AMR Fundamentals - Resistance Rising
- Antimicrobial Resistance (AMR): Microbes evolve, making drugs ineffective.
- Global Crisis: ↑morbidity, ↑mortality, ↑costs. India: high AMR burden.
- Drivers: Antibiotic overuse (humans, animals), poor infection control (IPC).
- Impact: Treatment failure, prolonged illness, costly/toxic alternatives.
⭐ Key Definitions:
- MDR (Multidrug-Resistant): Non-susceptible to $\ge$1 agent in $\ge$3 antimicrobial categories.
- XDR (Extensively Drug-Resistant): Non-susceptible to $\ge$1 agent in all but $\le$2 categories.
- PDR (Pandrug-Resistant): Non-susceptible to all agents in all antimicrobial categories.
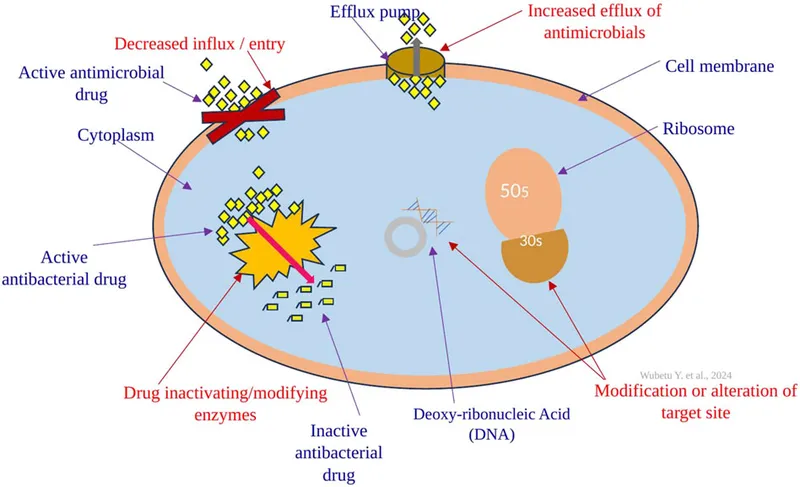
Resistance Mechanisms - Bugs' Clever Tricks
- Enzymatic Inactivation: Drug destroyed/modified.
- $\beta$-lactamases: Hydrolyze $\beta$-lactam ring (Penicillinases, ESBLs, Carbapenemases like NDM-1, KPC).
⭐ Beta-lactamases, like penicillinase, break the $\beta$-lactam ring of antibiotics (e.g., penicillin), inactivating them.
- Aminoglycoside-modifying enzymes (AMEs): Acetylation, phosphorylation.
- Chloramphenicol Acetyltransferase (CAT).
- Target Site Modification: Drug binding site altered.
- PBP change: mecA gene $\rightarrow$ PBP2a (MRSA).
- Ribosome change: 23S rRNA methylation (erm genes) $\rightarrow$ Macrolide resistance.
- Cell wall precursor: van genes (VRE) $\rightarrow$ D-Ala-D-Lac.
- DNA gyrase/Topoisomerase IV mutation $\rightarrow$ Quinolone resistance.
- $\downarrow$ Permeability / Uptake: Drug entry blocked.
- Porin loss/mutation (e.g., Gram-negatives vs carbapenems).
- Efflux Pumps: Drug actively expelled.
- ATP-dependent pumps remove antibiotics (Tetracyclines, Macrolides).
- Cause Multi-Drug Resistance (MDR). 📌 "Pump It Out!"
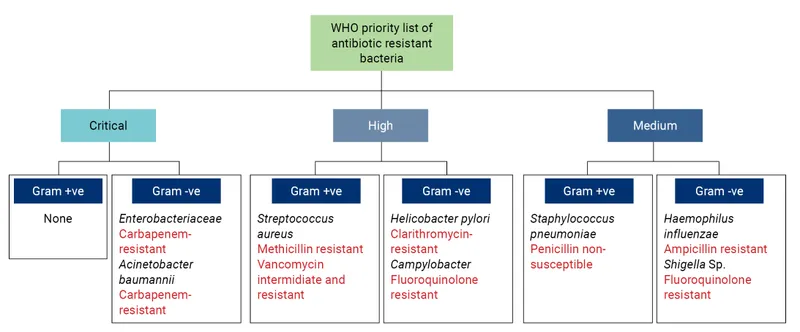
Key Resistant Pathogens - The Usual Suspects
- ESKAPE Pathogens (📌 Enterococcus, Staph, Klebsiella, Acinetobacter, Pseudomonas, Enterobacter): Major nosocomial threats & drivers of antimicrobial resistance.
- MRSA (Staphylococcus aureus): Methicillin-resistant due to mecA gene (altered PBP2a).
- VRE (Enterococcus faecium, E. faecalis): Vancomycin-resistant via vanA/vanB genes (altered D-Ala-D-Lac peptidoglycan target).
- ESBL-producers (e.g., E. coli, Klebsiella pneumoniae): Extended-Spectrum β-Lactamases hydrolyze most penicillins, cephalosporins (1st-3rd gen), monobactams.
- CRE (Carbapenem-Resistant Enterobacteriaceae e.g., Klebsiella, E. coli):
- Key Carbapenemases: KPC, OXA-48 like, VIM, IMP.
- MDR/XDR Acinetobacter baumannii: Multi-Drug Resistant / Extensively Drug-Resistant, often to carbapenems & colistin.
- MDR/XDR Pseudomonas aeruginosa: Intrinsic & acquired resistance; difficult to treat.
- Indian Scenario Highlights:
- High burden of NDM-1 (New Delhi Metallo-β-lactamase-1) producing Gram-negative bacteria.
- Emergence of colistin resistance (e.g., plasmid-mediated mcr-1 gene).
- Increasing resistance in Salmonella Typhi (fluoroquinolones, extended-spectrum cephalosporins).
⭐ NDM-1 (New Delhi metallo-beta-lactamase-1) is a prominent carbapenemase in India, conferring broad resistance to beta-lactams, including carbapenems, in Enterobacteriaceae and other Gram-negative bacteria.
Combating AMR - Our Strategic Moves
- Core Strategies (A.S.P.I.R.E. 📌):
- Antimicrobial Stewardship (AMS): Optimize use (right drug, dose, duration).
- Surveillance & Monitoring: Track resistance patterns (e.g., ICMR-AMRSN, NCDC).
- Prevention & Control (IPC): Strengthen hand hygiene, sanitation, biosecurity.
- Innovation (R&D): Develop new antibiotics, diagnostics, vaccines.
- Regulation & Policy: Control OTC sales, ensure quality of antimicrobials.
- Education & Awareness: For public, healthcare providers, policymakers.
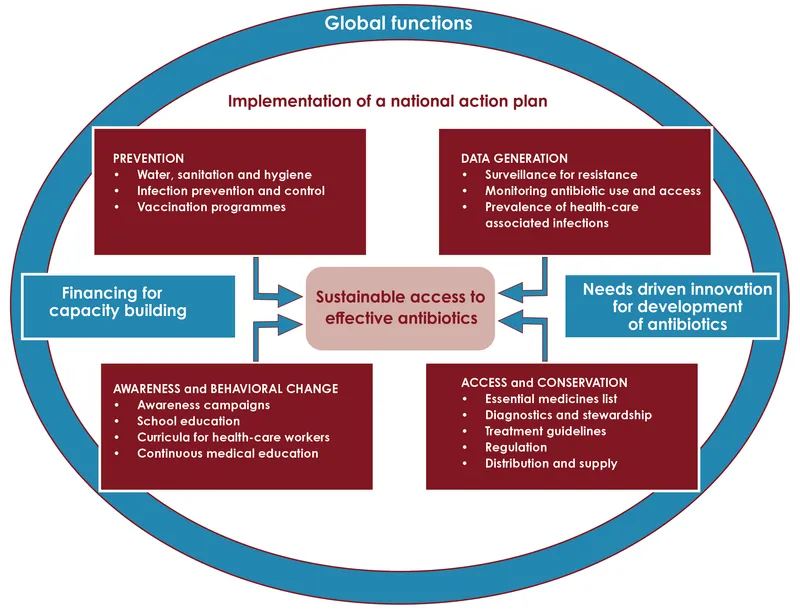
- National Action Plan on AMR (NAP-AMR) India:
- Launched 2017, based on WHO Global Action Plan.
- Emphasizes 'One Health' across its strategic priorities.
- ⭐ > The 'One Health' approach, integrating human, animal, and environmental health, is a cornerstone of India's National Action Plan on AMR.
- Global Collaboration: WHO GLASS, Global AMR R&D Hub.
High‑Yield Points - ⚡ Biggest Takeaways
- ESBLs, MBLs (e.g., NDM-1), KPC are major resistance mechanisms in Gram-negatives.
- MRSA (mecA) and VRE (vanA/vanB) remain critical Gram-positive resistant pathogens.
- Horizontal gene transfer via plasmids and transposons accelerates resistance spread.
- Biofilm formation significantly contributes to antibiotic treatment failure.
- MDR-TB and XDR-TB represent severe forms of drug-resistant tuberculosis.
- Emergence of colistin resistance (mcr-1 gene) limits last-resort treatment options.
- Antimicrobial stewardship programs are vital to control resistance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more