Glaucoma Surgery: Aims & Classification - Pressure Busters
- Aims of Surgery:
- Achieve target ↓ IOP (Intraocular Pressure)
- Prevent further optic nerve damage & visual field loss
- Preserve long-term vision
- General Indications:
- Medication/laser failure or intolerance
- Rapid disease progression despite therapy
- Poor patient compliance with medical treatment
- Target IOP not achieved with non-surgical means
- Broad Classification:
- Enhancing Aqueous Outflow (Filtration Surgery):
- Trabeculectomy (conventional, guarded filtration)
- Glaucoma Drainage Devices (GDDs) / Setons / Valves
- Minimally Invasive Glaucoma Surgery (MIGS) - various devices
- Non-Penetrating Glaucoma Surgery (NPGS) - e.g., deep sclerectomy
- Reducing Aqueous Production:
- Cyclodestructive procedures (e.g., cyclocryotherapy, Transscleral Cyclophotocoagulation - TCP)
- Enhancing Aqueous Outflow (Filtration Surgery):
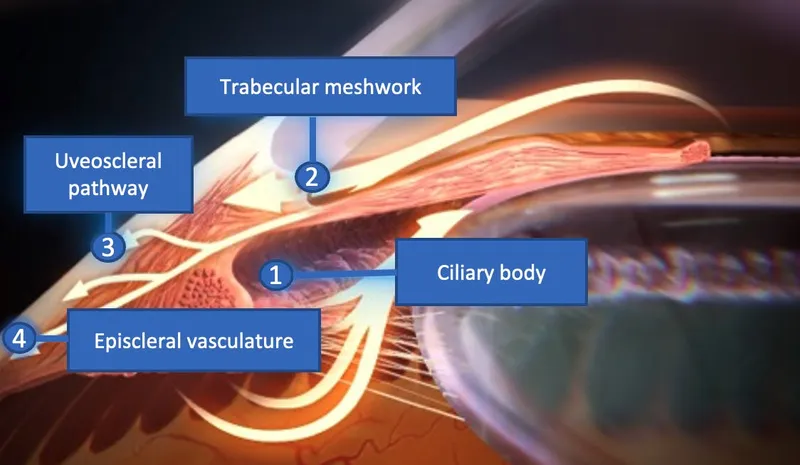
⭐ The primary goal of glaucoma surgery is to lower intraocular pressure to a level that prevents further optic nerve damage and vision loss.
Trabeculectomy - The Gold Standard Drain
- Mechanism: Creates new subconjunctival aqueous humor outflow pathway via a guarded fistula (scleral flap, sclerostomy/punch) to form a filtration bleb.
- Key Steps:
- Conjunctival & scleral flap (partial thickness)
- Sclerostomy (punch)
- Peripheral Iridectomy (PI)
- Antimetabolites (MMC, 5-FU)
- Flap suturing → bleb formation
- Antimetabolites:
- Mitomycin C (MMC): $0.2-0.4 \text{ mg/ml}$ for 1-5 mins. Alkylating agent.
- 5-Fluorouracil (5-FU): $50 \text{ mg/ml}$ for 5 mins (injections). Pyrimidine analog.
- Complications:
- Early: Hypotony, shallow AC, choroidal effusion/hemorrhage, malignant glaucoma.
- Late: Bleb leak, blebitis/endophthalmitis, bleb encapsulation/failure, cataract.
- 📌 Mnemonic (BLECH): Bleb leak, Low IOP, Endophthalmitis, Choroidal detachment, Hypotony.

⭐ Avascular, cystic bleb (MMC-associated) is at higher risk for late bleb leaks and blebitis.
Glaucoma Drainage Devices & MIGS - Tubes 'n' Tech
-
Glaucoma Drainage Devices (GDDs / Tube Shunts): Aqueous shunted to an external subconjunctival reservoir plate.
-
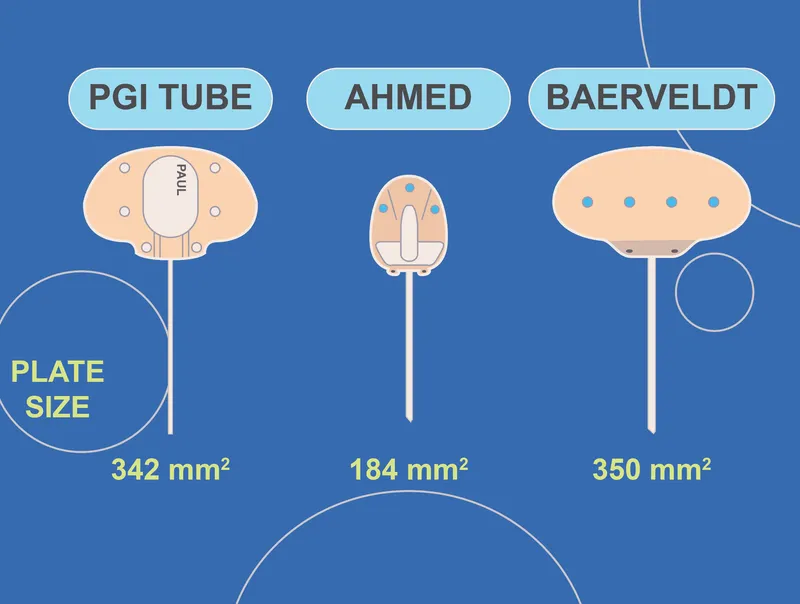
Types & Key Differences:
Feature Valved (e.g., Ahmed - AGV) Non-valved (e.g., Baerveldt - BGI, Molteno) Mechanism Flow-restrictor valve No valve (requires temporary ligation/stent) Early IOP Ctrl Immediate Delayed (awaits suture lysis/absorption) Plate Size Generally smaller Generally larger (may achieve lower long-term IOP) -
Indications: Complex glaucomas (neovascular, uveitic, traumatic), failed previous trabeculectomy(s), congenital/juvenile glaucoma.
-
Complications: Hypotony (esp. non-valved if not properly ligated), tube-corneal endothelial damage, tube erosion/exposure, diplopia, plate encapsulation (Tenon's cyst).
-
-
Minimally Invasive Glaucoma Surgery (MIGS): Typically ab-interno approach, less tissue disruption, better safety profile, often combined with cataract surgery.
- Classification by Outflow Target:
- Trabecular Meshwork Bypass: e.g., iStent, Hydrus, KDB (Kahook Dual Blade), GATT (Gonioscopy-Assisted Transluminal Trabeculotomy).
- Suprachoroidal Space: e.g., Cypass (withdrawn); newer devices emerging.
- Subconjunctival Space: e.g., XEN Gel Stent.
- Advantages: High safety, rapid recovery, conjunctival sparing.
- Disadvantages: Generally modest IOP reduction, often not for advanced glaucoma.

- Classification by Outflow Target:
⭐ MIGS procedures are generally preferred for mild to moderate glaucoma, especially when combined with cataract surgery, due to their favorable safety profile and less invasive nature compared to traditional surgeries like trabeculectomy or GDDs.
Cyclodestructive Procedures - Ciliary Body Cooldown
- Mechanism: Ablation of ciliary body epithelium → ↓ aqueous humor production.
- Indications: Refractory glaucoma (failed surgeries/GDDs), poor visual potential, painful blind eye, neovascular glaucoma, unfit for incisional surgery.
- Types:
- Transscleral Cyclophotocoagulation (TSCPC): Diode/Nd:YAG laser applied externally. Avoid 3 and 9 o'clock meridians (long posterior ciliary nerves/arteries).
- Endoscopic Cyclophotocoagulation (ECP): Direct laser to ciliary processes via intraocular probe; often with cataract surgery.
- Cyclocryotherapy: Older, less controlled, ↑ inflammation; rarely used.
- Complications: Significant pain, inflammation (uveitis), hypotony, phthisis bulbi, vision loss, cataract (phakic), sympathetic ophthalmia (very rare).
⭐ Micropulse TSCPC is a newer modification aiming to reduce collateral damage and inflammation compared to continuous wave TSCPC.
High‑Yield Points - ⚡ Biggest Takeaways
- Trabeculectomy: Gold standard surgery, creates a filtering fistula; MMC/5-FU prevent bleb failure.
- Glaucoma Drainage Devices (GDDs): Implanted for refractory glaucoma or after failed trabeculectomy.
- MIGS: Safer, less invasive options targeting outflow pathways; generally less IOP lowering than trabeculectomy.
- Cyclodestructive procedures (e.g., cyclophotocoagulation): Reduce aqueous production; for refractory or painful blind eyes.
- Key complications: Hypotony, bleb leak/itis, endophthalmitis, cataract, and aqueous misdirection.
- Aqueous misdirection (malignant glaucoma): Presents with high IOP and a flat/shallow anterior chamber post-surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

