Pathophysiology & Risk Factors - Triad Trouble
- Core Pathophysiological Triad:
- Neuropathy: Sensory (Loss Of Protective Sensation - LOPS), motor (muscle imbalance → deformities like claw toes, Charcot), autonomic (anhidrosis → dry, cracked skin).
- Angiopathy (PAD): Atherosclerosis → ↓ blood flow, ↓ oxygen & nutrient delivery, impaired wound healing. Affects distal vessels.
- Immunopathy: Impaired leukocyte function, ↓ chemotaxis & phagocytosis, blunted inflammatory response → ↑ infection susceptibility.
- Key Risk Factors:
- Uncontrolled DM (HbA1c > 7%)
- DM duration > 10 years
- Previous DFU/amputation
- Structural foot deformity
- Limited joint mobility
- Poor footwear, smoking
- Visual impairment, nephropathy
⭐ Peripheral neuropathy is the primary factor in the development of diabetic foot ulcers.
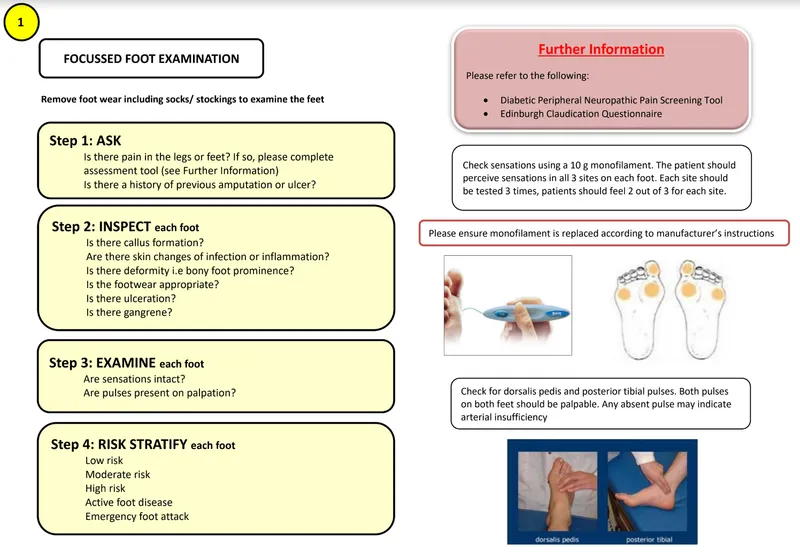
Clinical Assessment & Diagnosis - Spotting the Signs
- History: DM duration, glycemic control, neuropathy symptoms (pain, numbness), claudication, prior ulcers.
- Examination:
- Inspect: Deformities (Charcot, claw/hammer toes), calluses, ulcers (site, size, depth, base, discharge), skin (dry, fissures, hair loss, infection signs).
- Palpate: Skin temperature, tenderness, pulses (DP, PT), Capillary Refill Time.
- Neuropathy: 10g Semmes-Weinstein Monofilament (SWMT), 128Hz tuning fork (vibration).
- Vascular: Ankle-Brachial Index (ABI).
⭐ An Ankle-Brachial Index (ABI) < 0.9 suggests Peripheral Arterial Disease (PAD).
- Key Investigations:
- X-ray: Osteomyelitis, gas, foreign body, Charcot.
- MRI: Gold standard for osteomyelitis, deep abscess.
- Doppler Ultrasound: Assesses arterial flow.
- Wound Culture: For targeted antibiotics.
Classification & Charcot Foot - Grading the Grief
Diabetic Foot Ulcer Classification:
- Wagner Classification: Key system for severity.
- Grade 0: Intact skin, may have bony deformity (pre-ulcerative).
- Grade 1: Superficial ulcer (skin only).
- Grade 2: Ulcer extending to ligament, tendon, joint capsule, or deep fascia (no bone/abscess).
- Grade 3: Deep ulcer with abscess, osteomyelitis, or septic arthritis.
- Grade 4: Gangrene of a portion of the forefoot or heel.
- Grade 5: Extensive gangrene of the entire foot.
- University of Texas (UT) Classification:
- Matrix: Combines ulcer depth (Grades 0-III) with presence of Infection and/or Ischemia (Stages A-D).
Charcot Neuroarthropathy:
- Progressive, non-infectious, destructive process affecting bones, joints, and soft tissues, typically in individuals with neuropathy.
- Acute phase: Presents as a red, hot, swollen foot; often misdiagnosed as infection.
- Eichenholtz Classification (Modified):
⭐ Wagner Grade 3 ulcer involves deep infection with abscess, osteomyelitis, or septic arthritis.
Management & Prevention - Healing & Halting
- Multidisciplinary Team: Key.
- Wound Care:
- Sharp debridement.
- Moist wound dressings (hydrocolloids, alginates).
- NPWT for select wounds.
- Infection Control:
- Mild: Oral antibiotics.
- Mod/Severe: IV Abx, surgical debridement.
- Deep tissue cultures.
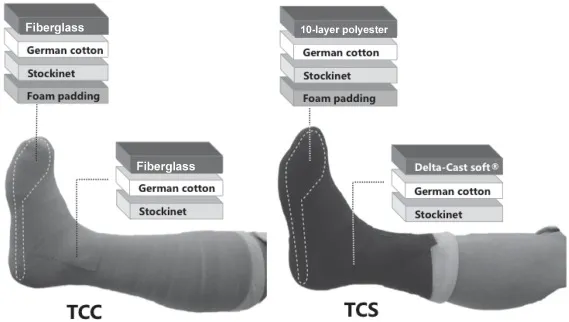
- Offloading (Key for Neuropathic Ulcers):
⭐ Total Contact Casting (TCC) is the gold standard for offloading neuropathic plantar ulcers.
- Alternatives: Removable Cast Walkers (RCW), therapeutic shoes.
- Vascular Management:
- Assess: ABI < 0.9 or > 1.3 (calcification) needs vascular studies.
- Revascularization for PAD.
- Surgical Interventions:
- Debridement, I&D.
- Charcot reconstruction.
- Amputations (minor/major) last resort.
- Prevention (Halting Progression):
- Glycemic control (HbA1c < 7%).
- Education: Daily foot inspection, hygiene, nail care.
- Therapeutic footwear, orthotics.
- Podiatric care.
- 📌 Mnemonic: "FOOT CARE" (Footwear, Observe daily, Offloading, Test sensation, Control sugar, Annual check-up, Refer early, Educate).
High‑Yield Points - ⚡ Biggest Takeaways
- Diabetic Foot triad: neuropathy (sensory loss), angiopathy (poor circulation), and immunodeficiency.
- Charcot neuroarthropathy: progressive destruction causing rocker-bottom foot deformity.
- Wagner classification (Grades 0-5) is essential for ulcer staging.
- Management pillars: strict glycemic control, wound debridement, effective offloading (e.g., Total Contact Cast), and targeted antibiotics.
- Always assess for Peripheral Vascular Disease; revascularization may be needed.
- Osteomyelitis is a common, severe complication requiring prompt, aggressive treatment.
- Prevention is key: patient education, daily foot inspection, and appropriate footwear.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

