Biomaterials 101 - Ortho's Building Blocks
- Definitions:
- Biomaterial: Material designed to interface with biological systems for medical purposes.
- Biocompatibility: Ability of a material to perform with an appropriate host response.
- Bioinert: Minimal interaction with surrounding biological tissue (e.g., Alumina, Zirconia).
- Bioactive: Elicits a specific biological response, forms a bond with tissue (e.g., Hydroxyapatite).
- Bioresorbable: Degrades in the body over time, replaced by host tissue (e.g., PLLA, PGA).
- Classes of Biomaterials:
- Key Mechanical Properties:
- Stress ($\\sigma = F/A$): Force per unit area.
- Strain ($\\\epsilon = \\\Delta L/L_0$): Deformation relative to original length.
- Young's Modulus ($E = \\sigma/\\ oluene$): Material stiffness; resistance to elastic deformation.
- Yield Strength: Stress at which permanent (plastic) deformation begins.
- Ultimate Tensile Strength (UTS): Maximum stress a material can withstand before fracture.
- Fatigue Strength: Resistance to failure under cyclic loading.
- Toughness: Energy absorbed before fracturing.
- Hardness: Resistance to localized surface indentation or scratching.
- Wear Resistance: Ability to resist material loss due to friction.
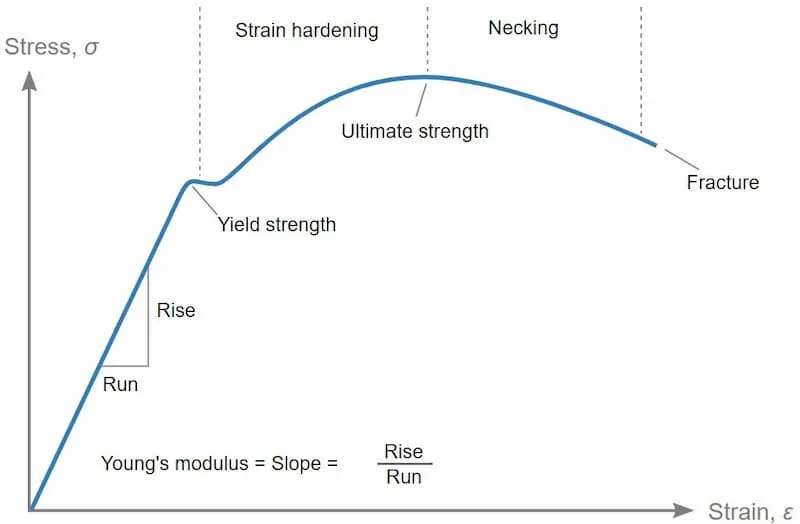
⭐ Young's Modulus of Cortical Bone is approximately 10-30 GPa. Implant materials with significantly different moduli can lead to stress shielding (bone resorption) or implant loosening due to micromotion.
Metallic Marvels - Shiny Strong Supports
Key load-bearing implants. Common alloys:
| Alloy | Properties ($E$=Young's Modulus) | Pros | Cons | Uses |
|---|---|---|---|---|
| Stainless Steel (316L) | Strength, corrosion resist. $E \approx$ 200 GPa | Low cost | Ni allergy, fretting | Plates, screws, nails |
| Co-Cr-Mo | ↑Strength, wear resist. $E \approx$ 210 GPa | Superior wear (joints) | Ion leach (Co, Cr), MoM debris | Joint replacements (heads, cups) |
| Ti-6Al-4V | Excellent biocompatibility, $E \approx$ 110 GPa (↓stress shield) | MRI safe, osseointegration | ↓Shear strength, notch sensitive | Stems, spinal/trauma implants |
Common Concerns:
- Stress Shielding: Bone loss (implant stiffness).
- Ion Leaching: Metal ion release (e.g., Co, Cr, Ni).
- Fretting/Corrosion: Interface wear.
- Metal-on-Metal (MoM) Wear Debris: Tissue reactions.
⭐ Ti-6Al-4V's Young's modulus ($E \approx$ 110 GPa) is closer to bone (cortical bone: 10-30 GPa), significantly reducing stress shielding effects compared to other metals like stainless steel or Co-Cr alloys.
Ceramics & Polymers - Articulating Aces
Ceramics and polymers offer diverse solutions in orthopaedics, from wear-resistant joint surfaces to resorbable fixation devices.
Key Ceramics in Orthopaedics
| Ceramic Type | Key Properties | Common Applications |
|---|---|---|
| Alumina ($Al_2O_3$) | High hardness, wear resistance, inert | Joint bearing surfaces (hip, knee) |
| Zirconia ($ZrO_2$) | Higher toughness & strength than alumina, inert | Femoral heads |
| Bioactive Glasses | Bonds to bone, osteoconductive | Bone graft substitutes, coatings |
| Calcium Phosphates (HA, TCP) | Osteoconductive, resorbable (TCP > HA) | Bone void fillers, coatings on implants |
| Polymer Type | Key Properties | Common Applications |
|---|---|---|
| UHMWPE | Low friction, high toughness, wear resistance | Acetabular liners, patellar components |
| PMMA (Bone Cement) | Space-filling, exothermic setting, drug elution | Joint fixation, vertebroplasty |
| PEEK | Biocompatible, radiolucent, good mechanical strength | Spinal implants (cages), trauma plates |
| Biodegradable (PLA, PGA, PLGA) | Resorbable, variable degradation rates | Sutures, screws, drug delivery systems |
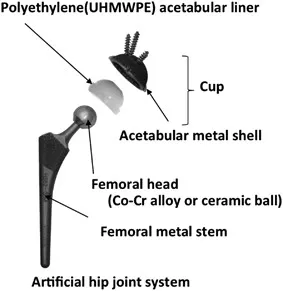
⭐ Exam Favourite: Gamma irradiation in air can cause oxidative degradation of UHMWPE, leading to ↓ wear resistance and ↑ risk of osteolysis. Modern sterilization (e.g., gas plasma, ethylene oxide, or gamma in inert gas) and cross-linking mitigate this.
Sterilization can affect polymer properties; e.g., gamma radiation can alter UHMWPE's wear characteristics if not processed correctly (cross-linking).
Host-Material Tango - Implant Immune Interface
-
Biocompatibility: A material's capacity to perform with an appropriate, specific host response in a given application.
-
Host Response Sequence: Implant triggers injury, leading to:
-
Factors Influencing Response:
- Material: Chemistry (e.g., Ti vs. CoCr), surface properties (roughness, coatings).
- Implant: Size, shape, micromotion.
- Host: Immune status, mechanical loading.
-
Wear Debris: Particulate matter from implant degradation. 📌 Particle Disease.
- Types: Metal ions, Polymer (UHMWPE), Ceramic (often inert).
- Biological Effects: Macrophage activation → osteolysis, aseptic loosening.
-
Implant-Related Infection: Biofilm formation (e.g., S. aureus, S. epidermidis) resists antibiotics & host defenses.
-
Hypersensitivity: Immune reaction to metals (e.g., Nickel, Cobalt, Chromium).
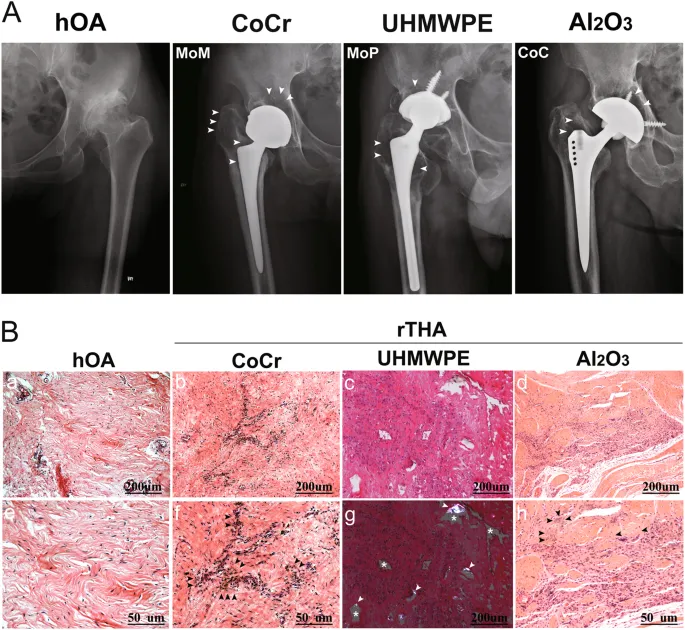
⭐ Aseptic loosening, often driven by wear debris-induced osteolysis, is a major cause of late prosthetic joint failure.
High‑Yield Points - ⚡ Biggest Takeaways
- Stress shielding: Bone resorption due to implant stiffness exceeding bone's, related to Young's Modulus mismatch.
- Biocompatibility: Material eliciting an appropriate host response.
- Bioactive materials (e.g., Hydroxyapatite, Bioglass) bond directly to bone.
- Bioinert materials (e.g., Titanium, Co-Cr alloys) form a fibrous capsule.
- Bioresorbable materials (e.g., PLLA, PGA) degrade and are replaced by host tissue.
- Wear debris (especially UHMWPE) is a major cause of aseptic loosening of implants.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

