Immune Response to Infections - Gatekeepers & Guards
- Innate Immunity (First Line): Rapid, non-specific.
- Barriers: Physical (skin, mucosa), chemical (lysozyme, pH), biological (flora).
- Key Cells:
- Phagocytes: Neutrophils (early), Macrophages (APC, late).
- NK Cells: Cytotoxic; target viral/tumor cells (no prior sensitization).
- Recognition & Signaling:
- PRRs (e.g., TLRs, NLRs): Detect PAMPs (Pathogen-Associated) & DAMPs (Damage-Associated).
- Complement System: Proteins activated via Classical, Alternative, Lectin pathways.
- Functions: Opsonization (C3b), Lysis (MAC: C5b-C9), Inflammation (C3a, C5a). 📌 CALM.
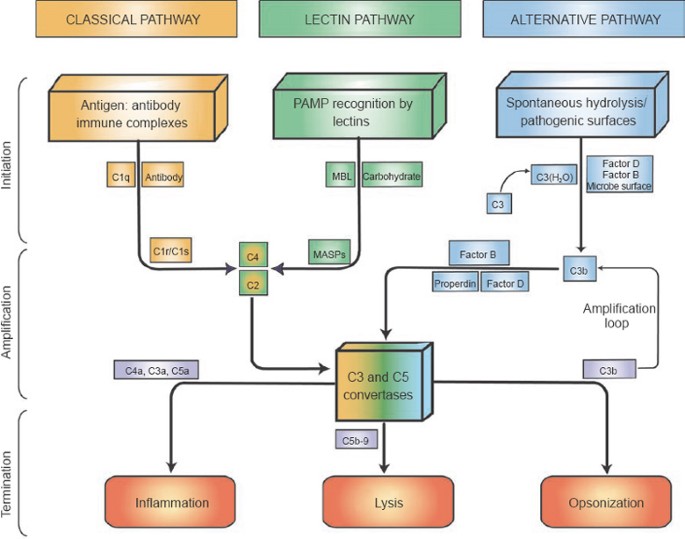
> ⭐ **TLR4** recognizes Lipopolysaccharide (LPS) on Gram-negative bacteria, a key PAMP.
Immune Response to Infections - Special Forces Strike
Adaptive immunity: "Special Forces" (T & B lymphocytes) for targeted elimination & memory. APCs present antigens via MHC for activation.
-
Cell-Mediated Immunity (CMI): T-cell driven; combats intracellular pathogens (viruses, Mycobacteria) & tumor cells.
- CD4+ T Helper (Th) Cells: Orchestrate.
- Th1: IFN-γ → Potent macrophage activation (vs. intracellular microbes); granuloma formation.
- Th2: IL-4, IL-5, IL-13 → B-cell switching to IgE, eosinophil activation (helminths, allergy).
- CD8+ Cytotoxic T Lymphocytes (CTLs): Directly kill virus-infected/tumor cells (perforins/granzymes); MHC-I restricted.
- CD4+ T Helper (Th) Cells: Orchestrate.
-
Humoral Immunity: B-cell driven; antibodies neutralize/eliminate extracellular microbes & toxins.
- B-cells → Plasma cells → Antibodies (IgM, IgG, IgA, IgE).
- Key Antibody Actions: Neutralization, opsonization (enhances phagocytosis), complement activation.
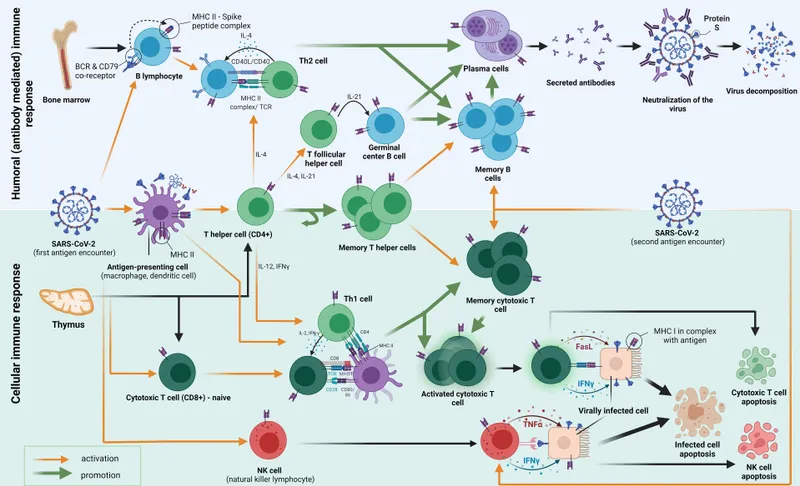
⭐ IFN-γ, secreted by Th1 cells and NK cells, is pivotal for macrophage activation and effective clearance of intracellular pathogens like Mycobacterium tuberculosis.
Immune Response to Infections - Know Your Enemy
Host defense mechanisms are tailored to specific pathogen classes.
- Innate Immunity: Rapid, non-specific first line.
- Cells: Phagocytes (Neutrophils, Macrophages), NK cells.
- Soluble: Complement, Interferons (IFNs), Cytokines.
- Adaptive Immunity: Specific, develops memory.
- Humoral (B-cells): Antibodies → Extracellular pathogens.
- Cell-Mediated (T-cells): CTLs (cytotoxic T lymphocytes), Th1 (intracellular pathogens), Th17 (fungi, extracellular bacteria), Th2 (helminths).
| Pathogen | Key Innate Response | Key Adaptive Response |
|---|---|---|
| Extracellular Bacteria | Phagocytosis, Complement | Antibodies (IgM, IgG), Th17 cells |
| Intracellular Bacteria | Macrophages, NK cells | Th1 cells (IFN-γ), CTLs |
| Viruses | IFN-α/β, NK cells | Neutralizing Antibodies, CTLs |
| Fungi | Neutrophils, Macrophages | Th1 cells, Th17 cells |
| Parasites (Helminths) | Eosinophils, Mast cells | IgE, Th2 cells (IL-4, IL-5, IL-13) |
Immune Response to Infections - Masters of Disguise
- Microbial Evasion Strategies:
- Antigenic variation: Altering surface antigens (e.g., Influenza, HIV, Neisseria).
- Complement inhibition: Preventing opsonization/lysis.
- Resistance to phagocytosis: Capsules (e.g., S. pneumoniae), toxins.
- Blocking IFN pathways: Dampening antiviral responses.
- Establishing latency: Persisting silently (e.g., Herpesviruses, HIV).
- Immunopathology (Damage by Immune Response):
- Cytokine storm: Excessive inflammation (e.g., Sepsis, ARDS).
- Immune complex deposition: Glomerulonephritis, vasculitis.
- Molecular mimicry: Cross-reactive antibodies triggering autoimmunity (e.g., Rheumatic fever).
- Granuloma formation: Walling off pathogens, but causing fibrosis (e.g., TB).
⭐ Antigenic variation in Trypanosoma brucei involves sequential expression of variant surface glycoproteins (VSGs), enabling chronic infection by evading host antibodies.
High‑Yield Points - ⚡ Biggest Takeaways
- Innate immunity: first defense via phagocytes (neutrophils, macrophages), NK cells.
- Adaptive immunity (T/B cells): specific, long-lasting protection, immunological memory.
- T-helper (CD4+) cells: orchestrate responses, activate B cells & cytotoxic T cells.
- Cytotoxic T (CD8+) cells: kill virus-infected and tumor cells.
- Antibodies: neutralize toxins, opsonize pathogens, activate complement.
- Granulomatous inflammation: characteristic of intracellular pathogens (e.g., TB).
- Microbes use immune evasion (antigenic variation, latency) to persist.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

