Visual Pathway & Lesions - Pathway Puzzles

- Visual information from the retina travels via the optic nerve, chiasm, tract, lateral geniculate nucleus (LGN), optic radiations, to the visual cortex.
- Lesion localization is key to diagnosing neurological disorders.
| Lesion Site | Visual Field Defect (VFD) |
|---|---|
| Optic Nerve | Ipsilateral blindness (anopia) |
| Optic Chiasm | Bitemporal hemianopia |
| Optic Tract | Contralateral homonymous hemianopia |
| Optic Radiations | Contralateral homonymous quadrantanopia/hemianopia |
| - Meyer's Loop (Temporal) | Contralateral superior quadrantanopia ('pie in the sky') |
| - Baum's Loop (Parietal) | Contralateral inferior quadrantanopia ('pie on the floor') |
| Visual Cortex | Contralateral homonymous hemianopia (macular sparing) |
⭐ Lesions of Meyer's loop (temporal lobe) cause contralateral superior quadrantanopia ('pie in the sky').
Types of VFDs - Shadow Shapes
- Central Scotoma: Central vision loss. Lesion: Macula, optic nerve.
- Centrocecal Scotoma: Macula to blind spot. Lesion: Optic nerve (toxic, nutritional).
- Arcuate Scotoma (Bjerrum's): Arches from blind spot (nerve fiber layer). Glaucoma.
- Nasal Step: Nasal defect, respects horizontal meridian. Glaucoma.
- Altitudinal Hemianopia: Superior/inferior half loss. Retinal vascular occlusion, AION.
- Homonymous Hemianopia: Same half lost, both eyes. Post-chiasmal. Congruity ↑ with posteriority.
- Bitemporal Hemianopia: Both temporal fields lost. Chiasmal lesion (e.g., pituitary adenoma).
- Quadrantanopia: Quarter field loss. 📌 PITS: Parietal-Inferior, Temporal-Superior ("Pie in the sky").
- Blind Spot Enlargement: Papilledema, glaucoma, drusen.
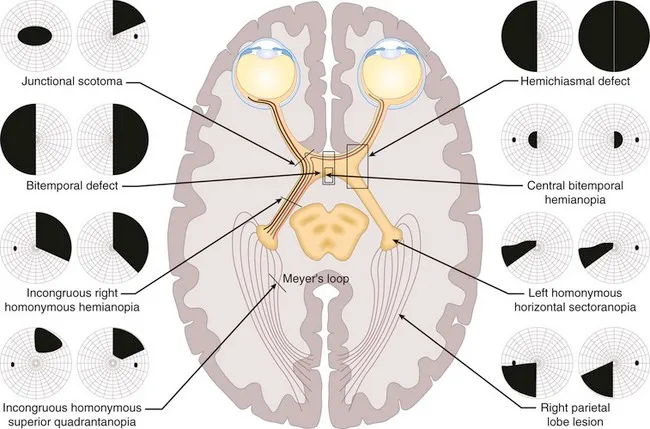
⭐ Respect for the vertical meridian indicates a lesion posterior to the chiasm, while respect for the horizontal meridian is more typical of retinal/glaucomatous lesions.
Etiologies of VFDs - Vision Villains
-
Pre-chiasmal (Optic Nerve): Glaucoma, optic neuritis (e.g., MS), NAION/GCA, compression.
- VFDs: Monocular scotomas, altitudinal/arcuate defects.
-
Chiasmal & Retro-chiasmal Pathologies & VFDs:
Pathology Typical VFD Pituitary Adenoma Bitemporal Hemianopia Craniopharyngioma Bitemporal Hemianopia (often inferiorly) Optic Tract Lesion Contralateral Incongruous Homonymous Hemianopia Meyer's Loop Lesion Contralateral Superior Quadrantanopia ("Pie in sky") Parietal Lobe Lesion Contralateral Inferior Quadrantanopia ("Pie on floor") Occipital Lobe Lesion (PCA Stroke) Contralateral Homonymous Hemianopia (macula sparing) ⭐ Pituitary adenomas are the most common cause of bitemporal hemianopia.

Perimetry Basics - Field Test Tactics
- Types:
- Confrontation: Gross screening.
- Kinetic (e.g., Goldmann): Moving stimulus, maps isopters.
- Static (e.g., Humphrey): Stationary stimulus, threshold testing.
- Normal Field Extent: Superior 60°, Inferior 75°, Nasal 60°, Temporal 100°.
- Interpretation (Automated):
- Reliability Indices: Fixation losses, false +ve/-ve.
- Pattern Deviation: Highlights localized loss.

⭐ A dense central scotoma with peripheral sparing (tunnel vision) can be seen in advanced glaucoma, retinitis pigmentosa, or hysteria.
High‑Yield Points - ⚡ Biggest Takeaways
- Optic chiasm lesions typically cause bitemporal hemianopia.
- Optic tract lesions result in contralateral homonymous hemianopia.
- Meyer's loop lesions (temporal lobe) cause contralateral "pie in the sky" (superior quadrantanopia).
- Parietal lobe lesions (affecting optic radiations) cause contralateral "pie on the floor" (inferior quadrantanopia).
- Occipital cortex lesions cause contralateral homonymous hemianopia, often with macular sparing.
- Junctional scotoma (anterior chiasmal) presents with ipsilateral central vision loss and contralateral superotemporal defect.
- Respect for the vertical midline is characteristic of retrochiasmal lesions.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

