Diabetes in Pregnancy - Sweet Beginnings
- Encompasses Pre-gestational Diabetes (PGDM) & Gestational Diabetes Mellitus (GDM).
- GDM: Glucose intolerance first detected during pregnancy.
- Screening (India - DIPSI): Single 75g OGTT; 2-hr plasma glucose $\ge$ 140 mg/dL.
- Diagnosis (WHO criteria): 75g OGTT; any one: Fasting $\ge$ 92, 1-hr $\ge$ 180, 2-hr $\ge$ 153 mg/dL.
- PGDM: Pre-existing Type 1 or Type 2 DM; higher congenital anomaly risk.
- Key risks: Macrosomia, neonatal hypoglycemia, preeclampsia, future maternal T2DM.
⭐ GDM typically manifests in the 2nd/3rd trimester due to placental hormones (e.g., hPL) inducing insulin resistance.
Diabetes in Pregnancy - Insulin's Uphill Battle
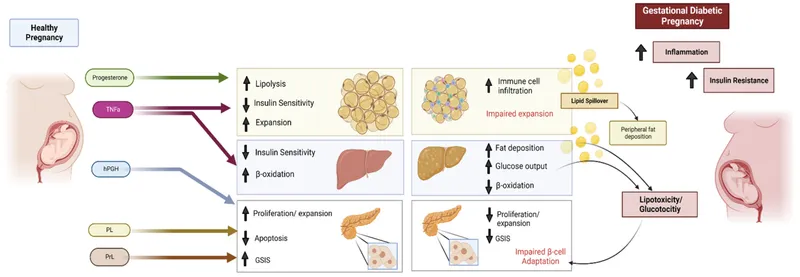
- Pregnancy: A diabetogenic state due to placental hormones.
- Key antagonists: Human Placental Lactogen (hPL), progesterone, estrogen, cortisol.
- These ↑, causing progressive ↑ insulin resistance, peaking in late pregnancy.
- Pancreatic β-cells ↑ insulin production to compensate (hyperinsulinemia).
- GDM: Develops if β-cells fail to overcome this resistance.
- Pre-existing DM: Control often worsens.
- Pre-existing DM: Control often worsens.
⭐ Human Placental Lactogen (hPL) is a major contributor to insulin resistance during pregnancy.
Diabetes in Pregnancy - Catch & Confirm
- Universal GDM screening is crucial.
- Indian Guidelines:
- DIPSI (Single Step): Non-fasting 75g Oral Glucose Tolerance Test (OGTT).
- 2-hour Plasma Glucose (PG) ≥ 140 mg/dL → GDM.
- IADPSG/WHO (One Step): Fasting 75g OGTT.
- Any one value met/exceeded: Fasting PG (FPG) ≥ 92 mg/dL, 1-hour PG ≥ 180 mg/dL, 2-hour PG ≥ 153 mg/dL → GDM.
- DIPSI (Single Step): Non-fasting 75g Oral Glucose Tolerance Test (OGTT).
- Overt Diabetes (Pre-existing): FPG ≥ 126 mg/dL, HbA1c ≥ 6.5%, or Random PG (RPG) ≥ 200 mg/dL with symptoms.
⭐ GDM diagnosis by IADPSG criteria is associated with a significantly increased risk of Large for Gestational Age (LGA) infants compared to older criteria.
Diabetes in Pregnancy - Mom & Baby Woes
Maternal Complications:
- Pre-eclampsia, eclampsia: ↑ risk
- Infections: UTI, candidiasis common
- Polyhydramnios: Due to fetal polyuria
- Operative delivery: ↑ C-section rates
- Diabetic Ketoacidosis (DKA): Life-threatening
- Progression of microvascular disease (retinopathy, nephropathy)
Fetal & Neonatal Complications:
- Macrosomia (>4-4.5 kg)
- Leads to birth trauma (e.g., shoulder dystocia)
- Neonatal Metabolic Issues:
- Hypoglycemia (due to fetal hyperinsulinemia)
- Hypocalcemia, Hypomagnesemia
- Respiratory Distress Syndrome (RDS): Delayed lung maturity
- Hyperbilirubinemia, Polycythemia
- Congenital Malformations (esp. with pre-GDM):
- Cardiac (VSD, TGA), CNS (NTDs)
⭐ Caudal regression syndrome is a rare but highly specific congenital anomaly associated with pre-gestational maternal diabetes.
- Stillbirth: Increased risk with poor glycemic control
Diabetes in Pregnancy - Sweet Control
- Goal: Euglycemia (Fasting <95 mg/dL, 1hr PP <140 mg/dL, 2hr PP <120 mg/dL).
- Management Steps:
- Medical Nutrition Therapy (MNT) & Exercise: First line.
- Pharmacological: If MNT fails.
- Insulin: Preferred. (📌 Insulin Is Ideal)
- Oral Hypoglycemics (OHAs): Metformin, Glyburide (cautious use).
- Monitoring: Self-monitoring of blood glucose (SMBG) 4-6 times/day.
- Intrapartum: Maintain glucose 80-110 mg/dL.
- Postpartum: Screen for overt diabetes at 6-12 weeks.
⭐ Oral Glucose Tolerance Test (OGTT) with 75g glucose is the standard for postpartum screening for diabetes after GDM.
High‑Yield Points - ⚡ Biggest Takeaways
- Screen GDM: 24-28 weeks with 75g OGTT.
- GDM diagnosis (75g OGTT): Fasting ≥92, 1-hr ≥180, 2-hr ≥153 mg/dL (any one).
- hPL: Main diabetogenic hormone, causes insulin resistance.
- Macrosomia (>4kg) is key fetal risk; shoulder dystocia ↑.
- Congenital anomalies (sacral agenesis) in pre-existing DM, not GDM.
- Insulin: First-line for GDM if diet fails; Metformin oral option.
- Postpartum: Screen for diabetes at 6-12 weeks with 75g OGTT.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

