CAJR Fundamentals - Precision Piloting
- Goal: Enhance surgical accuracy & precision in joint replacement (arthroplasty).
- Principle: Utilizes computer systems for:
- Pre-operative planning (3D models).
- Intra-operative navigation (real-time guidance).
- Robotic assistance (controlled bone cuts/implant placement).
- Benefits:
- Improved implant positioning & alignment.
- Reduced outliers in component placement.
- Potential for ↑ implant longevity & ↓ revision rates.
- Core Components: Tracking systems (optical, electromagnetic), specialized software, surgeon interface.
⭐ CAJR aims to restore the mechanical axis of the limb to within ±3° of neutral, a key factor for TKA longevity.
CAJR Technologies - The Digital Toolkit
Key tools for precision joint replacement:
- Imaging Modalities:
- Image-Based: Pre-op CT/MRI for detailed 3D planning. Intra-op registration crucial.
- Imageless: Intra-op kinematic/fluoroscopic data for landmarking. Avoids pre-op CT.
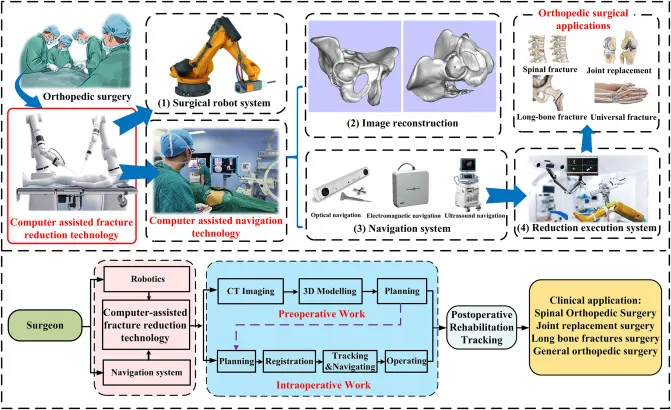
- Navigation Systems (Real-time Tracking):
- Optical: Uses infrared cameras & passive/active reflective markers.
- Electromagnetic: Uses sensors tracked within a generated magnetic field.
- Robotic Assistance Types:
- Haptic (Tactile): Surgeon-guided with robotic boundaries, offering tactile feedback (e.g., Stryker MAKO).
- Active: Robot autonomously executes pre-planned surgical steps (rare in modern joint CAJR).
- Shared-Control: Dynamic collaboration between surgeon and robot for task execution.
⭐ Most haptic robotic systems for knee/hip arthroplasty (e.g., MAKO) utilize CT-derived 3D models for pre-operative planning and provide tactile feedback to constrain bone resection.
CAJR in Action - Surgical Steps & Scope
-
Surgical Workflow:
-
Critical Intra-operative Phases:
- Registration: Links patient's actual anatomy to the digital pre-operative plan.
- Paired-point: Uses defined anatomical landmarks.
- Surface matching: Maps bone surface contours.
- Navigation: Provides dynamic referencing; real-time visual guidance for surgical precision.
- Registration: Links patient's actual anatomy to the digital pre-operative plan.
-
Common Applications & Goals:
- TKA: Accurate femoral/tibial cuts & component alignment (mechanical/kinematic), optimal gap balancing.
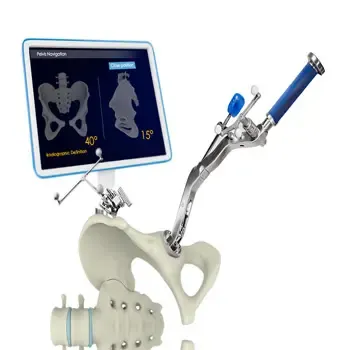
- THA: Precise acetabular cup orientation (inclination 40°±10°, anteversion 15°±10°), femoral stem version, leg length & offset restoration.
⭐ CAJR helps achieve planned implant positioning with high accuracy, aiming to reduce malalignment-related complications.
CAJR: Edge & Hurdles - Balancing Benefits
- Edge (Advantages):
- ↑ Accuracy & precision in implant alignment.
- ↑ Reproducibility of results.
- Potential for ↑ long-term outcomes & implant survival.
- ↓ Outliers in component positioning.
- Facilitates minimally invasive surgery (MIS).
- Intraoperative data & real-time feedback.
- Hurdles (Disadvantages):
- ↑ Initial equipment cost.
- Steep learning curve.
- ↑ Operative time (esp. initially).
- Specific complications:
- Pin-site issues (infection, fracture).
- Neurovascular injury from pins.
- Radiation exposure (CT-based systems).
- System errors/malfunctions risk.
- Balancing Act:
- Universal superiority evidence debated.
- Best for complex cases, revisions, or less experienced surgeons.
⭐ CAJR aims to restore mechanical axis to within 3° of neutral, crucial for implant longevity.
High‑Yield Points - ⚡ Biggest Takeaways
- CAS significantly improves prosthetic alignment and positioning accuracy in arthroplasty.
- Reduces outliers in component placement, aiming for optimal mechanical axis restoration.
- Employs image-based (CT scans) or imageless (kinematic, surface registration) techniques.
- Optical or electromagnetic trackers are key for intraoperative navigation.
- Benefits include potentially better long-term implant survival and functional outcomes.
- Crucial for complex cases, severe deformities, and revision surgeries.
- May lead to decreased blood loss and fat embolism risk_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

