VBAC Basics - Green Lights & Red Flags
VBAC: Vaginal Birth After Cesarean. TOLAC: Trial Of Labor After Cesarean.
- Suitable Candidates (Green Lights):
- One prior Low Transverse Cesarean Section (LTCS).
- Clinically adequate pelvis; no history of Cephalopelvic Disproportion (CPD).
- No other uterine scars (e.g., from myomectomy) or previous uterine rupture.
- Immediate access to emergency Cesarean delivery & anesthesia.
- Recommended interval from previous CS: >18 months.
- Singleton pregnancy, cephalic presentation.
- Informed consent obtained.

| Contraindication Type | Examples |
|---|---|
| Absolute | Previous classical/T-shaped incision, prior uterine rupture, extensive transfundal uterine surgery |
| Relative | ≥2 previous LTCS, unknown uterine scar type, twin gestation, breech presentation, suspected macrosomia (>4kg) |
VBAC Risks - Rupture Roulette
Uterine rupture: most critical risk.
- Incidence: LTCS 0.5-0.9%; Classical/Vertical 4-9%.
- Prior rupture: Absolute contraindication.
Risk Factors for Uterine Rupture:
| Factor | Risk Impact |
|---|---|
| Prior classical scar | ↑↑↑ |
| <18-24 months since CS | ↑ |
| Induction (Prostaglandins) | ↑ |
| Macrosomia | ↑ |
| Multiple prior CS (≥2) | ↑ |
- Fetal bradycardia (most common)
- Sudden, severe abdominal pain/scar tenderness
- Loss of fetal station
- Vaginal bleeding (variable)
- Maternal tachycardia/hypotension
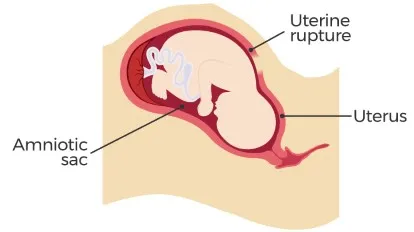
⭐ Fetal bradycardia is the most common and often earliest sign of uterine rupture during TOLAC.
Other Risks: Maternal (hysterectomy, hemorrhage); Neonatal (HIE, death).
Management: Suspected Rupture
TOLAC Tactics - Labor Game Plan
- Intrapartum Care:
- Delivery in a facility equipped for emergency Cesarean Section (CS).
- Continuous Electronic Fetal Monitoring (EFM) mandatory.
- Induction & Augmentation:
- Mechanical methods (e.g., Foley catheter) preferred for cervical ripening.
- Oxytocin: Cautious, low-dose protocol (e.g., start 0.5-2 mU/min, titrate slowly, max 20 mU/min).
- Avoid prostaglandins.
⭐ Prostaglandin E1 (Misoprostol) is generally contraindicated for cervical ripening or induction in TOLAC due to increased risk of uterine rupture.
- Pain Relief: Epidural analgesia is not contraindicated; can be used.
- Abandon TOLAC & Proceed to CS if:
- Arrest of labor (dilation/descent).
- Non-reassuring fetal status.
- Signs of uterine rupture (e.g., fetal bradycardia, maternal tachycardia/hypotension, scar tenderness, loss of station).
VBAC Success - Victory Predictors
Overall VBAC success rate: 60-80%.
| Favorable Factors (↑ Success) | Unfavorable Factors (↓ Success) |
|---|---|
| * Prior vaginal birth (especially prior VBAC) | * Recurrent indication for previous CS (e.g., CPD) |
| * Spontaneous labor | * Need for induction/augmentation of labor |
| * Non-recurrent indication for previous CS | * Increased maternal age (>40 years) |
| * Favorable cervix (e.g., Bishop score >6) | * Obesity (BMI >30) |
| * Inter-delivery interval >18 months | * Macrosomia (>4-4.5 kg) |
| * Single layer uterine closure (controversial) | * Gestational age >41 weeks |
High-Yield Points - ⚡ Biggest Takeaways
- One prior low transverse CS (LTCS) is the ideal prerequisite for VBAC.
- Risk of uterine rupture with one LTCS is ~0.5-0.9%.
- Absolute contraindications include classical/T-shaped incision or prior uterine rupture.
- Continuous electronic fetal monitoring is mandatory during TOLAC.
- Prostaglandins for induction are contraindicated; Oxytocin may be used cautiously.
- Fetal bradycardia is the most common and earliest sign of uterine rupture.
- Successful TOLAC rates are 60-80%.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

