Pregnancy's Surgical Stage - Bump's Big Day Prep
- Physiological Adaptations for Surgery:
- Cardio: ↑ Cardiac Output (CO), ↓ Systemic Vascular Resistance (SVR).
- Respiratory: ↓ Functional Residual Capacity (FRC), ↑ O2 consumption.
- GI: ↓ motility, ↓ Lower Esophageal Sphincter (LES) tone (↑ reflux/aspiration risk).
- Hematologic: Hypercoagulable state, physiological anemia.
- Surgical/Anesthetic Impact:
- Mother: Aspiration, Deep Vein Thrombosis (DVT).
- Fetus: Hypoxia, acidosis, preterm labor; Intrauterine Growth Restriction (IUGR) if prolonged/severe stress.
- Teratogenic Risks:
- Critical period (drugs/radiation): 3-8 weeks post-conception.
- Radiation exposure: <5 rads generally considered safe.
⭐ Progesterone-induced ↓GI motility & ↓LES tone significantly ↑ aspiration risk during anesthesia in pregnant patients.
The Pre-Op Puzzle - Timing Triumphs Tests
- Optimal Timing: Second Trimester (14-26 wks)
- Why: Organogenesis complete, ↓ spontaneous abortion risk, ↓ preterm labor risk. Uterus size manageable.
- Indications & Urgency:
- Urgent (e.g., appendicitis, trauma): Surgery ASAP.
- Non-urgent: Postpone postpartum if possible; if not, target 2nd trimester.
- Maternal Pre-Op Assessment:
- Standard surgical workup.
- Obstetric considerations: Gestational Age (GA), comorbidities (e.g., GDM, PIH), baseline Fetal Heart Rate (FHR).
- Fetal Pre-Op Assessment:
- Ultrasound: Confirm viability, GA, anatomy, placental location.
- If viable fetus & GA > 24 wks: Consider Non-Stress Test (NST) / Biophysical Profile (BPP).
- Informed Consent:
- Discuss maternal & fetal risks (anesthesia, surgery).
- Alternatives to surgery.
- Risk of preterm labor/delivery.
- Potential need for obstetric interventions (e.g., tocolysis, steroids, C-section).
⭐ > The second trimester is generally the safest period for non-urgent surgery in pregnant women.
Anesthesia & Intra-Op - Safe Sleep, Scalpel Smart
- Goals: Maternal safety, fetal well-being (uterine perfusion, avoid hypoxia/hypotension/acidosis), uterine quiescence.
- Choice: Regional (spinal/epidural) > GA (↓ fetal drug exposure & aspiration risk).
- GA for: Emergencies, regional C/I, complex/long surgery.
- Drugs:
- Avoid NSAIDs 3rd trimester (premature ductal closure).
- Benzos: Cleft risk (1st tri), neonatal effects.
- Opioids: Neonatal respiratory depression.
- Prefer: Short half-life, high protein binding.
- Positioning: 📌 LUD (Left Uterine Displacement) after ~18-20 wks (prevents aortocaval compression).
⭐ Aortocaval compression by gravid uterus reduces CO by up to 30% supine.
- Fetal Monitoring: Intermittent FHR auscultation or continuous EFM if viable; document FHR pre/post.
- Laparoscopy: Precautions:
- Insufflation <12-15 mmHg.
- Veress/Hasson; supraumbilical/Palmer's point (1st port).
- Ports under vision.
Post-Op & Common Culprits - Healing Duo, Usual Suspects
- Post-operative Care:
- Continuous Fetal monitoring (FHR, uterine activity) 4-6 hrs post-op, maternal vitals.
- Prophylactic Tocolysis:
- Not routine. Consider if high risk (beta-mimetics, CCBs, MgSO4).
- ⚠️ Avoid indomethacin in 3rd trimester.
- DVT Prophylaxis:
- Early ambulation, SCDs.
- LMWH if high risk (continue 6 wks postpartum if indicated).
- Pain Management:
- Paracetamol first-line. Opioids (cautious, short duration).
- ⚠️ Avoid NSAIDs late pregnancy.
- Common Non-Obstetric Surgical Conditions:
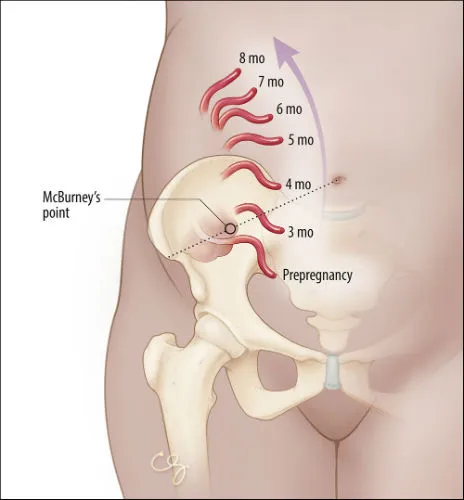
- Appendicitis: Most common. Atypical presentation (appendix displaced ↑ & laterally). Early surgery.
- Cholecystitis: Conservative vs surgery. Lap chole feasible (ideal 2nd trimester).
- Ovarian Torsion: High incidence. Surgical emergency. Contralateral oophoropexy if indicated.
- Trauma: ABCDE. Kleihauer-Betke test (Rh-negative) for RhoGAM.
- Appendicitis: Most common. Atypical presentation (appendix displaced ↑ & laterally). Early surgery.
⭐ Appendicitis is the most common non-obstetric surgical emergency during pregnancy, with diagnosis often delayed due to atypical symptoms.
High‑Yield Points - ⚡ Biggest Takeaways
- Optimal timing for non-urgent surgery: second trimester (14-28 weeks).
- Appendicitis: most common non-obstetric surgical emergency during pregnancy.
- Laparoscopy: generally safe; use open (Hasson) technique for initial access.
- Prophylactic tocolytics: generally not recommended.
- Maternal positioning: left lateral tilt (after 20 weeks) to avoid aortocaval compression.
- Fetal monitoring: indicated intra- and post-operatively for viable gestations.
- VTE prophylaxis: crucial due to pregnancy-induced hypercoagulable state.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

