Menopause Unveiled - Hormone Hibernation
- Definition (WHO): Permanent cessation of menstruation from loss of ovarian follicular activity; diagnosed after 12 months amenorrhea.
- Average Age: Indian: ~46-48 yrs (Global: ~51).
- Key Hormonal Shifts:
- ↑FSH (>25-30 IU/L): Key diagnostic marker.
- ↓Estradiol: Causes symptoms.
- ↓Inhibin B: Early marker of ovarian decline.
- ↓AMH: Reflects ovarian reserve.
- Stages:
- Perimenopause: Transition; irregular cycles, hormonal fluctuations, early symptoms.
- Menopause: 12 consecutive months of amenorrhea.
- Postmenopause: Years after menopause.
- Premature Ovarian Insufficiency (POI): Menopause before age 40.
⭐ Most reliable endocrine marker for ovarian reserve is AMH.
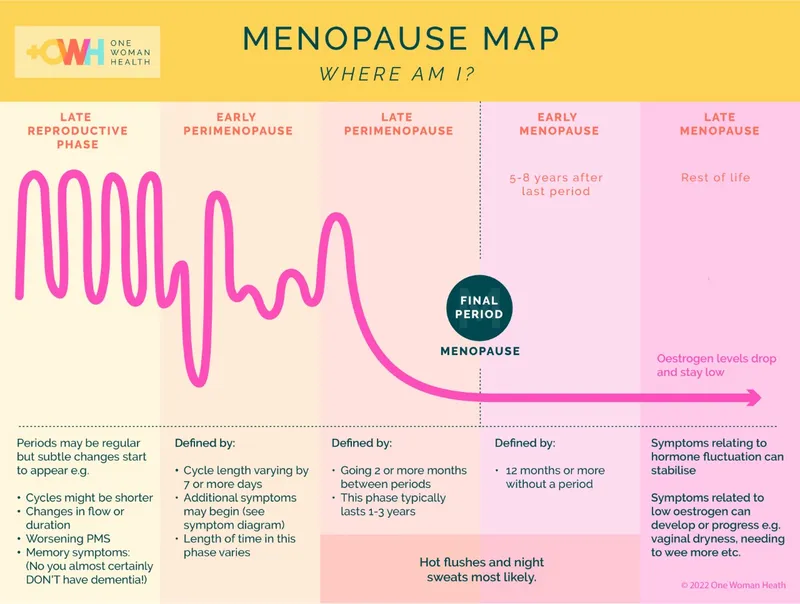
Symptom Spectrum - The Heat Is On
Menopause, driven by declining estrogen, presents symptoms affecting daily function and long-term health.
-
Hallmark Symptom Groups:
Feature Vasomotor Symptoms (VMS) Genitourinary Syndrome of Menopause (GSM) Core Issue Hypothalamic thermoregulatory instability. Estrogen deficiency leading to atrophic changes in urogenital tissues. Key Manifestations Sudden hot flashes (intense warmth, sweating, flushing); nocturnal night sweats disrupting sleep. 📌 VUS: Vaginal (atrophy, dryness, burning, dyspareunia); Urinary (urgency, frequency, dysuria, recurrent UTIs); Sexual discomfort. 
-
Other Significant Symptoms:
- Sleep Disturbances: Difficulty sleeping (insomnia), poor sleep quality, often VMS-linked.
- Mood & Cognitive Changes: Increased anxiety, depression, irritability; 'brain fog', concentration/memory lapses.
- Musculoskeletal Pain: Common: arthralgia (joint pain) and myalgia (muscle pain).
-
Critical Long-Term Health Risks:
- Osteoporosis:
- Pathophysiology: ↓Estrogen accelerates bone resorption (↑osteoclasts, ↓osteoblasts), reducing bone density.
- Risk Factors: Early/premature menopause, smoking, low BMI, inadequate $Ca^{2+}$/Vit D, family history.
- Screening: DEXA scan for BMD; T-score ≤ -2.5 indicates osteoporosis.
- Cardiovascular Disease (CVD) Risk:
- Factors: Adverse lipid profile (↑LDL, ↓HDL, ↑TG), endothelial dysfunction, increased visceral fat.
- Osteoporosis:
⭐ Hot flashes are the most common and bothersome symptom, often prompting medical evaluation.
Management Toolkit - Cooling Strategies
- Diagnosis: Clinical presentation; consider FSH >30 mIU/mL if diagnosis uncertain.
- Lifestyle First-Line: Layer clothes, cool environment, avoid triggers (spicy food, caffeine), stress reduction, exercise.
Menopausal Hormone Therapy (MHT) for Vasomotor Symptoms (VMS):
- Indications: Moderate-severe VMS, Genitourinary Syndrome of Menopause (GSM), Osteoporosis prevention (especially if <60 yrs or within 10 yrs of menopause onset).
- Contraindications: 📌 Current/past breast cancer, estrogen-sensitive cancers (e.g., endometrial cancer); undiagnosed abnormal genital bleeding; history of Venous Thromboembolism (VTE); active liver disease; established Coronary Artery Disease (CAD) or stroke.
- Regimens & Routes:
- Estrogen Therapy (ET): For women post-hysterectomy. (Oral, transdermal).
- Estrogen + Progestogen Therapy (EPT): For women with an intact uterus (endometrial protection). (Oral, transdermal).
- ⭐ > For women with an intact uterus, estrogen therapy (ET) must always be combined with a progestogen (EPT) to prevent endometrial hyperplasia/cancer.
- Key Risks: VTE, stroke, slight ↑ breast cancer risk with long-term EPT.
- Key Benefits: Highly effective for VMS, improves GSM, prevents osteoporosis.
 risks versus benefits for VMS, GSM, and bone health)
risks versus benefits for VMS, GSM, and bone health)
Non-Hormonal Pharmacotherapy for VMS:
- SSRIs: Paroxetine 7.5mg/day (FDA-approved for VMS).
- SNRIs: Venlafaxine, Desvenlafaxine (off-label).
- Gabapentin.
- Clonidine.
Flowchart: VMS Management Approach
High‑Yield Points - ⚡ Biggest Takeaways
- Menopause: Defined as 12 consecutive months of amenorrhea; average age in India is 46-51 years.
- Vasomotor symptoms (hot flushes, night sweats) are hallmark; Hormone Replacement Therapy (HRT) is most effective. SSRIs/SNRIs are non-hormonal alternatives.
- Genitourinary Syndrome of Menopause (GSM) causes vaginal dryness and dyspareunia; treat with topical estrogen or moisturizers.
- Osteoporosis risk significantly ↑ post-menopause; screen with DEXA scan, manage with bisphosphonates, calcium, and Vitamin D.
- HRT is indicated for symptomatic women <60 years or within 10 years of menopause, after excluding contraindications (e.g., breast cancer Hx, VTE, undiagnosed vaginal bleeding).
- Premature Ovarian Insufficiency (POI): Menopause before age 40; requires HRT until the average age of natural menopause unless contraindicated.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

