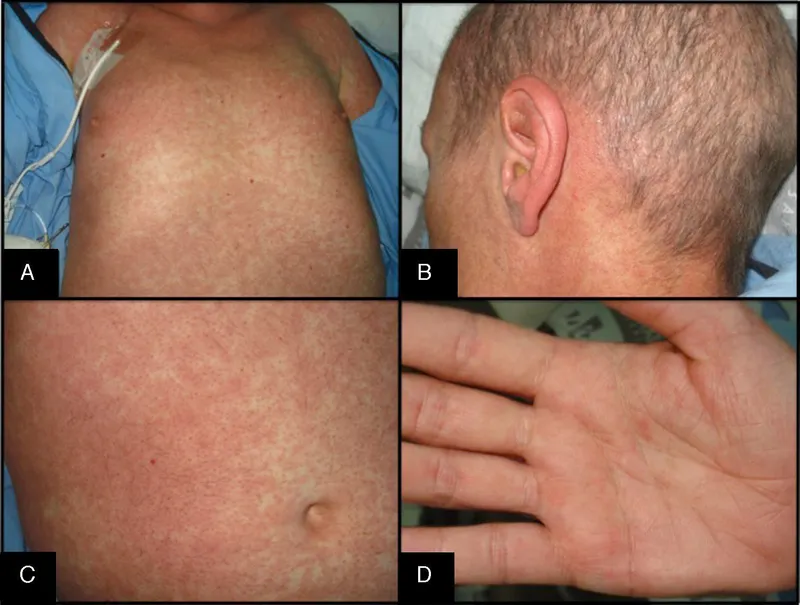
- Features resemble autoimmune disorders: Skin (sclerosis, lichenoid changes), eyes/mouth (sicca syndrome), lungs (bronchiolitis obliterans).
- Acute GvHD: Occurs < 100 days post-transplant.
⭐ The triad of dermatitis, hepatitis, and enteritis is characteristic of acute GvHD.
Immunosuppressive Therapy - Taming the Beast
- Goal: Prevent rejection/GVHD; minimize drug toxicity (infection, malignancy).
- Strategy: Combination therapy, lower individual drug doses.
- Phases:
- Induction: Intense, peri-transplant (Basiliximab, ATG).
- Maintenance: Long-term (CNI + Antimetabolite ± Steroids).
- Anti-rejection: Acute episodes (Pulse steroids, ATG).
- Key Drugs/Classes:
- Calcineurin Inhibitors (CNIs): Tacrolimus, Cyclosporine.
- ↓ IL-2 production.
- Nephrotoxic, Neurotoxic, HTN, Diabetes.
- Antiproliferatives: Mycophenolate Mofetil (MMF), Azathioprine.
- MMF: Inhibits IMPDH (lymphocyte purine synthesis).
- GI (MMF), myelosuppression.
- mTOR Inhibitors: Sirolimus, Everolimus.
- Block IL-2 signaling.
- Hyperlipidemia, myelosuppression, poor wound healing.
- Corticosteroids: Prednisone.
- Broad anti-inflammatory, ↓ cytokines.
- Cushingoid, osteoporosis, hyperglycemia.
- Antibodies: Basiliximab (Anti-CD25), ATG (T-cell depleting).
- Calcineurin Inhibitors (CNIs): Tacrolimus, Cyclosporine.
⭐ Calcineurin inhibitors (Tacrolimus, Cyclosporine) are notorious for causing nephrotoxicity, a major dose-limiting side effect.
High‑Yield Points - ⚡ Biggest Takeaways
- Hyperacute rejection is immediate, mediated by pre-formed anti-donor antibodies (ABO/HLA).
- Acute cellular rejection (days-weeks) is T-cell driven (Type IV HSR), often reversible with immunosuppression.
- Acute humoral rejection involves donor-specific antibodies and C4d deposition in vessels.
- Chronic rejection (months-years) features graft arteriosclerosis and interstitial fibrosis, poorly responsive.
- Graft-versus-Host Disease (GVHD) occurs when donor T-cells attack recipient tissues, especially in BMT.
- Mainstay immunosuppressants include calcineurin inhibitors, antimetabolites, and steroids.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

