Endometriosis Pain: Pathophysiology - Rogue Tissue Riot
- Ectopic Tissue: Endometrial glands & stroma outside uterus, estrogen-sensitive.
- Inflammatory Milieu: Core of pain.
- Cyclical bleeding from implants → sterile inflammation.
- ↑ Prostaglandins (e.g., $PGE_2$, $PGF_{2\alpha}$), cytokines (e.g., TNF-α, IL-1β, IL-6), chemokines.
- Activated immune cells (macrophages, mast cells).
- Neurogenic Inflammation & Angiogenesis:
- ↑ Nerve Growth Factor (NGF) → sensory nerve fiber sprouting (hyperinnervation).
- New vessel growth sustains lesions.
- Pain Sensitization:
- Peripheral: Nociceptors become hypersensitive.
- Central: CNS amplifies pain signals (allodynia, hyperalgesia).
- Structural Distortion:
- Adhesions, fibrosis, scarring.
- Nerve compression/infiltration by lesions.
- Endometriomas (ovarian "chocolate cysts").
⭐ Increased Nerve Growth Factor (NGF) in peritoneal fluid is strongly linked to endometriosis-associated pain severity and lesion hyperinnervation.
Endometriosis Pain: Diagnosis - Unmasking Misery
- Clinical Presentation:
- Cyclical pelvic pain (dysmenorrhea), often progressive.
- Deep dyspareunia.
- Chronic pelvic pain (CPP > 6 months).
- Dyschezia, dysuria (if bowel/bladder involved).
- Subfertility or infertility.
- Key Examination Findings:
- Pelvic tenderness (non-specific).
- Uterosacral ligament nodularity, thickening, or tenderness.
- Adnexal mass (endometrioma).
- Fixed, retroverted uterus.
- Investigations:
- Transvaginal Sonography (TVS):
- First-line imaging modality.
- Identifies endometriomas (homogenous, low-level echogenicity - "ground glass" appearance).
- May suggest Deep Infiltrating Endometriosis (DIE) or adenomyosis.
- MRI:
- Useful for complex cases, extensive DIE, or when TVS is inconclusive.
- Aids in pre-operative mapping.
- Laparoscopy:
- Gold standard for definitive diagnosis.
- Allows direct visualization of lesions (e.g., powder-burn, clear, red, blue-black, white opacifications, adhesions, endometriomas).
- Enables biopsy for histological confirmation (presence of endometrial glands and stroma).
- Transvaginal Sonography (TVS):
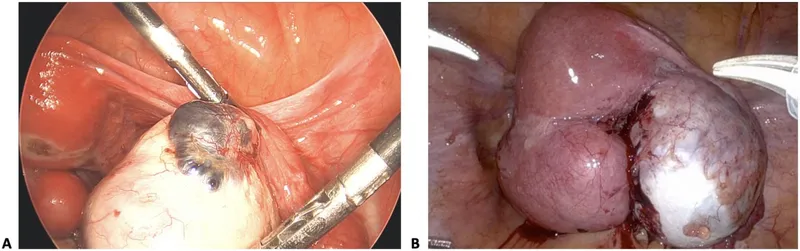
⭐ Laparoscopy with histological confirmation is the gold standard for diagnosing endometriosis, allowing for simultaneous diagnosis and potential treatment.
Endometriosis Pain: Management - Calming the Chaos
Goal: Alleviate pain, improve QoL, preserve fertility if desired. Stepwise, individualized management.
- Pharmacological Therapy:
- NSAIDs: Mild pain (e.g., Mefenamic acid, Ibuprofen).
- Combined Oral Contraceptives (COCs): Continuous regimen for amenorrhea, ovulation suppression.
- Progestins:
- Dienogest (2 mg/day).
- Norethisterone acetate (5-15 mg/day).
- MPA (depot/oral).
- GnRH Agonists: (Leuprolide, Goserelin)
- Pseudomenopause; use "add-back" (E+P) to ↓ side effects (bone loss, vasomotor). Max 6-12 months.
- GnRH Antagonists: (Elagolix) Oral, dose-dependent estradiol suppression.
- Danazol: Androgenic side effects limit use.
- Surgical Management:
- Conservative: Laparoscopic excision/ablation of implants, adhesiolysis. For Dx, pain relief, fertility enhancement.
- Definitive: TAH+BSO for severe, refractory pain (childbearing complete).
- Adjunctive Therapies: Physiotherapy, TENS, acupuncture, lifestyle modifications.
⭐ Dienogest 2 mg/day is an effective oral progestin for endometriosis-associated pain, often chosen for its balance of efficacy and tolerability, avoiding severe hypoestrogenic effects seen with GnRH agonists alone.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic pelvic pain, dysmenorrhea, and dyspareunia are classic symptoms.
- Retrograde menstruation is the most accepted etiological theory.
- Ovaries are the most common site, often with endometriomas ('chocolate cysts').
- Laparoscopy with biopsy is the gold standard for diagnosis.
- Look for powder-burn lesions, adhesions, and blue-black ('mulberry') spots.
- Management: NSAIDs, hormonal therapy (OCPs, GnRH agonists), and surgery.
- Strong association with infertility and subfertility.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

