Effusion Basics - Fluid Foundations
- Effusion: Abnormal fluid accumulation in body cavities (pleural, peritoneal, pericardial).
- Types:
- Transudate: Systemic factors (↑ hydrostatic pressure e.g., CHF; ↓ oncotic pressure e.g., cirrhosis). Clear, low protein/LDH.
- Exudate: Local factors (inflammation, infection, malignancy). Cloudy, high protein/LDH.
- Light's Criteria (Exudate if ≥1):
- $ \frac{\text{Pleural Fluid Protein}}{\text{Serum Protein}} > \mathbf{0.5} $
- $ \frac{\text{Pleural Fluid LDH}}{\text{Serum LDH}} > \mathbf{0.6} $
- Pleural Fluid LDH > $ \mathbf{\frac{2}{3}} $ of the upper limit of normal (ULN) for serum LDH.
- Collection: EDTA (cells), plain (biochem), sterile (micro). Process fresh.
- Processing: Smears (Pap, MGG), cell block (histology, IHC).

⭐ In India, tuberculosis is a very common cause of exudative pleural effusions, often lymphocyte-predominant.
Benign Findings - Innocent Inhabitants
- Mesothelial Cells:
- Arrangement: Single, flat sheets, loose clusters, papillae.
- Nuclei: Round/oval, central, smooth contour; nucleoli can be prominent.
- Cytoplasm: Abundant, dense; may show blebs, vacuoles.
- Hallmarks: "Windows" (intercellular gaps), scalloped "community" borders.
- Reactive atypia: ↑Nuclei/nucleoli, multinucleation; benign architecture.
- Inflammatory Cells:
- Neutrophils: Acute inflammation (e.g., empyema).
- Lymphocytes: Chronic (TB, viral), autoimmune.
- Eosinophils (>10%): Allergic, parasitic, Hodgkin's, pneumothorax.
- Macrophages: Foamy, phagocytic.
- Plasma cells: Chronic inflammation.
- Other Benign Elements:
- RBCs: Trauma, contamination.
- LE cells: Specific for SLE.
- DCTs (Detached Ciliary Tufts): Benign; respiratory/fallopian origin.
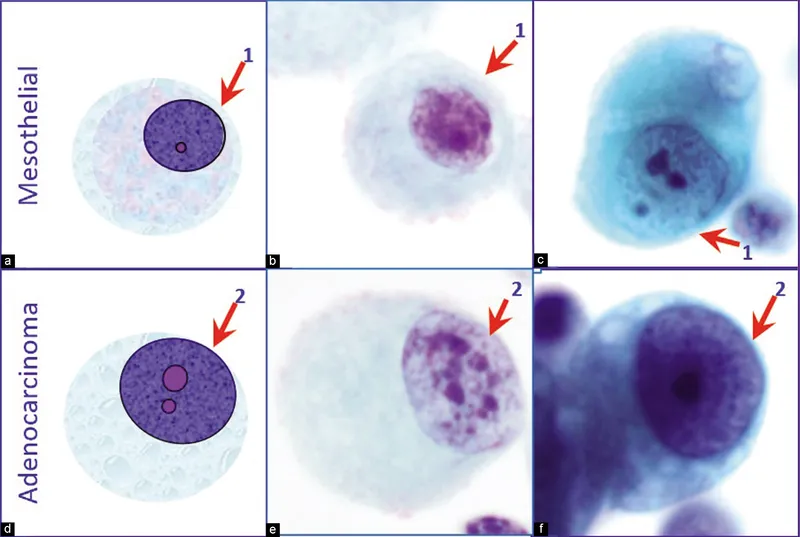
⭐ "Windows" (intercellular spaces) in mesothelial cell groups are a key benign sign, contrasting with adenocarcinoma's tight, 3D clusters without such gaps.
Malignant Cells - Cancerous Clues
- General Malignant Criteria:
- ↑ N:C ratio, nuclear pleomorphism, hyperchromasia.
- Irregular nuclear membrane, coarse chromatin, prominent/multiple/irregular nucleoli.
- Atypical mitoses.
- Cellular crowding: 3D clusters (morulae, papillae, acini), cell balls.
- Single malignant cells with overt features of malignancy.
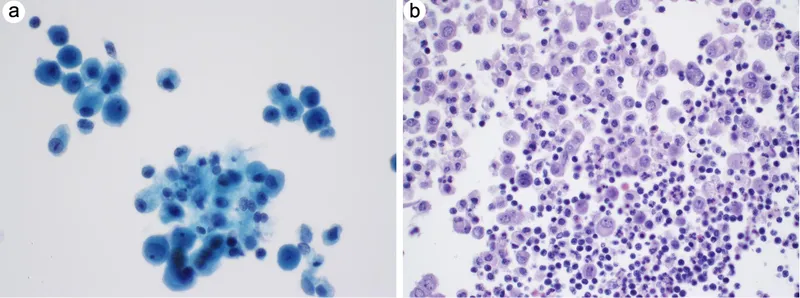
- Key Tumor Types:
- Adenocarcinoma: Most common. Glandular clusters, acini, papillae; signet-ring cells (GIT, breast). Cytoplasmic mucin vacuoles (PAS-D+). Psammoma bodies (ovary, lung).
- Squamous Cell Carcinoma (SCC): Keratinized cells (dense, orangeophilic/eosinophilic cytoplasm), bizarre shapes (e.g., tadpole, spindle), sharp cell borders.
- Lymphoma/Leukemia: Monotonous population of dispersed atypical lymphoid/leukemic cells, high N:C ratio, scant cytoplasm. Lymphoglandular bodies (background).
- Melanoma: Single cells or loose clusters. Melanin pigment (variable, fine brown granules). Prominent eosinophilic nucleoli. Intranuclear cytoplasmic pseudoinclusions.
⭐ Signet ring cells in an effusion strongly suggest metastatic adenocarcinoma, commonly from the gastrointestinal tract or breast, and carry a poor prognosis.
Special Cases & Stains - Meso & Markers
- Malignant Mesothelioma:
- Cytology: Large cells, prominent nucleoli, dense cytoplasm; clusters, morules ("mulberry"), "windows" (cell separation), cell-in-cell.
- Fluid: Often viscous (↑ hyaluronic acid).
- Special Stains: Alcian blue +ve (digests with hyaluronidase), PAS-D -ve.
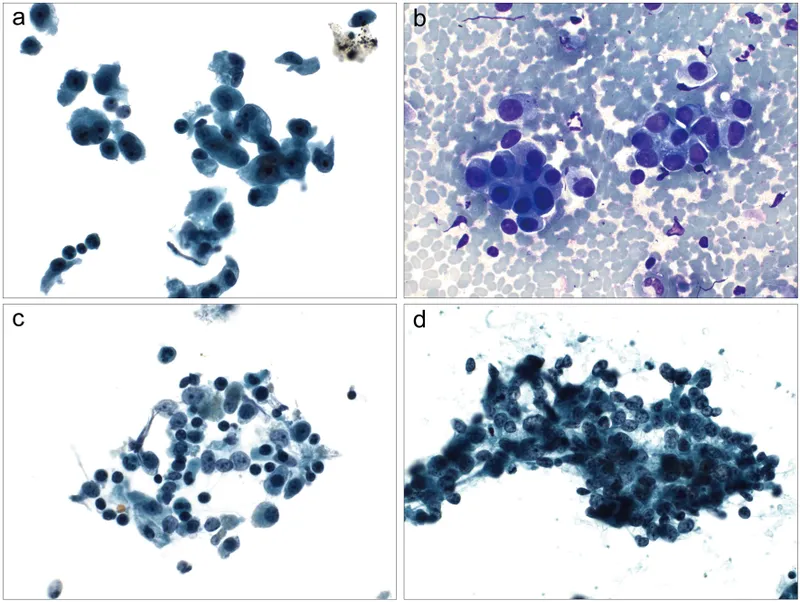
- IHC for Mesothelioma vs. Adenocarcinoma:
- Meso Positive Panel: Calretinin (nuclear & cytoplasmic), WT-1 (nuclear), CK5/6, D2-40 (podoplanin). (📌 Mnemonic: "Call WiTh 5 or 6 Doctors")
- Adeno Positive Panel (Meso Negative): CEA, Ber-EP4, MOC-31, TTF-1 (Lung), Napsin A (Lung).
⭐ EMA typically shows a thick, "garland-like" peripheral membranous staining in mesothelioma, contrasting with the apical/luminal staining in adenocarcinoma.
High‑Yield Points - ⚡ Biggest Takeaways
- Transudates: paucicellular (mesothelial cells); Exudates: ↑cellularity (inflammatory/malignant cells).
- Reactive mesothelial cells (windows, scalloped borders) vs. malignant mesothelioma (large clusters, psammoma bodies).
- Adenocarcinoma: commonest metastasis; look for signet ring cells, glandular clusters.
- Lymphocyte-predominant effusions: suspect tuberculosis or lymphoma.
- LE cells are pathognomonic for SLE. Cell blocks are vital for IHC.
- Psammoma bodies: seen in serous ovarian Ca, mesothelioma, papillary thyroid Ca.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

