SCI Basics & Anatomy - Cord Under Siege
- Etiology:
- Trauma (common): RTA, falls, violence.
- Non-traumatic: Vascular, tumors, infections, degenerative.
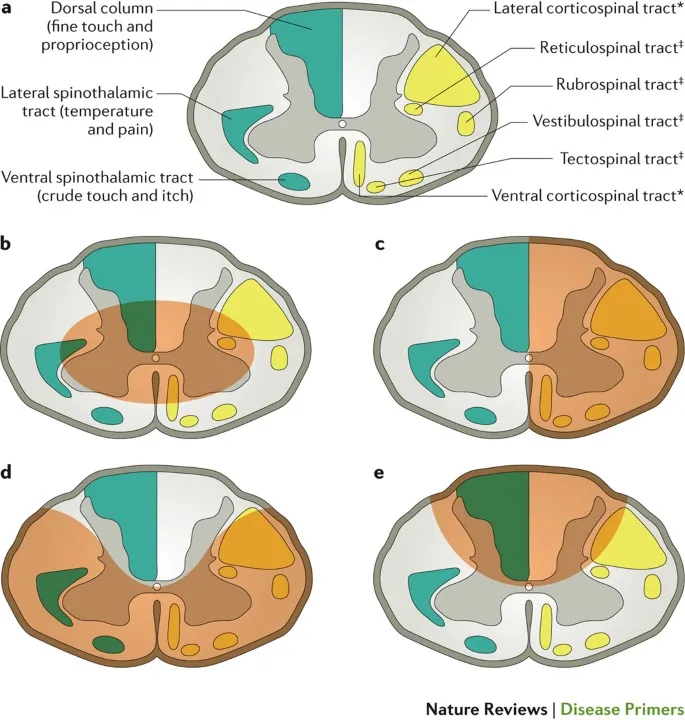
- Cord Structure:
- Meninges: Dura, Arachnoid, Pia.
- Grey matter (central H-shape): Neuronal bodies.
- White matter (peripheral): Tracts.
- Ascending: Dorsal columns (proprioception, vibration, fine touch), Spinothalamic (pain, temp).
- Descending: Corticospinal (motor).
- Vascular Supply:
- Anterior Spinal Artery (ASA): Anterior 2/3.
- Posterior Spinal Arteries (PSAs): Posterior 1/3.
- Key Concepts:
- Spinal Shock: Transient reflex loss below injury.
- Neurogenic Shock: Hypotension, bradycardia (injury ≥T6).
⭐ Vertebral level often doesn't correspond to spinal cord segment level, especially in lower spine (e.g., L1 vertebra injury can affect S1-S5 cord segments).
SCI Classification & Syndromes - Code Red Cord
-
ASIA Impairment Scale (AIS):
- A: Complete. No S4-S5 motor/sensory.
- B: Sensory Incomplete. Sensory preserved below neurological level (NL) & S4-S5; no motor.
- C: Motor Incomplete. Motor preserved below NL; >half key muscles <3.
- D: Motor Incomplete. Motor preserved below NL; ≥half key muscles ≥3.
- E: Normal.
-
Key SCI Syndromes:
| Syndrome | Motor Deficit | Sensory Deficit | 📌 Key / Prognosis |
|---|---|---|---|
| Brown-Séquard | Ipsilateral UMN, proprioception, vibration | Contralateral pain/temp | Hemi-section. Good. 📌 "One Sided Story" |
| Central Cord | UE > LE weakness | "Cape-like" pain/temp loss | Hyperextension. Fair.  |
| Anterior Cord | Complete motor paralysis | Pain/temp loss; proprioception intact | Flexion; ASA occlusion. Poor. |
| Posterior Cord | Minimal weakness | Proprioception/vibration loss | Rare; PSA occlusion. Good. |
| Conus Medullaris | Symmetric LMN LE; Early bowel/bladder | Saddle anesthesia | L1-L2; UMN+LMN. Variable. |
| Cauda Equina | Asymmetric LMN LE; Late bowel/bladder | Saddle anesthesia; radicular pain | Below L2; LMN. Variable. |
Clinical Picture & Diagnosis - Spotting the Damage
- Initial: ABCDEs. Neuro exam (motor, sensory, reflexes). ASIA Scale.
- Spinal Shock: Temp. reflex/sensorimotor loss below injury. Flaccid paralysis, areflexia, absent BCR. BCR return ends shock.
- Neurogenic Shock (SCI ≥T6): Sympathetic loss → vagal. Hypotension (SBP <90 mmHg), bradycardia, poikilothermia. ⚠️ Vs. hypovolemic.
- Table: Shock Types
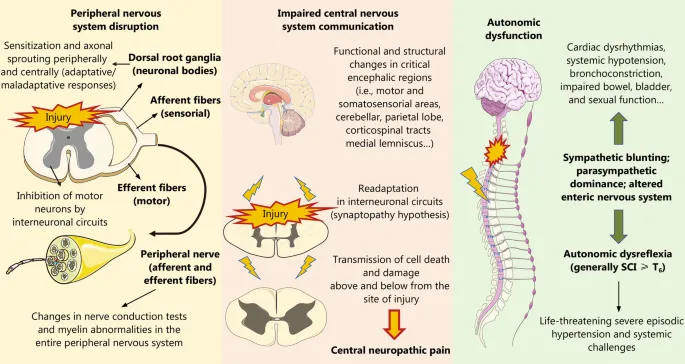
Feature Spinal Neurogenic (≥T6) Cause Reflex loss Sympathetic loss BP Norm/Var ↓ Hypotension HR Norm/Var ↓ Bradycardia Reflexes Absent Unaffected - Autonomic Dysreflexia (SCI ≥T6, post-shock): Trigger: noxious stimuli (full bladder). Sudden HTN (↑SBP 20-40 mmHg), headache, bradycardia, sweating above.
- ⭐ > Autonomic dysreflexia is a medical emergency in patients with SCI at or above T6, characterized by paroxysmal hypertension, bradycardia, and headache, often triggered by bladder or bowel distension.
- Diagnosis: Clinical (ASIA). Imaging: X-ray, CT; MRI (cord std).
SCI Management & Complications - Road to Recovery
Acute Management:
- Medical:
⭐ While controversial and not universally recommended, the NASCIS II protocol for methylprednisolone (bolus 30 mg/kg IV over 15 min, then 5.4 mg/kg/hr for 23 hrs if started within 3-8 hrs of injury) is a frequently tested topic.
- Hemodynamic support (MAP >85-90 mmHg).
- DVT/Stress ulcer prophylaxis.
- Surgical: Decompression, stabilization if indicated.
- Complications:
- Neurogenic Shock (↓BP, ↓HR).
- Spinal Shock (transient flaccid paralysis).
- Autonomic Dysreflexia (≥T6): noxious stimuli → HTN, headache. Rx: sit up, remove trigger.
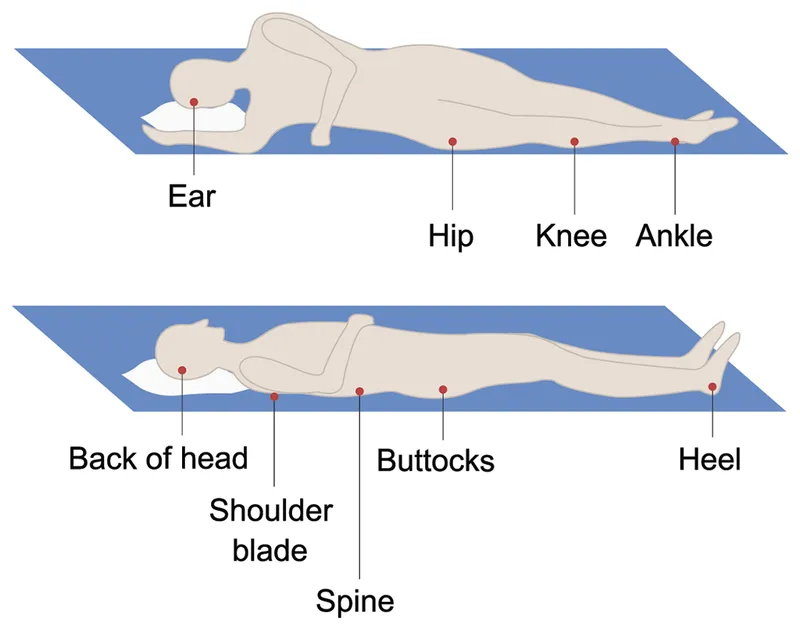
- Pressure Sores.
- Respiratory, DVT/PE.
- Rehab: Multidisciplinary team approach for functional recovery and quality of life improvement.
High‑Yield Points - ⚡ Biggest Takeaways
- ASIA Scale is vital for SCI classification and predicting prognosis.
- Distinguish spinal shock (transient areflexia) from neurogenic shock (hypotension, bradycardia).
- Central cord syndrome: Most common incomplete SCI; upper limbs affected more than lower.
- Anterior cord syndrome: Worst prognosis; motor, pain, temperature loss below lesion.
- Brown-Séquard syndrome: Ipsilateral motor/proprioception loss, contralateral pain/temperature loss.
- Autonomic dysreflexia (lesions above T6): Medical emergency; triggered by noxious stimuli below injury.
- Sacral sparing indicates an incomplete lesion and a better chance of recovery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

