Blepharitis & MGD: Overview - Lid Edge Lowdown
- Blepharitis: Chronic inflammation of eyelid margins.
- Anterior: Involves skin, eyelashes; often Staphylococcal or seborrhoeic.
- Posterior: Involves Meibomian gland orifices; linked to MGD.
- Meibomian Gland Dysfunction (MGD): Altered Meibomian gland secretion/obstruction, leading to tear film instability.
- Key cause of evaporative dry eye.
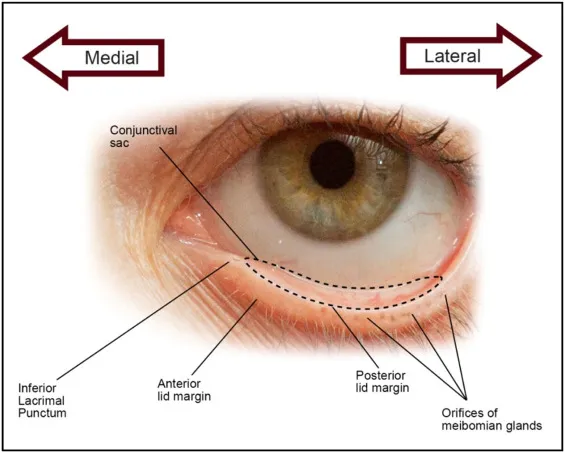
⭐ Posterior blepharitis is nearly synonymous with Meibomian Gland Dysfunction (MGD).
Anterior Blepharitis - Frontline Inflammation
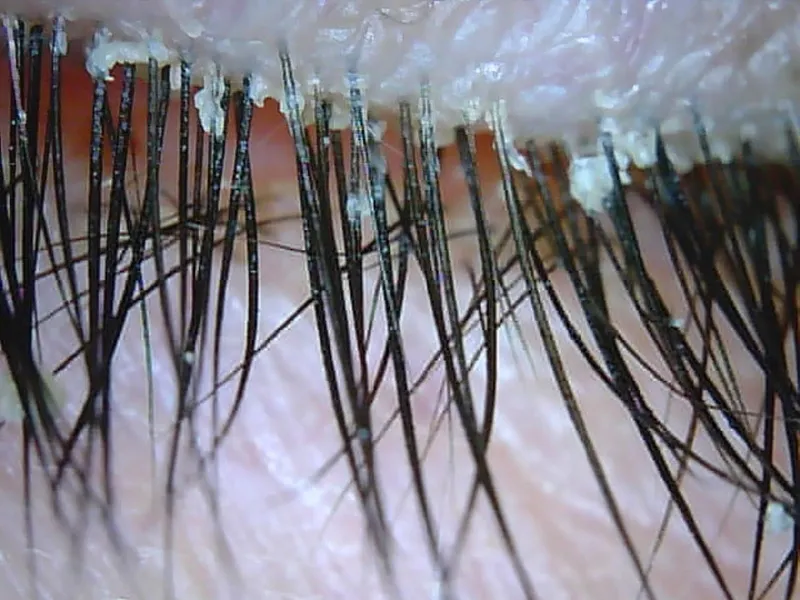
- Inflammation at eyelash base. Two main types:
- Staphylococcal:
- Hard scales, collarettes (fibrin crusts around lash base).
- Madarosis (lash loss), trichiasis (misdirected lashes), recurrent hordeolum.
- Often younger patients; more symptomatic.
- Seborrheic:
- Greasy, soft scales on lashes & lid margin; foamy tears.
- Less inflammation; associated with seborrheic dermatitis (scalp/face).
- Lashes often matted.
- Staphylococcal:
⭐ Collarettes are pathognomonic for Staphylococcal anterior blepharitis.
Posterior Blepharitis & MGD - Gland Gridlock
- Central: Meibomian Gland Dysfunction (MGD).
- Pathophysiology:
- Altered meibum: ↑viscosity, ↑melting point.
- Bacterial lipases → inflammatory free fatty acids.
- Results in: Gland obstruction, inspissation, dilation.
- Key Signs:
- Lid margin: Telangiectasias, hyperemia.
- Glands: Capped/pouting orifices; thick, "toothpaste" secretions; gland dropout.
- Tear film: ↓TBUT, frothy.
- Symptoms: Burning, foreign body sensation (FBS), blurred vision.
- Associated with: Acne rosacea.
⭐ MGD is the most common cause of evaporative dry eye disease.
Blepharitis: Complications - Lid's Angry Aftermath
- Lid Margin:
- Madarosis (loss of lashes)
- Trichiasis (misdirected lashes)
- Poliosis (white lashes)
- Tylosis (lid margin thickening)
- Lid ulceration, scarring
- Glandular:
- Hordeolum (stye) - acute
- Chalazion - chronic granuloma
- Conjunctival/Corneal:
- Chronic conjunctivitis
- Dry eye syndrome (secondary to MGD)
- Marginal keratitis (sterile infiltrates)
- Phlyctenular keratoconjunctivitis
- Corneal neovascularization, pannus

⭐ Recurrent chalazia, especially in the same location, warrant biopsy to rule out sebaceous gland carcinoma.
- Tear Film Instability: Common due to altered meibum quality/quantity in MGD.
- Contact Lens Intolerance
Blepharitis: Dx & Management - Clearing the View
- Dx (Clinical):
- Anterior: Lid margin redness, scurf, collarettes.
- Posterior (MGD): Inspissated glands, frothy tears, telangiectasia.
- Management:
- Core: Lid hygiene (warm compresses, scrubs).
- Medical: Topical antibiotics (e.g., azithromycin), oral tetracyclines (MGD), short-course steroids. Artificial tears.
⭐ Chronic blepharitis can lead to madarosis (loss of eyelashes).
High‑Yield Points - ⚡ Biggest Takeaways
- Blepharitis is chronic eyelid margin inflammation. Anterior involves lash base (Staphylococcal, Seborrheic); Posterior is Meibomian Gland Dysfunction (MGD).
- Staphylococcal blepharitis: Hard, collarette scales, madarosis, trichiasis. Seborrheic type: Greasy scales.
- MGD: Blocked meibomian glands cause inspissated secretions, frothy tears, lid margin telangiectasia; linked with rosacea.
- Cornerstone of all types: Lid hygiene (warm compresses, lid scrubs).
- Medical treatment: Topical antibiotics for anterior; oral doxycycline for MGD.
- Complications: Recurrent chalazia/hordeola, dry eye syndrome, marginal keratitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

