Orbital Blueprint - Setting the Stage
- Anatomy: Orbit formed by 7 bones. Key landmark: Orbital septum (fibrous sheet dividing anterior/posterior).
- Crucial Spaces (re: Septum):
- Preseptal: Anterior to septum. Vision, motility typically normal.
- Postseptal (Orbital): Posterior to septum. High risk: ↓vision, proptosis, ophthalmoplegia.
- Inflammation Types:
- By Location: Preseptal vs. Postseptal (critical distinction!)
- By Etiology: Infectious vs. Non-infectious (e.g., TED, IOI/NSOI).
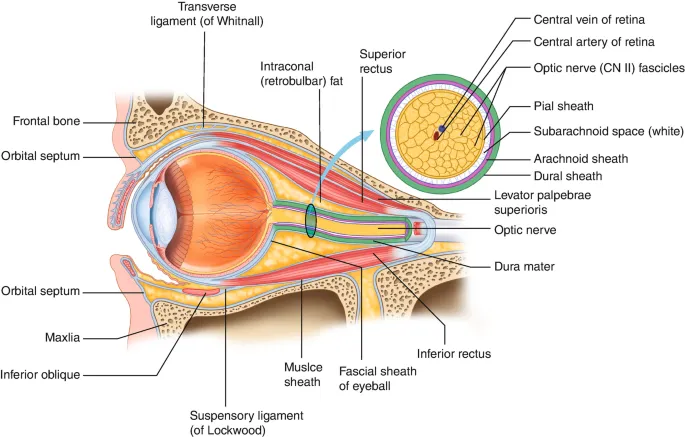
⭐ The orbital septum is the key anatomical boundary; postseptal inflammation implies true orbital involvement and higher urgency.
Infection Invasion - Orbital Alert
-
Key Distinction: Location relative to orbital septum.
- Preseptal Cellulitis (Periorbital): ANTERIOR. Lid swelling, erythema, warmth. NO proptosis, NO ophthalmoplegia, normal vision.
- Orbital Cellulitis: POSTERIOR. EMERGENCY! Proptosis, painful ophthalmoplegia, ↓ vision, afferent pupillary defect (APD).
-
Common Pathogens: S. aureus, Strep. pneumoniae, H. influenzae. Fungi (e.g., Mucor) in immunocompromised.
-
Sources: Sinusitis (esp. ethmoid), dacryocystitis, trauma, dental.
-
Management Approach:

-
Complications (Orbital): Optic neuropathy, cavernous sinus thrombosis, intracranial spread. ⚠️ High risk with delayed treatment.
⭐ > In children, ethmoid sinusitis is the most common precursor to orbital cellulitis.
Steroid Squad - Fiery Orbits
- Idiopathic Orbital Inflammatory Disease (IOID) / Orbital Pseudotumor: Non-infectious, non-neoplastic inflammation.
- Presentation: Acute painful proptosis, diplopia, chemosis, ↓ vision, restricted EOM.
- Types: Dacryoadenitis, myositis (commonest), scleritis, perineuritis, diffuse.
- Investigations:
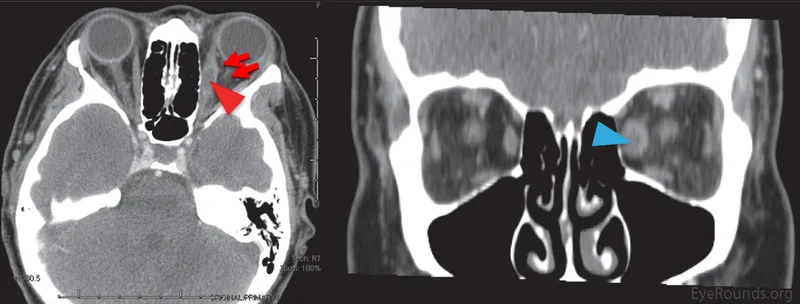
- CT/MRI: Diffuse inflammation, muscle belly enlargement (tendon sparing vs TED).
- Biopsy: Rules out lymphoma, vasculitis (GPA), IgG4-RD.
⭐ Biopsy is crucial in atypical/recalcitrant IOID to exclude malignancy (lymphoma) or specific inflammations like IgG4-related disease.
- Treatment:
- Corticosteroids (oral prednisolone 1-1.5 mg/kg/day); rapid response.
- Radiotherapy (20-30 Gy) for steroid-resistant/dependent cases.
- Immunosuppressants (MTX, AZA), Biologics for refractory IOID.
- Tolosa-Hunt Syndrome: IOID of cavernous sinus/SOF. Painful ophthalmoplegia (CN III, IV, VI). Steroid-responsive.
- 📌 S.O.A.P. for IOID: Swelling, Ophthalmoplegia, Acute, Pain.
Graves' Gaze - Thyroid's Fury
- Patho: Autoimmune; TSH-R Abs on orbital fibroblasts → GAGs, adipogenesis, muscle swelling.
- Clinical Features:
- Proptosis.
- Lid retraction (Dalrymple's).
- Diplopia: restrictive myopathy (Muscles: Inf > Med > Sup > Lat - 📌 IMSLO).
- Compressive Optic Neuropathy (CON): emergency!
- Exposure keratopathy.
- Signs (NO SPECS):
- No signs/symptoms.
- Only signs (lid retraction).
- Soft tissue (edema, chemosis).
- Proptosis (>22 mm / >2 mm asymm).
- EOM involvement (diplopia).
- Corneal.
- Sight loss (CON).

- Investigations:
- TFTs, TRAb.
- CT/MRI Orbit: EOM belly ↑, tendon sparing.
- Management:
- Mild: Lubricants, Selenium, stop smoking.
- Mod-Severe (active): IV Methylprednisolone, Teprotumumab.
- Inactive: Orbital decompression, strabismus/lid surgery.
⭐ Most common muscle affected in TED is the Inferior Rectus.
High‑Yield Points - ⚡ Biggest Takeaways
- Orbital cellulitis: Post-septal infection, often from ethmoidal sinusitis. Key signs: proptosis, painful ophthalmoplegia, ↓vision.
- Preseptal cellulitis: Anterior to septum. No proptosis, no ophthalmoplegia; normal vision & ocular motility.
- Thyroid Eye Disease (TED): Most common cause of adult proptosis (unilateral/bilateral). Use NO SPECS for staging.
- Idiopathic Orbital Inflammatory Disease (IOID): Painful ophthalmoplegia; a diagnosis of exclusion. Responds dramatically to steroids.
- Tolosa-Hunt Syndrome: Granulomatous inflammation of cavernous sinus/SOF causing painful ophthalmoplegia & cranial neuropathies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

