Classification of Bone Tumors - Tumor Blueprint
-
Fundamental Principles:
- Histogenesis (Cell of Origin): E.g., Osteogenic (bone-forming), Chondrogenic (cartilage-forming), Fibrogenic, Hematopoietic (marrow cells), Vascular.
- Biological Behavior:
- Benign (e.g., Osteoma, Enchondroma)
- Intermediate (locally aggressive, e.g., Giant Cell Tumor; or rarely metastasizing)
- Malignant (e.g., Osteosarcoma, Chondrosarcoma, Ewing Sarcoma)
- Origin: Primary (arises in bone) vs. Secondary (metastatic, e.g., from breast, lung, prostate).
-
WHO Classification: International standard, integrates morphology, genetics, and clinical behavior.
⭐ Osteosarcoma is the most common non-hematopoietic primary malignant bone tumor, typically affecting metaphysis of long bones in adolescents.
Classification of Bone Tumors - Gentle Giants
- Osteogenic (Bone-forming):
- Osteoid Osteoma: < 2 cm, night pain (NSAID relief), nidus.
- Osteoblastoma: > 2 cm, similar histology, less pain. Spine common.
- Chondrogenic (Cartilage-forming):
- Osteochondroma: Most common. Cartilage-capped exostosis (metaphysis). 📌 Mnemonic: "Osteo-CONE-droma" (cone-shaped).
- Enchondroma: Medullary cartilage. Hands/feet. Ollier's, Maffucci's.
- Chondroblastoma: Epiphyseal. "Chicken-wire" calcification.
- Fibrogenic:
- Non-Ossifying Fibroma (NOF): Children, eccentric, lytic, sclerotic rim.
- Other Origin:
- Giant Cell Tumor (GCT): Epiphyseal (mature). Locally aggressive. "Soap bubble".
- Aneurysmal Bone Cyst (ABC): Expansile, lytic, blood-filled spaces. Fluid-fluid levels on MRI.
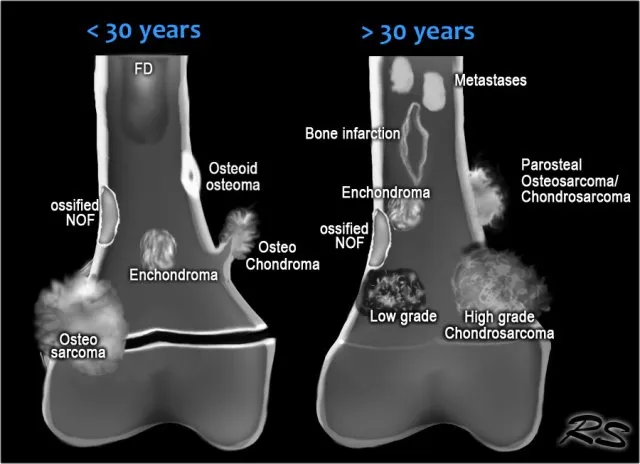
⭐ Osteoid Osteoma classically presents with nocturnal pain dramatically relieved by NSAIDs/aspirin.
Classification of Bone Tumors - Bone Breakers
- Primary Malignant Tumors: Arise from bone/cartilage.
- Osteosarcoma: Most common (excl. myeloma); bone-forming.
- Age: 10-20 yrs (peak), also >50 yrs.
- Sites: Metaphysis (knee, proximal humerus).
- X-ray: Sunburst, Codman's triangle.
- Ewing Sarcoma: Small round blue cell tumor; aggressive.
- Age: 10-20 yrs.
- Sites: Diaphysis (long bones, pelvis).
- X-ray: Onion-peel, moth-eaten.
- Genetics: t(11;22) EWS-FLI1.
- Chondrosarcoma: Cartilage-producing malignancy.
- Age: >40 yrs.
- Sites: Pelvis, femur, ribs.
- X-ray: Popcorn/ring-and-arc calcification.
- Others:
- Fibrosarcoma/MFH (spindle cell)
- Malignant GCT (rare transformation)
- Chordoma (notochordal; sacrum, clivus)
- Adamantinoma (low-grade; tibia)
- Osteosarcoma: Most common (excl. myeloma); bone-forming.
⭐ Ewing Sarcoma is highly radiosensitive & chemosensitive, unlike Osteosarcoma (radioresistant; surgery + chemo primary).
Classification of Bone Tumors - Masqueraders & Invaders
- Masqueraders (Tumor-like Lesions): Mimic tumors; non-neoplastic.
- Fibrous Dysplasia: Ground-glass appearance, Shepherd's crook deformity.
- Simple Bone Cyst (SBC/UBC): Central, lytic, "fallen leaf" sign.
- Aneurysmal Bone Cyst (ABC): Eccentric, expansile, blood-filled; fluid-fluid levels.
- Brown Tumor: Due to hyperparathyroidism.
- Osteomyelitis: Bone infection.
- Eosinophilic Granuloma (LCH): Vertebra plana, punched-out lytic lesions.
- Invaders (Metastatic Disease):
- Most common bone malignancy overall.
- Common Primaries: 📌 PBL KT (Prostate, Breast, Lung, Kidney, Thyroid).
- Radiographic Types: Lytic (e.g., Lung, Kidney), Sclerotic/Blastic (e.g., Prostate), Mixed (e.g., Breast).
⭐ Metastasis is the most common malignant tumor affecting bone.
oka
High‑Yield Points - ⚡ Biggest Takeaways
- Primary division: Benign versus Malignant, dictates management approach.
- Histogenetic origin (osteogenic, chondrogenic, fibrogenic, hematopoietic) is crucial for classification.
- Patient age and tumor location (epiphysis, metaphysis, diaphysis) are vital diagnostic clues.
- Osteosarcoma: Most common primary malignant tumor, typically in metaphysis around knee.
- Ewing's Sarcoma: Pediatric diaphysis tumor, classic "onion-skin" periosteal reaction.
- Giant Cell Tumor (GCT): Locally aggressive, epiphyseal location, characteristic "soap bubble" appearance.
- Multiple Myeloma: Most common overall malignant bone tumor in adults (plasma cell origin).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

