Benign Bone Tumors: Intro & Classification - Gentle Giants
- Definition: Non-cancerous, localized bone growths; generally not life-threatening, rarely metastasize.
- Key Features (Radiographic & Clinical):
- Well-defined, sharp "geographic" borders (Enneking Stage 1: Latent, Stage 2: Active)
- Sclerotic reactive rim often present
- No aggressive cortical destruction or extensive periosteal reaction
- Slow growth; often asymptomatic, may cause pain, swelling, or pathological fracture.
- Classification (by predominant cell type/tissue of origin):
- Cartilage-forming: Osteochondroma, Enchondroma, Chondroblastoma
- Bone-forming: Osteoid Osteoma, Osteoblastoma
- Fibrous: Non-ossifying fibroma (NOF), Fibrous Dysplasia
- Others: Giant Cell Tumor (GCT), Aneurysmal Bone Cyst (ABC), Hemangioma
⭐ Osteochondroma is the most common benign bone tumor.
Key Osteogenic & Chondrogenic Tumors - Bone Builders & Cartilage Crafters
- Osteogenic (Bone-Forming):
- Osteoid Osteoma:
- Age: < 30 yrs. Long bones (femur, tibia), spine.
- Pain: Nocturnal, severe, localized.
⭐ Osteoid osteoma pain is classically relieved by NSAIDs due to prostaglandin E2 production by the nidus.
- X-ray: Radiolucent nidus (< 1.5-2 cm) with surrounding reactive sclerosis.
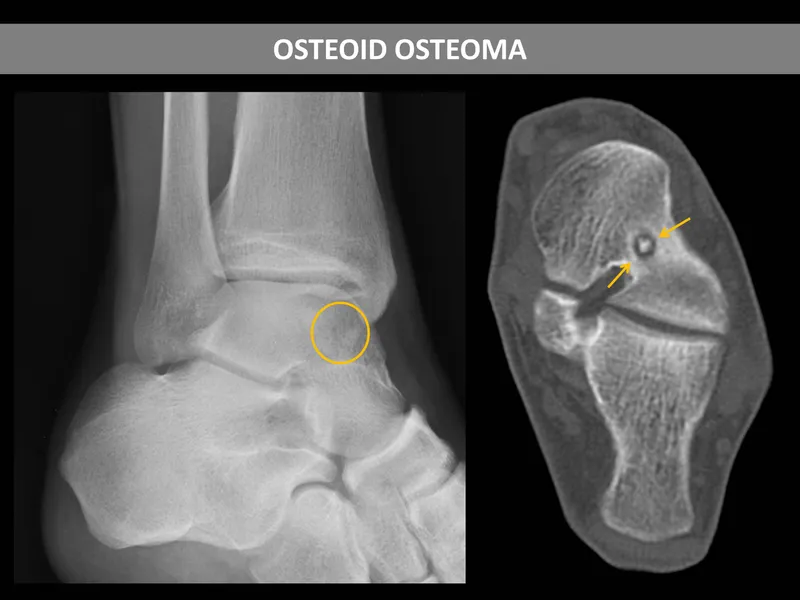
- Tx: Radiofrequency Ablation (RFA), surgical excision.
- Osteoblastoma:
- "Giant Osteoid Osteoma" (nidus > 2 cm). Spine, long bones.
- Pain: Dull, achy; less responsive to NSAIDs.
- X-ray: Expansile, lytic or mixed lytic/sclerotic lesion.
- Tx: Curettage, bone grafting, marginal excision.
- Osteoid Osteoma:
- Chondrogenic (Cartilage-Forming):
- Osteochondroma (Exostosis):
- Most common benign bone tumor. Cartilage-capped bony projection from bone surface.
- Location: Metaphysis of long bones (esp. knee, proximal humerus).
- Sessile or pedunculated. Malignant transformation risk < 1% (solitary).
- X-ray: Bony outgrowth continuous with cortex & medulla of parent bone.
- Enchondroma:
- Benign hyaline cartilage tumor within medullary cavity.
- Location: Small bones of hands/feet (most common), long bones.
- X-ray: Well-defined lytic lesion; chondroid matrix calcification ("rings & arcs").
- Associated with Ollier's disease, Maffucci's syndrome.
- Chondroblastoma: 📌 "Codman's tumor"
- Age: 10-25 yrs (skeletally immature).
- Location: Epiphysis or apophysis of long bones (knee, proximal humerus).
- X-ray: Well-defined lytic lesion in epiphysis, may have sclerotic rim, spotty calcification (chicken-wire).
- Osteochondroma (Exostosis):
GCT, Fibrous Dysplasia & Others - Cellular Crowds & Bony Blends
-
Giant Cell Tumor (GCT / Osteoclastoma)
- Age 20-40 yrs (skeletally mature).
- Epiphysis (distal femur, prox tibia).
- X-ray: Eccentric, lytic, "soap bubble". Locally aggressive.

- Histo: Stromal cells, giant cells.
- Tx: Curettage + adjuvant. Denosumab (unresectable).
⭐ Giant Cell Tumors (GCT) typically occur in the epiphysis of long bones in skeletally mature individuals (20-40 years).
-
Fibrous Dysplasia (FD)
- GNAS1 mutation; developmental.
- Monostotic or Polyostotic.
- McCune-Albright: Polyostotic, café-au-lait, endocrinopathy. 📌 MAP.
- X-ray: "Ground-glass", Shepherd's crook.
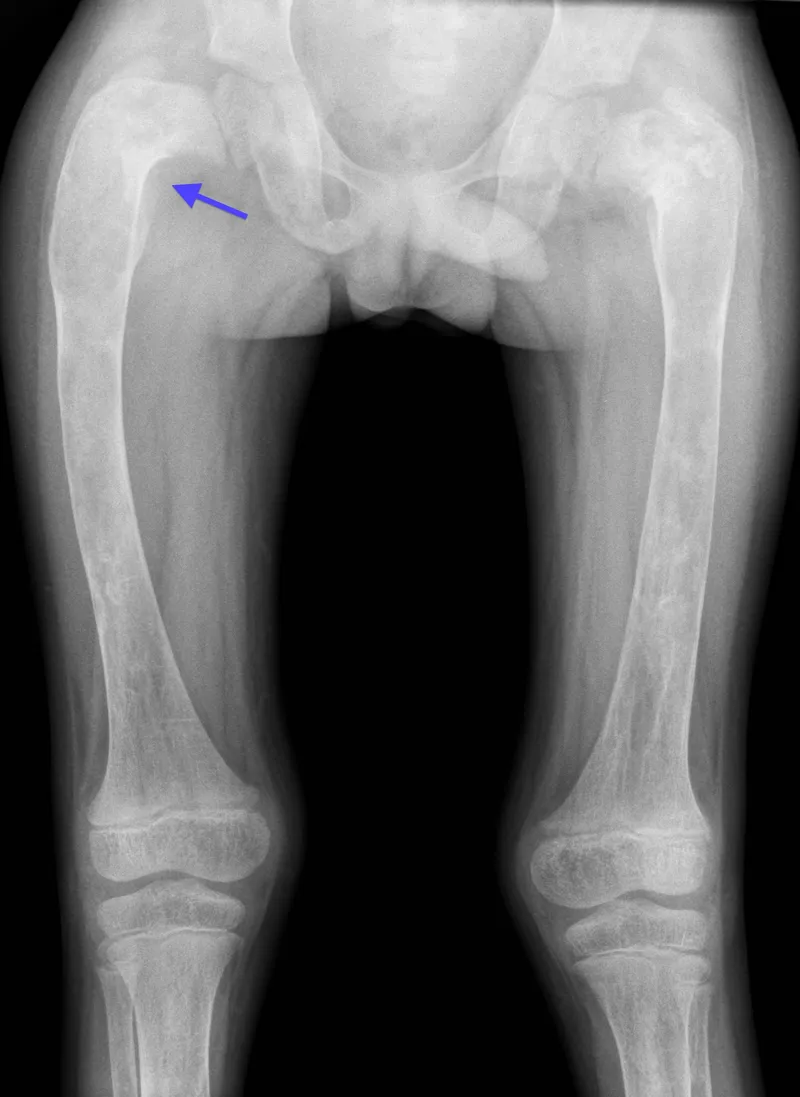
- Histo: "Chinese letters" (woven bone).
-
Other Benign Lesions
- Aneurysmal Bone Cyst (ABC)
- Age <20 yrs; metaphysis.
- X-ray: Expansile, lytic; fluid-fluid levels (MRI).
- Simple Bone Cyst (UBC)
- Age 5-15 yrs; prox humerus/femur.
- X-ray: Central, lytic; "fallen leaf" sign (fractured).
- Aneurysmal Bone Cyst (ABC)
Benign Tumors: Diagnosis & Management - Spot & Sort Strategies
- Initial Dx: X-ray (location, margins, matrix, periosteal reaction).
- "Leave-me-alone" lesions: Classic benign features, asymptomatic: observe (e.g., NOF).
- Symptomatic/Aggressive/Uncertain:
- Further imaging: CT (cortical, matrix), MRI (soft tissue, marrow).
- Biopsy: Excisional (small, accessible) or incisional (large/complex).
- Management:
- Observation: Asymptomatic, stable.
- Curettage (+/- adjuvants: phenol, cryo, graft/cement).
- Excision (marginal/wide): e.g., GCT, osteoblastoma.
⭐ Most asymptomatic, incidentally discovered benign bone lesions in children (e.g., Non-Ossifying Fibroma) can be safely observed with serial radiographs.
High‑Yield Points - ⚡ Biggest Takeaways
Error generating content for this concept group: Failed to process successful response
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

