Definitions & Spectrum - Vax Views Vary
- Vaccine Hesitancy: Delay/refusal of vaccines despite availability of vaccine services. (WHO SAGE WG)
- Spectrum:
- Acceptance: Full trust, accepts all recommended vaccines.
- Hesitancy: Doubts, concerns, leading to delays or selective refusal.
- Anti-vaccination: Active opposition, often spreading misinformation.
- Key Factors:
- Confidence: Trust in vaccine safety/efficacy, and health services.
- Complacency: Low perceived risk of vaccine-preventable diseases (VPDs).
- Convenience: Ease of access, affordability, and understandability.
⭐ Vaccine hesitancy is a continuum, not a simple yes/no decision.
Causes & Drivers - Doubt's Deep Dive
- Misinformation & Disinformation:
- Social media rapidly amplifies false or misleading claims.
- Persistence of discredited theories (e.g., MMR-autism myth).
- Trust Deficits:
- In healthcare systems, pharmaceutical industry, or government bodies.
- Stemming from past unethical research or negative personal experiences.
- Personal, Philosophical & Religious Beliefs:
- Preference for "natural" immunity or reliance on alternative medicine.
- Ethical or moral objections to vaccine ingredients or development processes.
- Risk Perception Imbalance:
- Overstated fear of rare adverse events following immunization (AEFIs).
- Underestimation of severity and complications of vaccine-preventable diseases (VPDs).
- Complacency & Low Perceived Threat:
- VPDs seem like a distant or eradicated threat due to prior vaccination success.
- Belief that diseases are inherently mild or easily treatable without vaccination.
⭐ The thoroughly debunked 1998 Wakefield study, which fraudulently linked the MMR vaccine to autism, remains a significant historical driver of anti-vaccine sentiment and public health challenges.
Impact & Consequences - Immunity Under Siege
- ↓ Herd immunity threshold: Compromises community protection, especially for vulnerable (infants, immunocompromised, elderly).
- Resurgence of Vaccine-Preventable Diseases (VPDs):
- Measles, mumps, rubella, pertussis outbreaks.
- Polio re-emergence risk in under-vaccinated areas.
- ↑ Morbidity & mortality: Preventable deaths & disability, particularly in children.
- Healthcare system strain: Costly outbreak investigations & management.
- Economic burden: Treatment costs, productivity loss, public health expenditure.
- Erosion of public trust: In vaccines, healthcare, and scientific institutions.
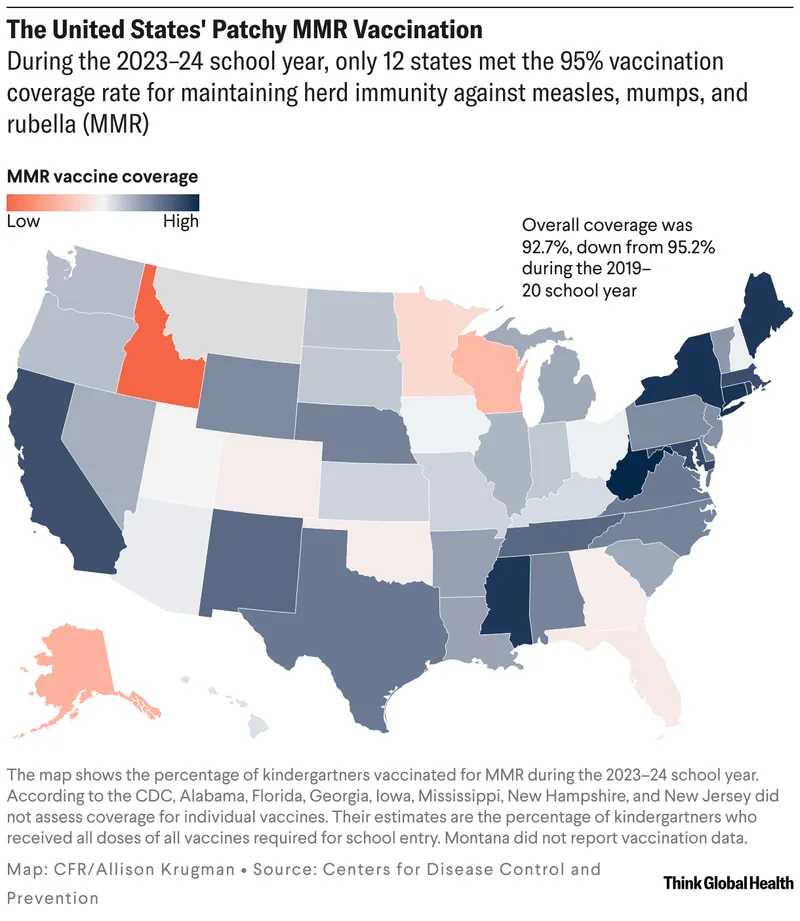
⭐ Measles, a highly contagious VPD, requires >95% population immunity (herd immunity threshold) to prevent outbreaks.
Addressing Hesitancy - Confidence Crusaders
Strategies to build vaccine confidence and counter misinformation. Focus on empathy, trust, and clear communication.
- Healthcare Provider (HCP) Role:
- CASE Approach:
- Corroborate: Acknowledge concerns.
- About Me: Share your stance as HCP.
- Science: Explain evidence simply.
- Explain/Advise: Recommend vaccination.
- Use motivational interviewing techniques.
- Provide strong, clear, empathetic recommendations.
- CASE Approach:
- Communication Strategies:
- Tailor messages (cultural, linguistic needs).
- Emphasize benefits: individual & community protection.
- Address misinformation promptly with verified facts.
- 📌 "LISTEN": Listen actively, Identify specific concerns, Share tailored facts, Tell stories (anecdotes), Encourage questions, Nurture ongoing trust.
- Community Engagement:
- Partner with community leaders, faith-based organizations, and local influencers.
- Empower peer educators and vaccine champions.
⭐ Healthcare providers are the most trusted source of vaccine information. Their strong, empathetic recommendation is a key factor in vaccine acceptance.

Indian Context - Bharat's Shield Strategy
- Mission Indradhanush (MI) & IMI: Boost routine immunization; target unvaccinated/partially vaccinated children & pregnant women.
- CoWIN Platform: Digital backbone for COVID-19 vaccine rollout; scheduling, tracking, certification.
- ASHA & Anganwadi Workers: Key grassroots motivators, build vaccine confidence, address local concerns.
- IEC Campaigns: Multi-platform communication to dispel myths, promote facts.
- Community Engagement: Involving religious leaders, local influencers to build trust.
⭐ India administered over 2 billion COVID-19 vaccine doses, showcasing its effective strategy.
High‑Yield Points - ⚡ Biggest Takeaways
- Vaccine hesitancy: Reluctance or refusal to vaccinate despite vaccine availability.
- Drivers: Misinformation (debunked MMR-autism link), religious/philosophical views, distrust, low perceived VPD risk.
- Wakefield's fraudulent 1998 study was a key trigger for anti-MMR sentiment.
- Social media rapidly spreads anti-vaccine narratives and misinformation.
- Results in VPD outbreaks (e.g., measles) and weakened herd immunity.
- Combating it: Transparent communication, community trust-building, HCP education.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

