Pediatric Bone: Unique Features - Not Just Little Adults
- Thicker Periosteum: Highly osteogenic; promotes rapid healing, increased callus formation, and fracture stability.
- Physis (Growth Plate): Weakest structural component; common site for Salter-Harris fractures. Ligaments are generally stronger than the physis.
- Bone Properties: More porous, less dense, and more elastic than adult bone. Allows for greater plastic deformation before fracturing.
- Unique Fracture Patterns:
- Greenstick: Incomplete fracture; one side of cortex broken, other side bent.
- Torus (Buckle): Impaction fracture causing a bulge or buckle in the cortex.
- Plastic Bowing: Bone bends without a visible cortical disruption.
- Healing & Remodeling Potential:
- Rapid healing; non-union is rare.
- Significant remodeling capacity, especially for angular deformities in the plane of joint motion and in younger children.
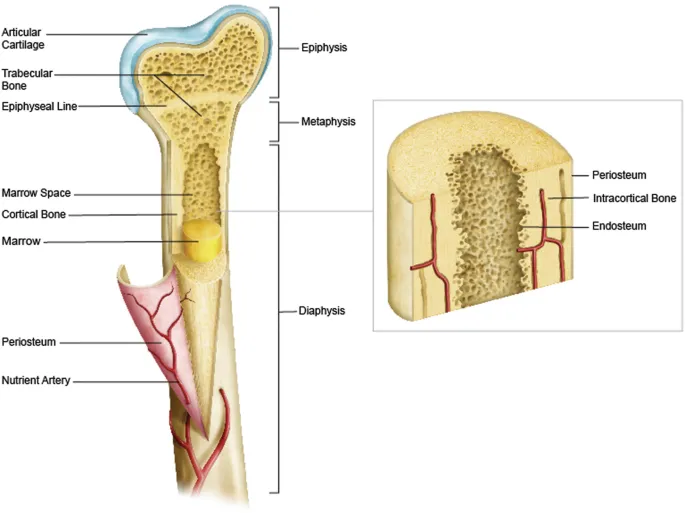
⭐ The thick, metabolically active periosteum in children is a key factor for faster fracture healing, robust callus formation, and its ability to act as a hinge during fracture reduction, often remaining intact on the concave side of angulated fractures.
Fracture Classification: Physeal & Patterns - Growth Plate Perils
- Physeal (Growth Plate) Injuries: Classified by Salter-Harris (SH). Physis = weakest zone.
- 📌 Mnemonic: SALTER
- S (Type I - Slipped): Through physis. Good prognosis.
- A (Type II - Above): Physis & Metaphysis. Most common. Good prognosis.
- L (Type III - Lower): Physis & Epiphysis. Intra-articular. Poorer prognosis.
- T (Type IV - Through/Transverse): Metaphysis, Physis & Epiphysis. Intra-articular. High risk of complications.
- ER (Type V - Erasure/Rammed): Crush of physis. Worst prognosis; growth arrest common.
- Risk of growth disturbance: V > IV > III > II > I.
- 📌 Mnemonic: SALTER
⭐ Salter-Harris Type II is the most common physeal fracture, typically involving the distal radius.
- Common Pediatric Fracture Patterns:
- Greenstick Fx: Incomplete; one cortex fractured, other bent. Like breaking a young branch.
- Torus (Buckle) Fx: Compression failure; bulging cortex. Stable.
- Plastic Bowing Deformity: Bone bends, no visible fracture line. Common in ulna/fibula.
- Complete Fx: Both cortices broken.
Common Pediatric Fractures: Regional Review - Hotspots & How-Tos
- Clavicle: Most common pediatric fracture. Typically mid-third. Often a birth injury (shoulder dystocia). Tx: Sling or Figure-of-eight bandage for 3-4 weeks.
- Supracondylar Humerus: Most common elbow fracture (~60%). FOOSH mechanism. Gartland classification.
- Complications: Volkmann's ischemic contracture (brachial artery), nerve injury (Median > Radial > Ulnar). Anterior humeral line, Baumann's angle assessment.
- Tx: Type I: Cast (~3 wks); Type II/III: Closed reduction & percutaneous pinning (CRPP).
- Lateral Condyle Humerus: Intra-articular (Salter-Harris Type IV). Risk: non-union, malunion (cubitus valgus), AVN. Tx: CRPP or ORIF if displaced >2mm.
- Forearm (Radius/Ulna): Distal radius most common. Greenstick & Torus (buckle) fractures frequent.
- Remodeling potential: <10 yrs: up to 20-30° angulation acceptable; >10 yrs: <10-15°.
- 📌 GRIMUS: Galeazzi - Radius fx, Inferior (Distal) radioulnar joint (DRUJ) injury; Monteggia - Ulna fx, Superior (Proximal) radioulnar joint / Radial head dislocation.
- Femur Shaft:
- <6 months: Pavlik harness.
- 6 months - 5 years: Hip spica cast.
- 6-12 years: Flexible intramedullary nails (TENS) or spica.
-
12 years: Rigid IM nail or plate.
- Tibia: Toddler's fracture (spiral fracture of tibia, typically undisplaced, in children 9 months - 3 years).
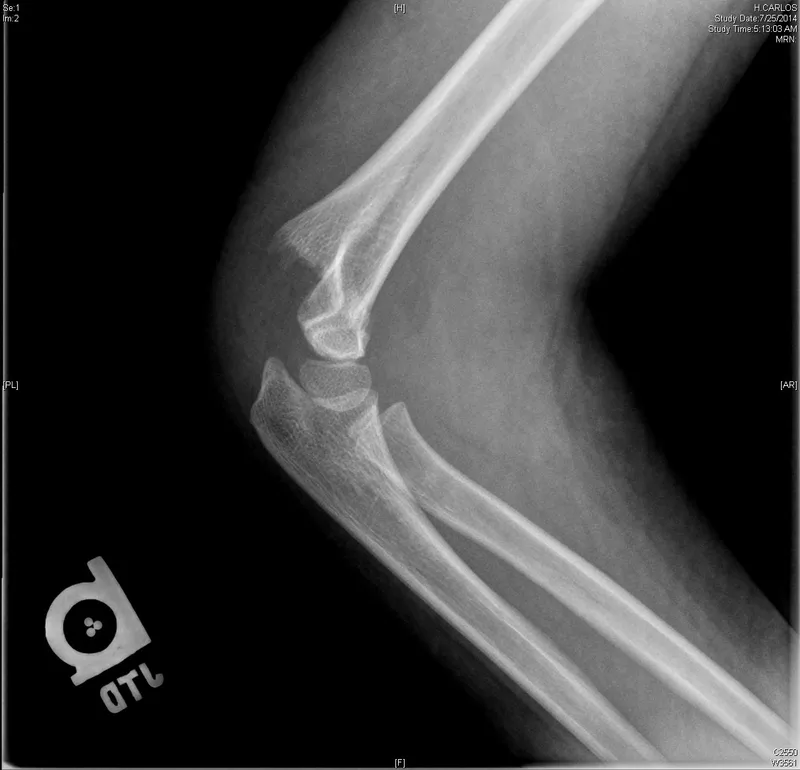
⭐ In supracondylar humerus fractures, posteromedial displacement is commonly associated with radial nerve injury, whereas posterolateral displacement often compromises the median nerve and brachial artery.
Fracture Complications & NAI - Red Flags & Responsibilities
- Complications:
- Early: Compartment syndrome (⚠️ urgent fasciotomy), neurovascular compromise, infection.
- Late: Malunion, nonunion, physeal arrest (growth issues), Avascular Necrosis (AVN).
- Non-Accidental Injury (NAI):
- Red Flags: Story-injury mismatch, multiple fractures (varied healing), bruises in pre-ambulatory infants.
- Highly specific: Metaphyseal corner fx, posterior ribs, sternal fx.
- Action: High suspicion, document meticulously, report (CWC/POCSO Act), ensure child safety.
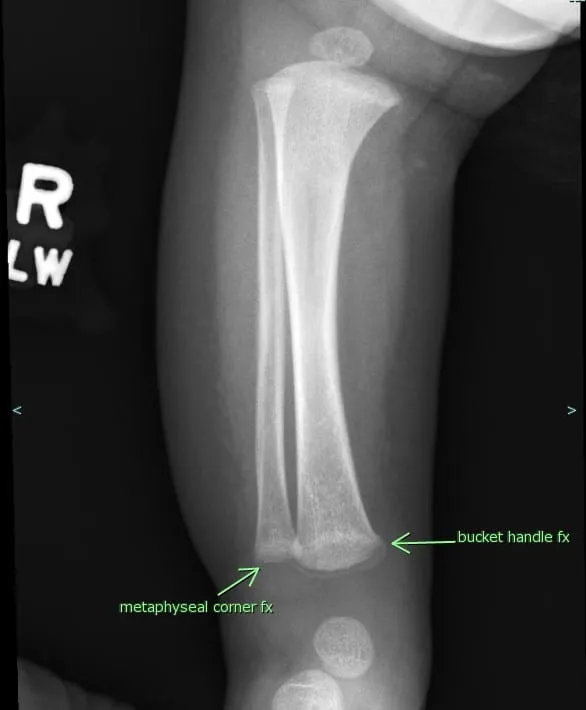
⭐ Metaphyseal "corner" or "bucket-handle" fractures are virtually pathognomonic for NAI.
 oka
oka
- Red Flags: Story-injury mismatch, multiple fractures (varied healing), bruises in pre-ambulatory infants.
High‑Yield Points - ⚡ Biggest Takeaways
- Salter-Harris Type II is the most common physeal injury.
- Greenstick and torus (buckle) fractures are unique to pediatric bones.
- Supracondylar humerus fractures: high risk of neurovascular injury and Volkmann's contracture.
- Clavicle fractures are very common, often treated non-operatively with a figure-of-eight bandage.
- Children possess excellent remodeling potential, especially for fractures near growth plates and in the plane of joint motion.
- Suspect non-accidental injury (NAI) with metaphyseal corner fractures, posterior rib fractures, or multiple fractures in varied healing stages.
- Toddler's fracture is typically an undisplaced spiral tibial fracture in young, ambulatory children (9 months to 3 years).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

