Pediatric Cataract Basics - Cloudy Peepers Primer
- Lens opacity in children; key cause of treatable childhood blindness.
- Types: Congenital (at birth or <1 yr), infantile, developmental, traumatic.
- Etiology:
- Genetic (most common)
- Metabolic (e.g., galactosemia)
- Intrauterine infections (TORCH)
- Trauma, Idiopathic
- Signs: Leukocoria (white pupil), strabismus, nystagmus, poor fixation.
⭐ Leukocoria is the most common presenting sign of pediatric cataract.
- Early diagnosis & intervention crucial to prevent amblyopia.

Etiology & Classification - Cataract Culprits Lineup
- Etiology:
- Idiopathic/Sporadic: Most common (approx. 50%).
- Hereditary: Autosomal Dominant (AD, most common inherited), Autosomal Recessive (AR), X-linked. Genes: CRY, GJA.
- Maternal Infections (TORCH): Rubella (Gregg's triad), Cytomegalovirus (CMV), Toxoplasmosis.
- Metabolic: Galactosemia (oil-droplet, reversible), Lowe syndrome, Hypoglycemia.
- Trauma: Penetrating, blunt.
- Drugs: Corticosteroids (prolonged use).
- Radiation.
- Syndromic: Down syndrome, Stickler syndrome, Marfan syndrome.
- Morphological Classification:
- Lamellar/Zonular: Most common congenital type; opacities around embryonic nucleus.
- Polar: Anterior or Posterior (PPC often with Mittendorf's dot).
- Nuclear: Central opacity, early onset.
- Cortical: Peripheral, spoke-like opacities.
- Sutural: Along Y-sutures, often visually insignificant.
- Total/Mature or Membranous.
- Blue-dot (Cataracta Punctata Caerulea).
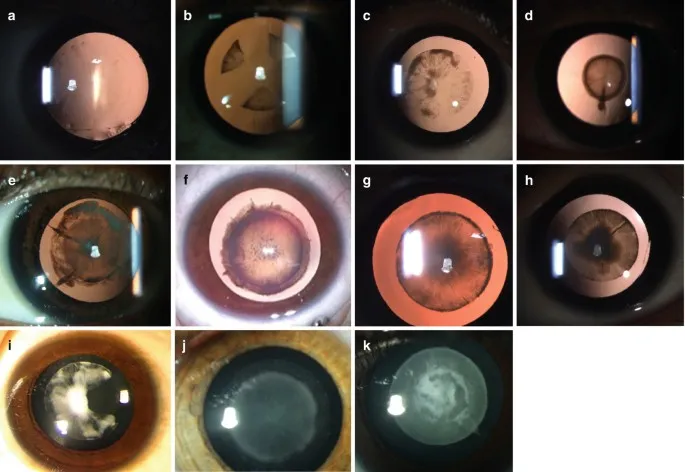
⭐ Galactosemia can cause an "oil-droplet" cataract, which may be reversible with early dietary restriction of galactose.
Clinical Features & Diagnosis - Little Eyes, Big Clues
- Presentation:
- Leukocoria (white pupil) - most common sign.
- Absent red reflex.
- Poor fixation, nystagmus (esp. bilateral, dense, early onset).
- Strabismus.
- Photophobia.
- Family history.
- Diagnostic Evaluation:
- Red Reflex Test (Bruckner): Crucial screening.
- Dim room, direct ophthalmoscope from 1 meter.
- Slit-lamp examination: Morphology (e.g., lamellar, polar, nuclear).
- Ophthalmoscopy.
- B-scan USG: If posterior view obscured.
- Systemic workup: TORCH screen, metabolic tests (e.g., for galactosemia - "oil droplet" cataract).
- Red Reflex Test (Bruckner): Crucial screening.

⭐ Leukocoria is the most common presenting sign of pediatric cataract and warrants urgent ophthalmological evaluation to prevent amblyopia.
Management Strategies - Clearing the View Path
- Surgical Timing (Critical Period):
- Unilateral dense: 4-6 weeks of birth.
- Bilateral dense: 6-8 weeks of birth.
- Partial/later onset: Individualized, based on visual significance.
- Surgical Technique:
- Lensectomy & Aspiration.
- Primary Posterior Capsulotomy (PPC).
- Anterior Vitrectomy (AV).
- Intraocular Lens (IOL) Implantation:
- Primary IOL: Typically >1 year (or >6 months). Consider deferring in neonates.
- Aphakia: If IOL deferred.
- Post-operative Management:
- Optical Correction: Aphakic glasses, contact lenses (esp. unilateral), IOL.
- Amblyopia Therapy: Crucial; patching, atropine penalization.
- Regular follow-up: Refraction, IOP monitoring.
⭐ The most common cause of poor visual outcome after pediatric cataract surgery is amblyopia, emphasizing the need for aggressive post-op therapy.
Complications & Prognosis - Post-Op Peeks & Outlook
- Post-Op: Uveitis, Posterior Capsular Opacification (PCO) (very common), Visual Axis Opacification (VAO).
- Long-Term: Amblyopia, strabismus, secondary glaucoma.
⭐ Secondary glaucoma: most common vision-threatening complication.
- Prognosis: Early surgery (<6 wks bilateral; <4-6 wks unilateral) & rigorous amblyopia therapy are key for better visual outcomes. Unilateral often poorer_._
High‑Yield Points - ⚡ Biggest Takeaways
- Leukocoria (white reflex) is the most common presentation.
- Key causes: TORCH infections (e.g., Rubella), galactosemia, trauma.
- Critical surgery: unilateral by 6 weeks, bilateral by 8 weeks to prevent amblyopia.
- Unilateral cataracts pose a higher amblyopia risk than bilateral.
- Oil-drop reflex on retroillumination suggests galactosemic cataract.
- Posterior lenticonus is a common cause of progressive unilateral cataract.
- Lifelong aphakic correction and amblyopia therapy are essential post-surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

