Mycobacteria Basics - The Acid-Fast Actors
- Acid-Fast Bacilli (AFB): Resist decolorization by acid-alcohol due to high mycolic acid content in cell wall.
- Stains: Ziehl-Neelsen (ZN) (red bacilli), Kinyoun (cold ZN), Auramine-Rhodamine (fluorescent).
- Cell wall: Rich in lipids (mycolic acid, lipoarabinomannan (LAM), Wax-D) → impermeability, resistance to disinfectants & antibiotics.
- Physiology: Strict aerobes; non-motile, non-spore-forming rods.
- Growth: Very slow; M. tuberculosis generation time ~15-20 hours.
- Culture media: Lowenstein-Jensen (LJ), Middlebrook 7H10/7H11.
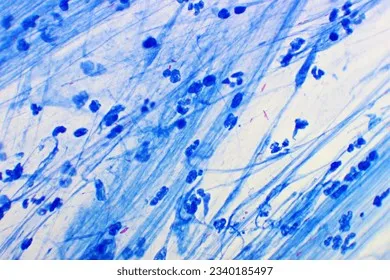 among blue background cells using Ziehl-Neelsen stain)
among blue background cells using Ziehl-Neelsen stain)
- Culture media: Lowenstein-Jensen (LJ), Middlebrook 7H10/7H11.
⭐ Cord factor (trehalose-6,6'-dimycolate) is a key virulence factor in M. tuberculosis, associated with serpentine cord-like growth in culture and inhibition of phagosome-lysosome fusion.
Tuberculosis - The Great Masquerader
- Agent: Mycobacterium tuberculosis (MTB), Acid-Fast Bacilli (AFB).
- Transmission: Airborne.
Primary TB:
- Non-sensitized host; often asymptomatic.
- Pathology:
- Ghon focus (subpleural lesion) + hilar lymphadenopathy = Ghon complex.
- Calcified Ghon complex = Ranke complex.
- Outcome: Latent TB Infection (LTBI) or primary progressive disease.
Post-Primary (Secondary) TB:
- Reactivation of LTBI or reinfection.
- Lung apices favored (high O₂).
- Symptoms: Chronic cough, fever, night sweats, weight loss, hemoptysis. Cavitation common.
Extrapulmonary TB (EPTB):
- Common sites:
- Lymph nodes (most frequent)
- Pleura, CNS (meningitis)
- Bone (Pott's disease), joints
- Genitourinary tract, GIT, Pericardium
Diagnosis:
- Immune-based tests:
- TST/Mantoux: Induration ≥5-15mm (risk-dependent).
- IGRAs (e.g., QuantiFERON-TB Gold).
- Microbiological confirmation:
- AFB Smear (ZN stain).
- Culture (LJ medium): Gold standard (2-8 wks).
- NAAT (GeneXpert): Rapid; detects Rifampicin resistance.
Treatment: Standard 6-month RIPE therapy (📌 Rifampicin, Isoniazid, Pyrazinamide, Ethambutol).

⭐ Rifampicin resistance in MTB is primarily due to mutations in the rpoB gene.
Leprosy Lowdown - Hansen's Unmasked
- Causative Agent: Mycobacterium leprae (Hansen's bacillus) - obligate intracellular, acid-fast.
- Transmission: Droplet infection (nasal secretions); prolonged close contact.
- Incubation Period: 2-5 years (can be up to 20 years).
- Spectrum: Based on cell-mediated immunity (CMI).
- Tuberculoid (TT): Strong CMI, few bacilli (paucibacillary - PB), localized lesions, nerve damage.
- Lepromatous (LL): Weak CMI, many bacilli (multibacillary - MB), diffuse lesions, skin thickening (leonine facies), high infectivity.
- Borderline forms: BT, BB, BL.
- Diagnosis: Slit-skin smear (Ziehl-Neelsen stain for AFB), skin biopsy (histopathology), Lepromin test (late TT).
- Treatment: Multidrug therapy (MDT) - Rifampicin, Dapsone, Clofazimine.
- PB: Rifampicin + Dapsone for 6 months.
- MB: Rifampicin + Dapsone + Clofazimine for 12 months.
- Reactions: Type 1 (Reversal), Type 2 (Erythema Nodosum Leprosum - ENL).

⭐ Lucio phenomenon, a severe necrotizing reaction, is seen in diffuse lepromatous leprosy (DLL).
NTMs Notables - The Atypical Cousins
- Runyon Classification Basis: Pigment production & growth rate.
- Group I (Photochromogens): M. kansasii (TB-like lung disease), M. marinum (fish tank/swimming pool granuloma). Pigment with light.
- Group II (Scotochromogens): M. scrofulaceum (cervical lymphadenitis in children). Pigment in dark.
- Group III (Nonchromogens): M. avium complex (MAC) - disseminated in AIDS (CD4 < 50/µL), Lady Windermere syndrome; M. ulcerans (Buruli ulcer).
- Group IV (Rapid Growers): M. fortuitum, M. chelonae. Grow in < 7 days; cause skin/soft tissue infections.

⭐ MAC is the most common NTM causing disseminated infection in AIDS patients (CD4 < 50 cells/µL); prophylaxis with azithromycin/clarithromycin is key.
High‑Yield Points - ⚡ Biggest Takeaways
- Mycobacteria: Acid-Fast Bacilli (AFB) due to mycolic acid; use Ziehl-Neelsen stain.
- M. tuberculosis (MTB): causes TB (airborne); diagnose: sputum (smear, LJ culture, NAAT/GeneXpert), TST, IGRA.
- Drug resistance: MDR-TB (resists isoniazid & rifampicin); XDR-TB (further key drug resistance).
- M. leprae: causes leprosy (Hansen's); tuberculoid to lepromatous forms; diagnose: skin biopsy/slit-skin smear.
- BCG vaccine (M. bovis): for TB prevention (severe childhood forms).
- Atypical mycobacteria (NTM): e.g., MAC, cause disease in immunocompromised patients.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

