Indications & Overview - Why & What We Test
- Purpose: Detect fetal conditions; enable informed choice & management.
- Indications (Why Test):
- AMA (>35 yrs).
- Previous child/family hx: genetic disorder/chromosome anomaly.
- Parental carrier: chromosomal abnormality.
- Abnormal screening: FTS, NIPT, Quad.
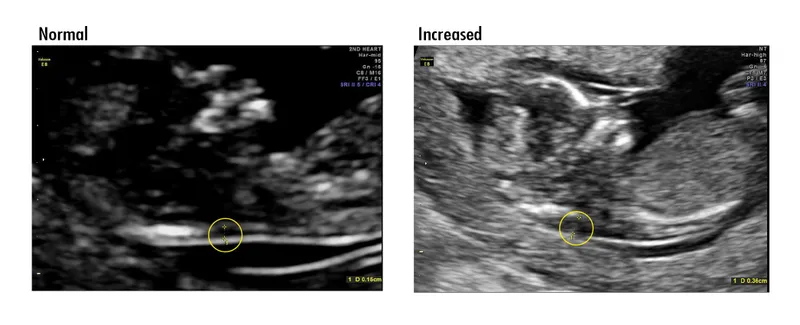
- Ultrasound markers: ↑NT, structural defects.
- Scope (What We Test):
- Chromosomal: Trisomies (21, 18, 13).
- Single gene: Thalassemia, CF.
- Structural: NTDs, cardiac.
- Genetic Counseling: Key for risk/benefit discussion, informed decisions.
⭐ Nuchal Translucency (NT) >3.5mm is a significant marker for aneuploidy (e.g., Trisomy 21) and fetal cardiac anomalies.
Screening Tests - Early Clues Hunt
- Goal: Identify ↑ risk for aneuploidy (e.g., Down syndrome) & NTDs. Non-diagnostic.
- First Trimester Combined (FTCS): 11 - 13$^{+6}$ wks
- Serum: ↓ PAPP-A, ↑ free β-hCG (T21)
- USG: ↑ Nuchal Translucency (NT)
- DR T21: ~90%
- Second Trimester Quad Test: 15 - 22$^{+6}$ wks (opt. 16-18w)
- Serum (T21): ↓ AFP, ↓ uE3, ↑ hCG, ↑ Inhibin A
- 📌 T21: "HI" - hCG & Inhibin A are High.
- ↑ AFP: NTDs.
- DR T21: ~80%
- Serum (T21): ↓ AFP, ↓ uE3, ↑ hCG, ↑ Inhibin A
- NIPT (cell-free fetal DNA): From 10 wks
- Highest DR for common trisomies (T21 >99%).
⭐ NIPT (cffDNA): highest screening DR (>99% T21); positive results need diagnostic confirmation.
- USG Markers:
- 1st Tri: NT, nasal bone.
- 2nd Tri: Soft markers (e.g., EIF).
 A_IMAGE_PLACEHOLDER
A_IMAGE_PLACEHOLDER
Invasive Diagnostics - Confirming Suspicions
Confirmatory tests after abnormal screening or high-risk history. Pre-test counseling is vital. Rapid results (e.g., FISH for common aneuploidies) often available.
- Chorionic Villus Sampling (CVS)
- Timing: 10-13 weeks gestation.
- Method: Samples placental villi (transcervical/transabdominal).
- Detects: Chromosomal abnormalities, genetic disorders (e.g., thalassemia). Does NOT detect NTDs.
- Risk: Miscarriage ~0.5-1%; limb reduction defects if <10 weeks.
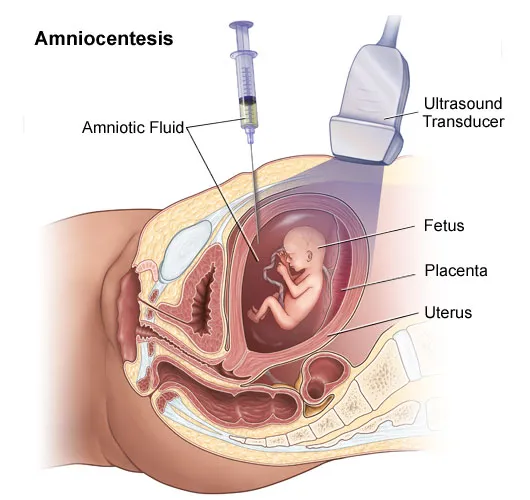
- Amniocentesis
- Timing: Typically 15-20 weeks; can be done later.
- Method: Samples amniotic fluid (fetal cells, biochemicals).
- Detects: Chromosomal abnormalities, NTDs (AFP), lung maturity (L/S ratio), Rh isoimmunization.
⭐ Amniotic fluid acetylcholinesterase (AChE) is more specific for open NTDs than AFP.
- Risk: Miscarriage ~0.1-0.3%.
- Cordocentesis (Percutaneous Umbilical Blood Sampling - PUBS)
- Timing: Usually >18 weeks.
- Method: Fetal blood from umbilical cord.
- Uses: Rapid karyotyping, fetal anemia, infection, thrombocytopenia, fetal therapy.
- Risk: Highest; ~1-2% miscarriage.
Genetic Counseling & Key Syndromes - Guidance & Genes
- Genetic Counseling:
- Non-directive communication for informed choices, risk assessment, support.
- Indications: Advanced Maternal Age (AMA >35y), +ve family Hx, abnormal screen/USG, teratogen, consanguinity.
- Key Aneuploidies (Chromosomal Abnormalities): 📌 Trisomy Ages: Down (21), Edwards (18), Patau (13).
- Down (T21): Most common. ID, epicanthal folds, single palmar crease, CHD.
- Edwards (T18): Severe. Clenched hands, rocker-bottom feet, micrognathia, CHD. Poor prognosis.
- Patau (T13): Severe. Midline defects (holoprosencephaly, clefts), polydactyly, CHD. Poor prognosis.
- Turner (45,X0): Female. Short stature, webbed neck, ovarian dysgenesis, coarctation.
- Klinefelter (47,XXY): Male. Tall, gynecomastia, hypogonadism, infertility.
⭐ Non-Invasive Prenatal Testing (NIPT) using cell-free fetal DNA (cffDNA) is a highly sensitive screening test for common aneuploidies.
High‑Yield Points - ⚡ Biggest Takeaways
- First-trimester screening (Dual test, NT scan): 11-13+6 weeks for aneuploidy risk.
- Second-trimester screening (Quadruple test): 15-20 weeks, detects Down syndrome, NTDs.
- CVS: 10-13 weeks for early genetic diagnosis; slight risk of fetal loss.
- Amniocentesis: 15-20 weeks for genetic diagnosis; safer than CVS.
- NIPT (cfDNA): From 10 weeks; high sensitivity for common trisomies.
- Karyotyping: Gold standard for definitive diagnosis of chromosomal abnormalities.
- Autosomal recessive disorders: 25% recurrence risk with each pregnancy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

