Overview & Classification - Brains Fading Fast
- Definition: Insidious onset, progressive loss of specific neuronal populations, leading to characteristic clinical syndromes.
- Core Mechanisms:
- Proteinopathies: Misfolding & aggregation of proteins (Aβ, Tau, α-synuclein, TDP-43).
- Shared pathways: Oxidative stress, mitochondrial dysfunction, neuroinflammation, excitotoxicity.
- Classification (Protein-based):
- Tauopathies: Alzheimer's (AD), Pick's disease, Progressive Supranuclear Palsy (PSP).
- α-Synucleinopathies: Parkinson's Disease (PD), Lewy Body Dementia (LBD), Multiple System Atrophy (MSA).
- Amyloidopathies: AD (Aβ component).
- TDP-43 Proteinopathies: Amyotrophic Lateral Sclerosis (ALS), Frontotemporal Lobar Degeneration (FTLD-TDP).
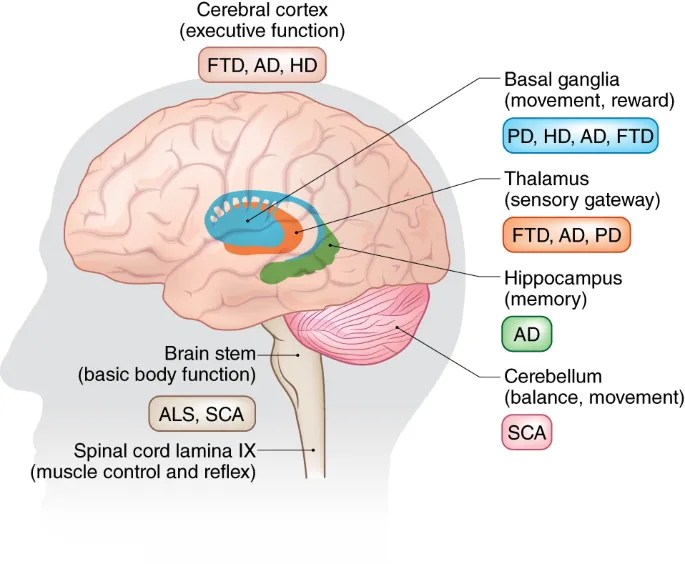
⭐ Huntington's disease is an autosomal dominant trinucleotide repeat disorder, distinct from most common proteinopathies but also a key neurodegenerative condition.
Alzheimer's Disease - Memory's Thief
- Pathology: Extracellular amyloid-β (Aβ) plaques & intracellular Tau neurofibrillary tangles (NFTs).
- Genetics:
- Early-onset: APP (Chr 21), PSEN1 (Chr 14), PSEN2 (Chr 1).
- Late-onset risk: APOE ε4 allele.
- Clinical: 📌 4 A's: Amnesia (anterograde first), Aphasia, Apraxia, Agnosia. Executive dysfunction.
- Diagnosis:
- Clinical criteria (e.g., NINCDS-ADRDA).
- CSF: ↓Aβ42, ↑Total Tau, ↑Phosphorylated Tau.
- Imaging: Medial temporal lobe (hippocampal) atrophy. PET for amyloid/tau.
- MMSE score <24/30 indicates cognitive impairment.
- Management:
- Cholinesterase inhibitors: Donepezil, Rivastigmine, Galantamine (mild-moderate).
- NMDA receptor antagonist: Memantine (moderate-severe).
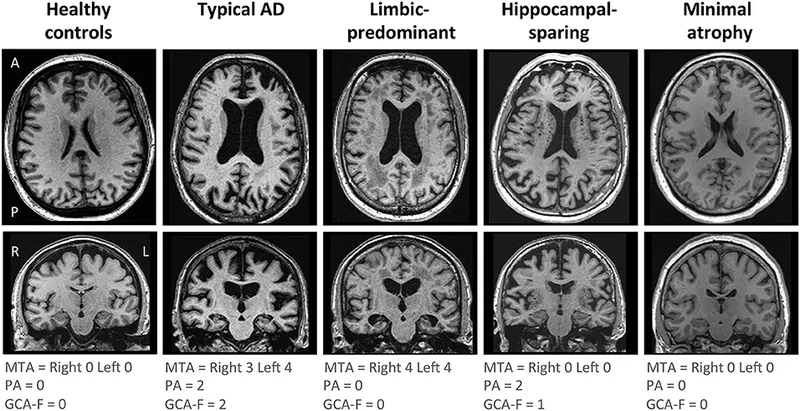
⭐ APOE ε4 is the most significant genetic risk factor for late-onset Alzheimer's disease.
Parkinson's Disease - Shakes & Slows
- Progressive loss of dopaminergic neurons (substantia nigra pars compacta) → ↓ striatal dopamine.
- Pathology: Lewy bodies (α-synuclein).
- Motor Symptoms (📌 TRAP):
- Tremor: Resting, pill-rolling (4-6 Hz), unilateral onset.
- Rigidity: Cogwheel or lead-pipe.
- Akinesia/Bradykinesia: Slow movement, micrographia, masked facies.
- Postural instability: Shuffling gait, festination (late).
- Non-motor: Anosmia, constipation, REM sleep behavior disorder, depression.
- Staging: Hoehn & Yahr (Stage 1-5).
- Rx: Levodopa/Carbidopa, Dopamine agonists, MAO-B inhibitors. Deep Brain Stimulation (DBS) for advanced.
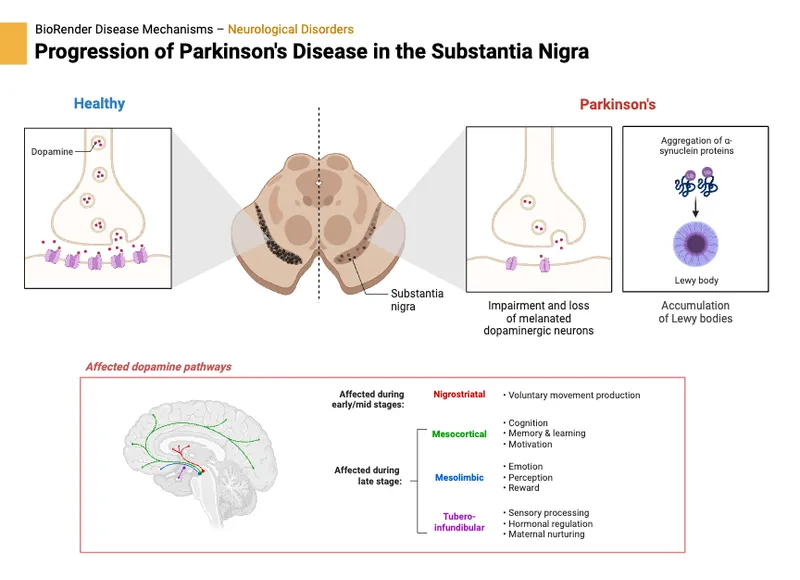
⭐ Asymmetric onset of motor symptoms is a key feature distinguishing PD from other parkinsonian syndromes.
LBD, FTD, HD, Prions - Diverse Decline
| Feature | Lewy Body Dementia (LBD) | Frontotemporal Dementia (FTD) | Huntington's Disease (HD) |
|---|---|---|---|
| Clinical | Parkinsonism, Visual Hallucinations, Fluctuating Cognition/Alertness. Poor L-DOPA response. | Behavioral changes (bvFTD: disinhibition, apathy) or Language (PPA). | Chorea, Cognitive (subcortical), Psychiatric (depression). Autosomal Dominant. |
| Pathology | α-synuclein (cortical Lewy bodies) | Tau (Pick bodies) or TDP-43 | CAG repeats (>39) HTT; Caudate atrophy; ↓GABA, ↓ACh |
| Onset | >60 yrs; RBD common precursor. | 45-65 yrs; insidious. | 30-50 yrs. |
⭐ LBD: Core feature is visual hallucinations; REM Sleep Behavior Disorder (RBD) is a strong early indicator.
Motor Neuron Disease - Muscles Wasting
- Progressive neurodegenerative disorder affecting upper motor neurons (UMN), lower motor neurons (LMN), or both, leading to muscle weakness and wasting.
- UMN Signs:
- Spasticity, hyperreflexia, ↑muscle tone.
- Babinski sign positive.
- Weakness pattern: Pyramidal.
- LMN Signs:
- Flaccidity, hyporeflexia/areflexia, ↓muscle tone.
- Muscle atrophy (wasting), fasciculations.
- Weakness pattern: Segmental/focal.
- Bulbar involvement (dysphagia, dysarthria) common.

⭐ Amyotrophic Lateral Sclerosis (ALS) is the most common form, characterized by combined UMN and LMN signs. No sensory or cognitive (usually) impairment initially. Riluzole may offer modest survival benefit (2-3 months).
High‑Yield Points - ⚡ Biggest Takeaways
- Alzheimer's Disease: Amyloid plaques, tau tangles; ApoE4 risk; most common dementia.
- Parkinson's Disease: Dopamine loss (substantia nigra); Lewy bodies (α-synuclein); tremor, rigidity, bradykinesia.
- Huntington's Disease: Autosomal Dominant, CAG repeats (Chr 4); chorea, dementia.
- ALS: Combined UMN & LMN signs; progressive weakness; SOD1 mutations (familial).
- Frontotemporal Dementia (FTD): Early behavioral/language changes; Pick bodies (tau) or TDP-43.
- Lewy Body Dementia (LBD): Fluctuating cognition, visual hallucinations, parkinsonism; REM sleep disorder.
- Creutzfeldt-Jakob Disease (CJD): Rapidly progressive dementia, myoclonus; prions; spongiform changes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

