Definitions & Criteria - Sepsis Starter Pack
- SIRS (Systemic Inflammatory Response Syndrome): ≥2 criteria:
- Temperature >38°C or <36°C
- Heart Rate >90/min
- Respiratory Rate >20/min or PaCO2 <32 mmHg
- WBC >12,000/mm³ or <4,000/mm³ or >10% immature bands
- Sepsis (Sepsis-3): Suspected infection + life-threatening organ dysfunction (SOFA score ↑ by ≥2 points).
- qSOFA (quick SOFA - bedside prompt for sepsis outside ICU, ≥2 criteria):
- Respiratory rate ≥22/min
- Altered mentation (GCS <15)
- Systolic BP ≤100 mmHg
- Septic Shock: Sepsis + persisting hypotension requiring vasopressors to maintain MAP ≥65 mmHg AND serum lactate >2 mmol/L despite adequate fluid resuscitation.
⭐ Sepsis-3 definition de-emphasized SIRS, focusing on organ dysfunction (SOFA score) for sepsis diagnosis.
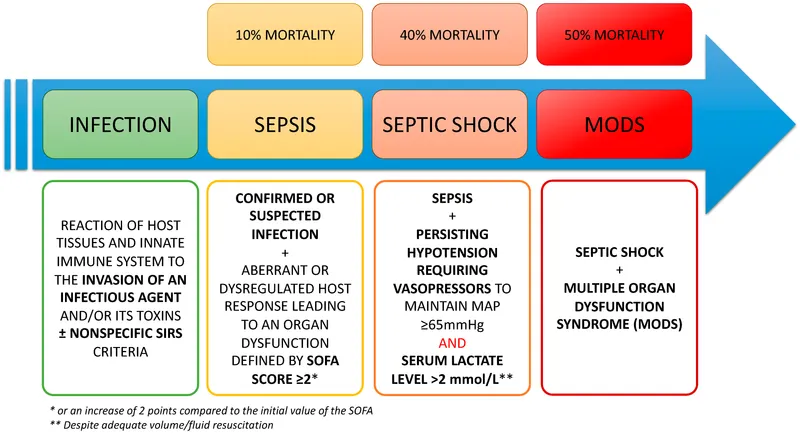
Pathophysiology of Sepsis - Cascade of Chaos
- Trigger: Pathogen-Associated Molecular Patterns (PAMPs, e.g., LPS from Gram-neg bacteria) or host-derived Damage-Associated Molecular Patterns (DAMPs) activate Pattern Recognition Receptors (PRRs, e.g., TLRs) on immune cells.
- Inflammatory Cascade: Leads to a "Cytokine Storm" - massive release of pro-inflammatory cytokines (TNF-α, IL-1β, IL-6).
- Activates complement & coagulation cascades (→ risk of Disseminated Intravascular Coagulation - DIC).
- Endothelial Dysfunction: Causes ↑vascular permeability, widespread vasodilation, and microthrombi formation.
- Cellular & Organ Damage: Results in tissue hypoperfusion, cellular hypoxia, and mitochondrial dysfunction, ultimately leading to Multiple Organ Dysfunction Syndrome (MODS).
- Immune Dysregulation: A simultaneous Compensatory Anti-inflammatory Response Syndrome (CARS), involving cytokines like IL-10, can occur, potentially leading to immunosuppression and susceptibility to secondary infections.
⭐ TNF-α is a key early mediator in sepsis, largely responsible for fever, hypotension, and initiating widespread inflammation leading to tissue injury.
Etiology & Microbiology - Bug Lineup
- Gram-Positive Cocci (GPC):
- Staphylococcus aureus (MSSA/MRSA): Skin, catheters, endocarditis.
- Streptococcus pneumoniae: Pneumonia, meningitis.
- Coagulase-Negative Staphylococci (CoNS): Catheters, implants.
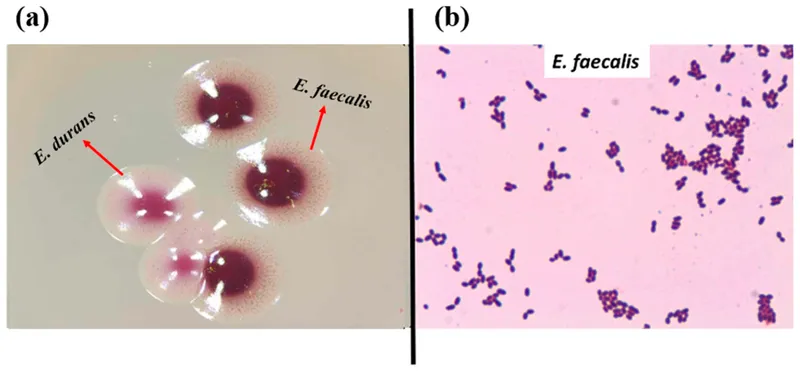
- Enterococci (E. faecalis, E. faecium): UTI, intra-abdominal, biliary.
- Gram-Negative Rods (GNR):
- Escherichia coli: UTI (commonest source), intra-abdominal.
- Klebsiella pneumoniae: Pneumonia, liver abscess, UTI.
- Pseudomonas aeruginosa: HAP/VAP, burns, neutropenia.
- Acinetobacter spp.: Ventilators, ICUs.
- Anaerobes: Bacteroides fragilis (intra-abdominal).
- Fungi: Candida spp. (e.g., C. albicans): Immunocompromised, CVCs, TPN.
⭐ Staphylococcus aureus is the leading cause of infective endocarditis in many regions and a frequent cause of catheter-related bloodstream infections (CRBSI).
Clinical Presentation & Diagnosis - Spotting Sepsis Signs
-
Red Flags (Think Sepsis!):
- Temp >38°C or <36°C; HR >90/min; RR >20/min
- Altered mental status; Hypotension (SBP <90 mmHg)
-
qSOFA Score (Bedside, ≥2 points = High Risk): 📌 HAT
- Hypotension (SBP ≤100 mmHg) - 1 pt
- Altered Mentation (GCS <15) - 1 pt
- Tachypnoea (RR ≥22/min) - 1 pt
-
Key Labs:
- Blood cultures (PRIORITY, pre-antibiotics!)
- Lactate (↑ = hypoperfusion)
- Procalcitonin, CRP
- CBC, Coags, LFTs, RFTs

⭐ Septic shock: Sepsis + persisting hypotension requiring vasopressors to maintain MAP ≥65 mmHg AND serum lactate >2 mmol/L despite adequate fluid resuscitation.
Sepsis Management - Rescue Mission
Rapidly implement Hour-1 Bundle (SSC):
- Lactate: Measure; remeasure if initial > 2 mmol/L.
- Cultures: Blood cultures before antibiotics.
- Antibiotics: Broad-spectrum IV within 1 hour.
- Fluids: 30 mL/kg IV crystalloid for hypotension or lactate ≥ 4 mmol/L.
- Vasopressors: If hypotensive post-fluids, for MAP ≥ 65 mmHg (Norepi 1st line).
⭐ Early administration of appropriate antibiotics (within 1 hour of recognition) is critical for improving survival in sepsis and septic shock.
High‑Yield Points - ⚡ Biggest Takeaways
- Sepsis: life-threatening organ dysfunction from dysregulated infection response; use qSOFA (≥2) or SOFA (↑≥2).
- Septic shock: sepsis + hypotension (MAP <65 mmHg despite fluids, needs vasopressors) + lactate >2 mmol/L.
- Common pathogens: S. aureus (GPC), E. coli, Klebsiella (GNB); Candida in immunocompromised.
- Key management: Early fluids (30mL/kg in 3h), antibiotics (<1hr), source control.
- Procalcitonin is a key biomarker for bacterial sepsis, aiding antibiotic de-escalation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

