Immunization Fundamentals - Immunity 101 Kickstart
- Immunization: Process inducing immunity against specific diseases, primarily via vaccination.
- Immunity: Body's defense against pathogens. Two main types: Active & Passive.
- Active Immunity:
- Host's immune system produces antibodies/cells after exposure to antigen (infection/vaccine).
- Lag period: Yes (days to weeks).
- Duration: Long-lasting (years/lifelong).
- Memory: Present; subsequent exposure leads to faster, stronger response (booster effect).
- Passive Immunity:
- Pre-formed antibodies are transferred to recipient.
- Lag period: No (immediate protection).
- Duration: Temporary (weeks to months, e.g., IgG half-life ~3 weeks).
- Memory: Absent.
⭐ Artificially acquired passive immunity provides immediate but temporary protection (e.g., anti-tetanus serum).
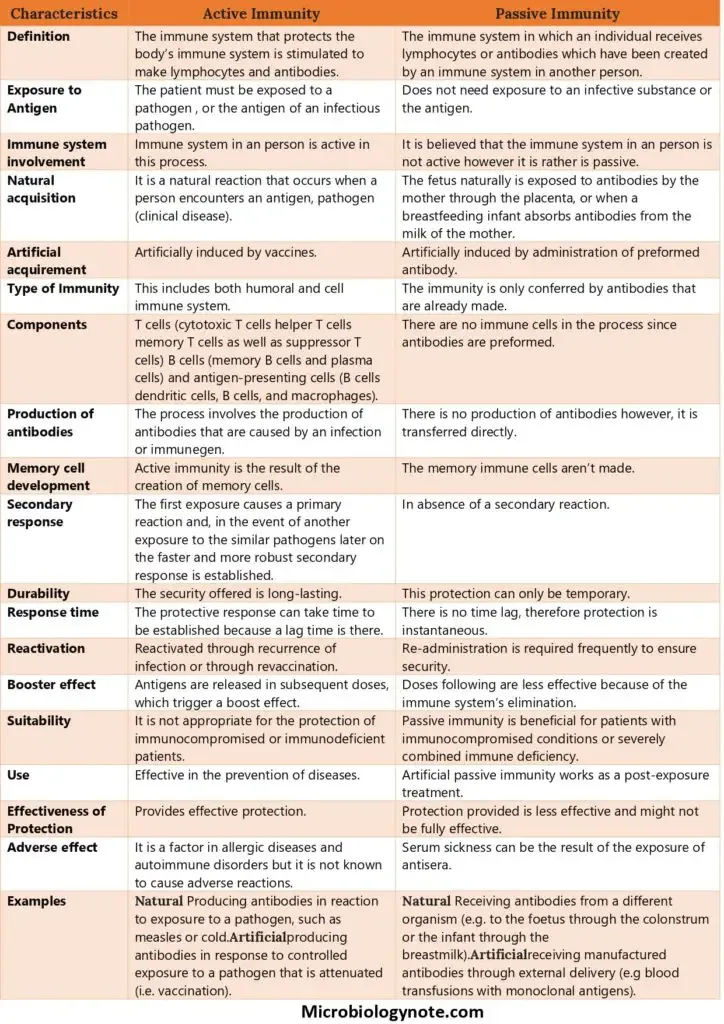
Vaccine Arsenal - Types & Tactics
⭐ Live attenuated vaccines generally provide longer-lasting immunity and elicit a strong cell-mediated response, but carry a risk of reversion to virulence.
| Type | Mechanism | Examples | Pros | Cons |
|---|---|---|---|---|
| Live Attenuated | Weakened pathogen | BCG, OPV, MMR, Varicella, Yellow Fever | Strong, long immunity (CMI/humoral) | Reversion risk, CI: immunocompromised |
| Inactivated (Killed) | Killed pathogen | IPV, Rabies, Influenza (inj.), Hep A | Safer, stable | Weaker immunity, multiple doses |
| Subunit | Antigenic parts (proteins, polysaccharides) | Tetanus, Diphtheria, Hep B, HPV, PCV, Hib | ↓ Side effects, defined antigen | Needs adjuvants/antigen ID |
| mRNA/DNA | Genetic material → host cells make antigen | COVID-19 (mRNA) | Rapid dev, strong CMI/humoral | Storage issues (some), newer tech |
Vaccine Admin & Response - The Immune Tango
- Admin Routes: IM, SC, ID (BCG), Oral (OPV), Intranasal.
- Site: Deltoid, anterolateral thigh (infants).
- Schedule: Primary series & boosters crucial.
- Cold Chain: ($+2$°C to $+8$°C) maintains potency.
- Immune Response:
- Primary: IgM → IgG, memory cells.
- Secondary (Anamnestic): Rapid, ↑IgG (memory).
- Factors Influencing Efficacy:
- Vaccine: Type, dose, adjuvants.
- Host: Age (extremes ↓), nutrition, immunity.
⭐ Adjuvants like aluminum salts (Alum) are used in some inactivated vaccines to enhance the immune response, particularly Th2 responses.
- Herd Immunity: Protects unvaccinated.
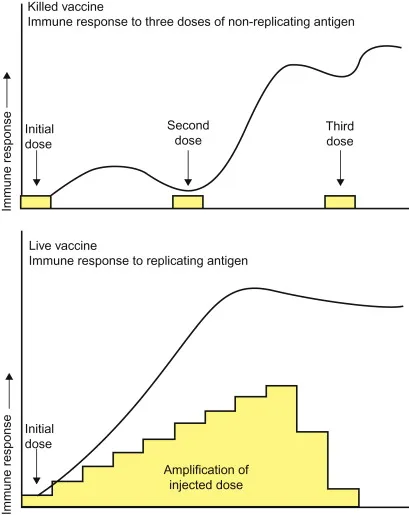
AEFI, Herd & Cold Chain - Beyond the Jab
- AEFI (Adverse Event Following Immunization): Any untoward medical event post-vaccination; not always causal. Crucial for safety surveillance.
- Types: Vaccine product-related, quality defect, immunization error, anxiety-related, coincidental.
- Serious AEFI: Death, life-threatening, hospitalization, persistent disability. Report promptly.
- Herd Immunity: Indirect protection of unimmunized when population immunity is high.
- Threshold ($1 - 1/R_0$, where $R_0$ is basic reproduction number): Proportion immune needed. E.g., Measles >95%.
- Protects vulnerable individuals (e.g., immunocompromised).
- Cold Chain: System ensuring vaccine potency via correct temperature storage/transport.
- Temp: Most +2°C to +8°C. Freezer (e.g., OPV, Measles): -15°C to -25°C.
- Vaccine Vial Monitor (VVM): Indicates cumulative heat exposure.
- Heat sensitive: OPV, Measles, BCG. 📌 "Old Men Are Best" (OPV, Measles, BCG).
- Freeze sensitive: DPT, TT, HepB, IPV. 📌 "Don't Touch The Ice Pack" (DPT, TT, HepB, IPV).
⭐ The cold chain is critical for maintaining vaccine potency, especially for live vaccines like measles and OPV, which are heat sensitive.

High‑Yield Points - ⚡ Biggest Takeaways
- Active immunity: Host immune response to antigen; long-lasting protection (e.g., post-vaccination).
- Passive immunity: Pre-formed antibodies transferred; immediate, temporary protection (e.g., maternal IgG).
- Herd immunity: Protects unvaccinated when population immunity is high, reducing pathogen spread.
- Live attenuated vaccines (MMR, OPV): Strong, often lifelong immunity; rare risk of reversion.
- Killed vaccines (IPV, Rabies): Safer, less immunogenic; require multiple doses/boosters.
- Adjuvants (Alum): Enhance immune response, especially for non-live/subunit vaccines.
- Anamnestic response: Faster, stronger, IgG dominant secondary immune response.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

