Osteoarthritis of Ankle and Foot - Wear & Tear Tale
- Progressive "wear & tear" disease leading to cartilage degradation and osteophyte formation.
- Ankle OA: Predominantly secondary, often post-traumatic (>70% of cases).
- Foot OA: Can be primary or secondary.
- Key joints affected:
- Ankle (tibiotalar)
- Hindfoot: Subtalar
- Midfoot: Talonavicular, cuneiform-metatarsal
- Forefoot: First MTP (Hallux Rigidus)
⭐ Unlike knee/hip OA, ankle OA is most commonly secondary to trauma (e.g., previous fractures or ligament injuries).
Osteoarthritis of Ankle and Foot - Joint Under Siege
- Often post-traumatic (70-80%); less common than knee/hip OA.
- Key sites: Ankle (tibiotalar), talonavicular, subtalar, 1st MTPJ (hallux rigidus).
- Symptoms: Activity-related pain, morning stiffness < 30 min, swelling, ↓ ROM.
- X-ray: ↓ Joint space, osteophytes, subchondral sclerosis & cysts.

- Management:
- Non-operative: NSAIDs, activity modification, orthotics (e.g., rocker bottom shoes, ankle brace), physiotherapy, intra-articular steroid injections.
- Operative: Arthrodesis (fusion - gold standard for ankle), arthroplasty (joint replacement - for selected cases, e.g., 1st MTPJ).
⭐ The talonavicular joint is the most common site of midfoot arthritis, often presenting with dorsal midfoot pain.
Osteoarthritis of Ankle and Foot - Groans & Limps
-
Progressive cartilage loss and osteophyte formation in ankle/foot joints. Ankle OA often post-traumatic.
-
Clinical: Activity-related pain ("groans"), morning stiffness < 30 mins, ↓ROM, crepitus, deformity, limp.
-
Common Sites: Ankle (tibiotalar), subtalar, talonavicular, 1st MTP (Hallux Rigidus).
-
X-ray (Weight-bearing): Joint space narrowing, osteophytes, subchondral sclerosis, cysts.
-
Management:
- Conservative: NSAIDs, physiotherapy, orthotics (e.g., rocker sole, ankle brace), injections.
- Surgical: Arthrodesis (fusion) is common; ankle arthroplasty (replacement) is an option.
⭐ Post-traumatic arthritis is the most common cause of ankle osteoarthritis, unlike primary OA in hip/knee.
Osteoarthritis of Ankle and Foot - X-Rays & Grades
X-rays confirm diagnosis. Key findings (📌 LOSS):
- Loss of joint space: Often asymmetric, especially in weight-bearing views.
- Osteophytes: Marginal bony outgrowths.
- Subchondral sclerosis: Increased bone density (↑) beneath cartilage.
- Subchondral cysts: Fluid-filled cavities in bone.
Kellgren-Lawrence (K-L) Grading:
⭐ Ankle OA is predominantly post-traumatic (secondary); foot OA commonly affects talonavicular and 1st MTP joints.
Osteoarthritis of Ankle and Foot - Easing the Ache
- Conservative Management (First-line):
- Lifestyle: Weight ↓, low-impact activity.
- PT: ROM, strengthening, proprioception.
- Orthotics: AFO, specialized footwear, inserts.
- Meds: NSAIDs (topical/oral), paracetamol.
- Injections: Corticosteroids (temp. relief), Hyaluronic acid.
- Surgical Management (Refractory cases):
- Arthroscopic debridement: Synovectomy, loose bodies.
- Arthrodesis (Fusion): Gold standard for end-stage ankle/subtalar/midfoot OA.
⭐ Tibiotalar arthrodesis: gold standard for severe ankle OA, provides pain relief & stability.
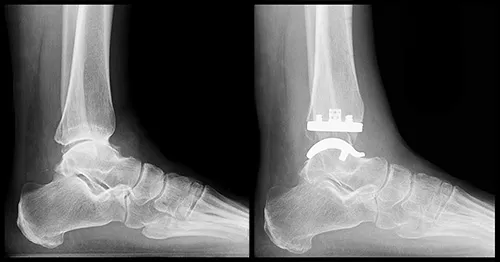
- Total Ankle Arthroplasty (TAA): Motion-sparing for select isolated ankle OA.
- Osteotomies: Corrective for malalignment.
High‑Yield Points - ⚡ Biggest Takeaways
- Ankle OA is mainly post-traumatic; foot OA commonly hits talonavicular & 1st MTPJ.
- Symptoms: Activity-related pain, morning stiffness (<30 min), crepitus, decreased ROM.
- X-ray: Asymmetric joint space narrowing, osteophytes, subchondral sclerosis, cysts.
- Conservative: NSAIDs, weight loss, activity modification, orthotics, corticosteroid injections.
- Ankle arthrodesis is gold standard surgery for severe tibiotalar OA.
- First MTPJ OA (hallux rigidus) often needs cheilectomy or arthrodesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

