POAG Defined - The Sneaky Thief
- A chronic, progressive optic neuropathy, often asymptomatic in early stages.
- Key diagnostic features:
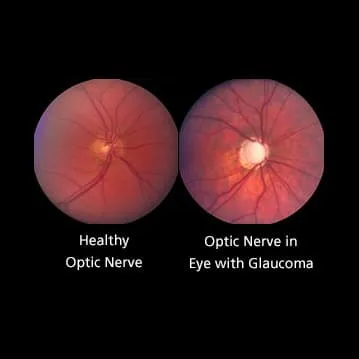
- Characteristic optic nerve head (ONH) cupping (e.g., ↑ cup-to-disc ratio).
- Specific patterns of visual field (VF) loss.
- Open, normal-appearing anterior chamber angle (ACA) on gonioscopy.
- Often linked to ↑ Intraocular Pressure (IOP > 21 mmHg), though Normal Tension Glaucoma exists.
- Epidemiology:
- Most common type of glaucoma worldwide.
- Prevalence significantly ↑ with age (typically affecting those > 40 years).
- Major risk factors: positive family history, African descent, myopia, diabetes mellitus.
- Its insidious, asymptomatic nature earns it the name "sneaky thief of sight".
⭐ Elevated IOP is the most significant modifiable risk factor for the development and progression of POAG.
Risk Factors & Pathophysiology - Pressure Cooker Eye
- Risk Factors: 📌 (Mnemonic: Age, Family Hx, Race, IOP, CCT, Associated diseases, Nearsightedness)
- ↑IOP (most significant modifiable)
- Age > 40 yrs
- Family Hx (1st degree)
- Race (African, Hispanic)
- Thin CCT (< 555 microns)
- High Myopia
- DM, HTN
- Pathophysiology:
- ↓Aqueous outflow via TM → ↑IOP.
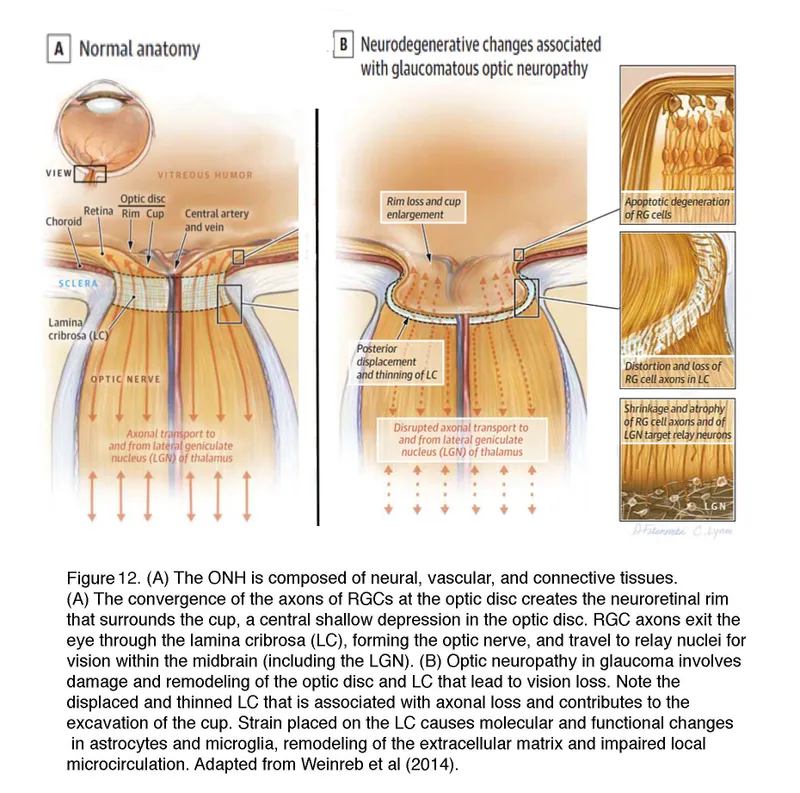
- ONH Damage:
- Mechanical: Lamina distortion.
- Vascular: Ischemia, ↓axonal flow.
⭐ A thin Central Corneal Thickness (CCT < 555 microns) is an independent risk factor for progression from ocular hypertension to POAG.
Clinical Picture - Silent Signs
- Largely asymptomatic initially ("silent thief of sight"); insidious onset.
- Late: Gradual, painless peripheral vision loss (classic tunnel vision).
- Signs:
- ↑IOP (typically > 21 mmHg, but variable).
- Open angle on Gonioscopy (Shaffer grade III-IV).
- Optic Disc Damage (Glaucomatous Optic Neuropathy):
- ↑CDR (> 0.5 or asymmetry > 0.2).
- Neuroretinal rim notching (often inferotemporal/superotemporal).
- RNFL defects (e.g., slit or wedge-shaped).
⭐ The ISNT rule (normal rim: Inferior > Superior > Nasal > Temporal) is often violated in glaucomatous optic neuropathy. oka
Diagnostic Toolkit - Unmasking POAG
- Tonometry: Measures Intraocular Pressure (IOP); Goldmann applanation tonometry is gold standard. Normal IOP: 10-21 mmHg.
- Gonioscopy: Visualizes iridocorneal angle; differentiates open vs. closed angle.
- Ophthalmoscopy/Stereo-biomicroscopy: Optic disc assessment (cupping, CDR >0.5, notching, NRR thinning).
- Perimetry (Humphrey Visual Field - HVF): Detects functional loss.
- Early: Nasal step, paracentral scotoma.
- Late: Arcuate scotoma (Bjerrum's), temporal wedge, tunnel vision.
- Optical Coherence Tomography (OCT): Quantifies structural damage.
- Retinal Nerve Fiber Layer (RNFL) thinning.
- Ganglion Cell Complex (GCC) analysis.
⭐ Vertical elongation of the cup (vertical C:D ratio > horizontal) is an early sign of glaucomatous optic neuropathy, often preceding RNFL changes detectable by OCT or visual field defects.
Management Matrix - Lowering Pressure
Goal: Achieve target IOP (↓ 20-30% from baseline or individualized).
- Medical Therapy (Stepwise):
- 1st Line: Prostaglandin analogs (PGAs) (e.g., Latanoprost) - ↑ Uveoscleral outflow.
- Adjunctive: Beta-blockers (e.g., Timolol), Carbonic Anhydrase Inhibitors (CAIs) (e.g., Dorzolamide) - ↓ aqueous production; α2-Agonists (e.g., Brimonidine) - dual mechanism (↓ aqueous production, ↑ uveoscleral outflow).
- Laser Therapy:
- Selective Laser Trabeculoplasty (SLT) or Argon Laser Trabeculoplasty (ALT) - ↑ Trabecular outflow.
- Surgical Therapy (if medical/laser fails or advanced disease):
- Trabeculectomy (gold standard).
- Glaucoma Drainage Devices (GDDs).
- Minimally Invasive Glaucoma Surgery (MIGS).
⭐ Latanoprost (a PGA) is often the first-line choice due to potent IOP lowering, once-daily dosing, and a favorable systemic side-effect profile.
High‑Yield Points - ⚡ Biggest Takeaways
- POAG: Most common glaucoma; painless, progressive optic neuropathy.
- Key signs: ↑ cup-disc ratio, characteristic visual field defects (e.g., arcuate scotoma).
- IOP is a major risk factor; gonioscopy confirms open angle.
- Prostaglandin analogues are often first-line medical treatment to ↓ IOP.
- Early diagnosis and treatment are crucial to prevent irreversible vision loss.
- Often asymptomatic until advanced stages, highlighting screening importance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

