SDB Spectrum - Defining the Zzz‑vil
Sleep-Disordered Breathing (SDB): Group of disorders with abnormal breathing during sleep.
- Key Terms:
- Apnea: Airflow stops ≥10s.
- Obstructive: Effort persists.
- Central: Effort absent.
- Hypopnea: Airflow ↓ ≥30% for ≥10s + ≥3% O₂ desat. or arousal.
- Apnea: Airflow stops ≥10s.
- Main Types:
- Obstructive Sleep Apnea (OSA): Repetitive upper airway collapse.
- Central Sleep Apnea (CSA): ↓/absent ventilatory drive.
- Obesity Hypoventilation Syndrome (OHS): BMI ≥30 kg/m², daytime PaCO₂ >45 mmHg.
⭐ Apnea-Hypopnea Index (AHI) = (apneas + hypopneas)/hour of sleep. AHI ≥5/hr is diagnostic for OSA.
oka
OSA: Culprits & Clues - The Choke Hold
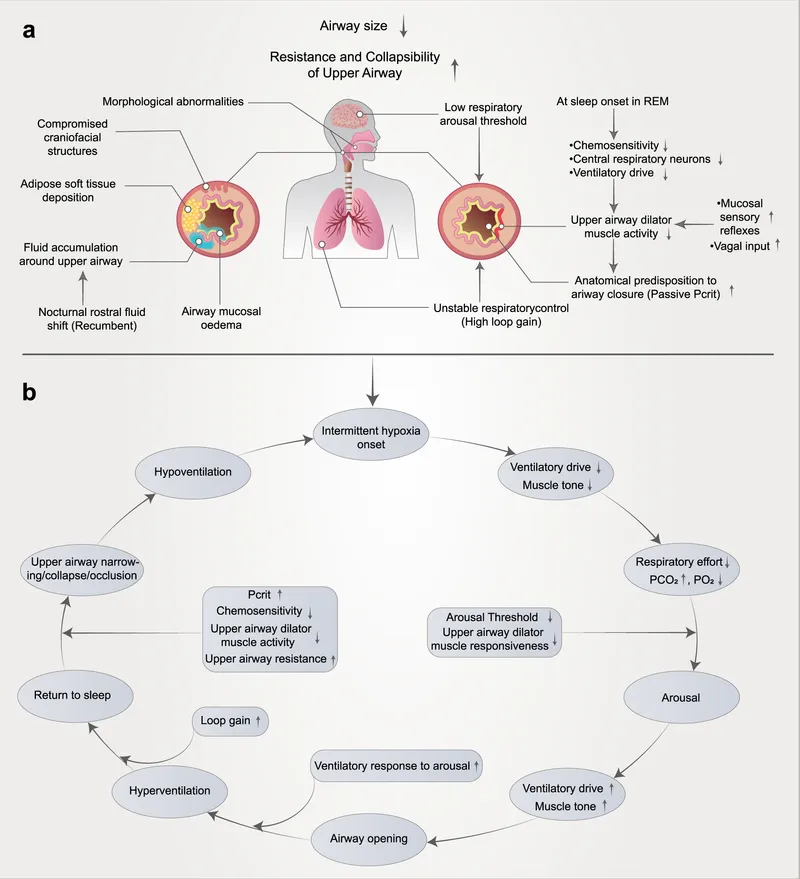
- Pathophysiology: The "Choke"
- Recurrent upper airway collapse during sleep due to:
- ↓ Pharyngeal muscle tone (e.g., genioglossus).
- Anatomical narrowing: Enlarged tonsils/adenoids, large tongue base, elongated soft palate/uvula.
- Inspiratory negative pressure overcoming airway dilator muscle activity.
- Recurrent upper airway collapse during sleep due to:
- Risk Factors: The "Culprits"
- Obesity (BMI > 30 kg/m²): Strongest risk factor. Neck circumference >17 inches (men), >16 inches (women).
- Craniofacial abnormalities: Retrognathia, micrognathia, adenotonsillar hypertrophy.
- Male gender; Increasing age (>40 years).
- Family history of OSA.
- Smoking, alcohol, or sedative use (especially before sleep).
- Endocrine disorders: Hypothyroidism, acromegaly.
- 📌 STOP-BANG Score (≥3 indicates high risk of OSA):
- Snoring loudly?
- Tired or fatigued during daytime?
- Observed apnea during sleep?
- High blood Pressure?
- BMI > 35 kg/m²?
- Age > 50 years?
- Neck circumference large?
- Gender male?
⭐ OSA is an independent risk factor for systemic hypertension, often resistant to standard antihypertensive therapy. It also significantly increases risk for arrhythmias (e.g., atrial fibrillation).
Diagnosing SDB - Unmasking the Night
- Clinical Red Flags:
- Loud Snoring, Witnessed Apneas, Gasping/Choking.
- Excessive Daytime Sleepiness (EDS): Epworth Sleepiness Scale (ESS) > 10.
- Morning headaches, fatigue, impaired concentration, nocturia.
- 📌 STOP-BANG (Snoring, Tired, Observed, Pressure, BMI, Age, Neck, Gender) for screening.
- Diagnostic Pathway:
-
Polysomnography (PSG): Gold Standard
- Comprehensive: EEG (sleep staging), EOG (eye movements), EMG (chin/limbs), ECG (arrhythmias), Airflow, Respiratory Effort (chest/abdomen), SpO2, Snoring.
-
Key Indices (events/hr):
- Apnea-Hypopnea Index (AHI): $AHI = \frac{\text{No. of Apneas} + \text{No. of Hypopneas}}{\text{Total Sleep Time (in hours)}}$.
- Respiratory Disturbance Index (RDI): AHI + Respiratory Effort-Related Arousals (RERAs).
-
SDB Severity (Adults, AHI/RDI):
- Normal: < 5
- Mild: 5-14.9
- Moderate: 15-29.9
- Severe: ≥ 30
⭐ OSA diagnosis: AHI ≥ 15/hr, OR AHI ≥ 5/hr with SDB symptoms (e.g., EDS, snoring, witnessed apneas) or associated medical/psychiatric disorders (e.g., HTN, CAD, mood disorder).
Managing SDB - Reclaiming Rest
- General Measures (All SDB):
- Weight loss (target >10% if overweight/obese).
- Positional therapy (e.g., tennis ball technique).
- Avoid alcohol & sedatives before sleep.
- Obstructive Sleep Apnea (OSA):
- CPAP (Continuous Positive Airway Pressure): Mainstay for moderate-severe OSA. Improves AHI, daytime somnolence, QoL.
⭐ CPAP is the first-line treatment for symptomatic moderate to severe Obstructive Sleep Apnea (OSA).
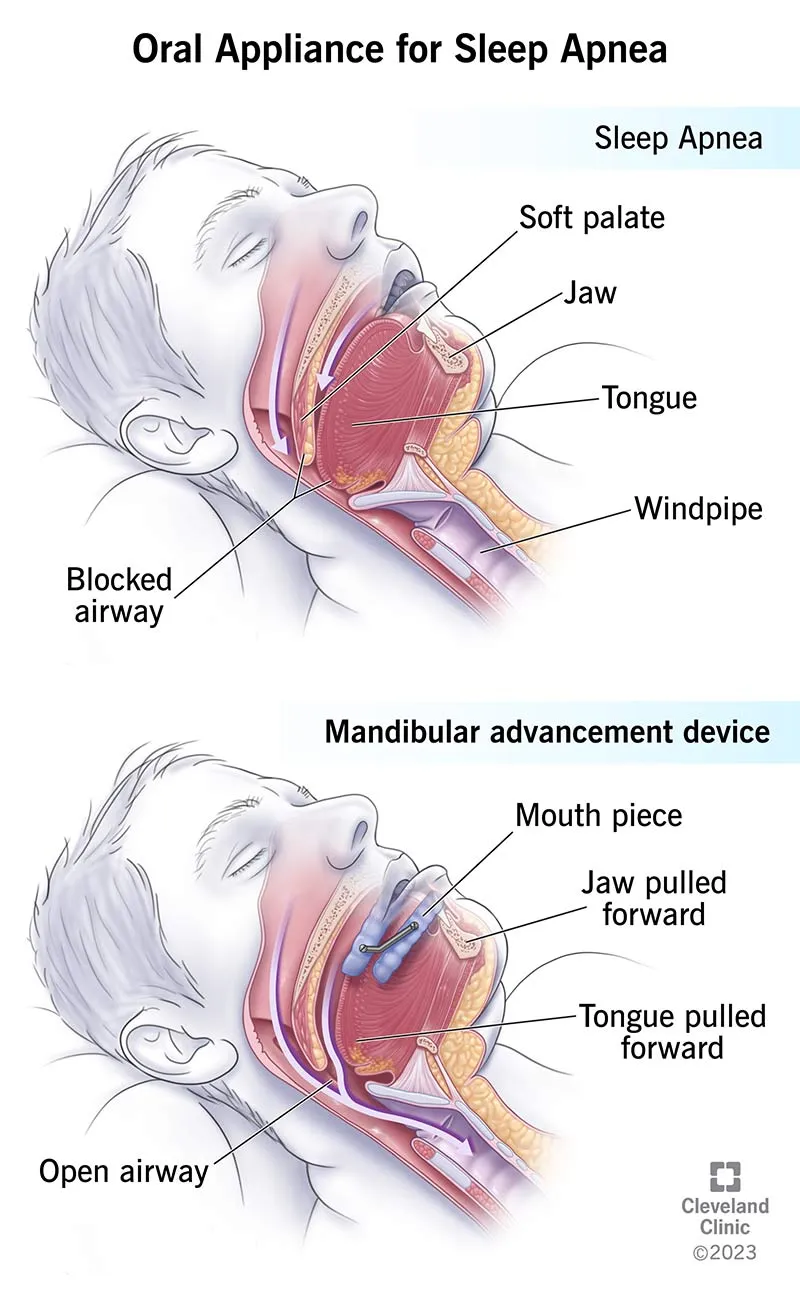
- Oral Appliances (Mandibular Advancement Devices - MADs): Mild-moderate OSA or CPAP intolerance.
- Surgical: Uvulopalatopharyngoplasty (UPPP), Maxillomandibular Advancement (MMA), bariatric surgery. Tracheostomy (rarely, severe refractory cases).
- CPAP (Continuous Positive Airway Pressure): Mainstay for moderate-severe OSA. Improves AHI, daytime somnolence, QoL.
- Central Sleep Apnea (CSA):
- Address underlying cause (e.g., heart failure, stroke, high altitude).
- Positive airway pressure (CPAP, BiPAP), Adaptive Servo-Ventilation (ASV).
- Oxygen, acetazolamide (limited use).
- Obesity Hypoventilation Syndrome (OHS):
- Aggressive weight loss.
- Nocturnal Non-Invasive Ventilation (NIV), usually BiPAP, to correct chronic hypoventilation.
High‑Yield Points - ⚡ Biggest Takeaways
- Obstructive Sleep Apnea (OSA): Most common; recurrent upper airway collapse during sleep.
- Polysomnography (PSG): Gold standard for diagnosis.
- AHI severity based on events/hr: Mild (5-15), Moderate (15-30), Severe (>30).
- CPAP: First-line, most effective therapy for moderate to severe OSA.
- Key risk factors: Obesity (BMI >30), male gender, age, craniofacial abnormalities.
- Central Sleep Apnea (CSA): Characterized by absent respiratory effort (CNS origin).
- Overlap Syndrome (OSA + COPD): Associated with significantly worse prognosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

