RRS & Code Activation - Early Warning, Swift Action
- RRS Triggers (Early Warning Signs):
- Vital signs: SBP <90/>180, HR <40/>130, RR <8/>30, SpO2 <90% (on O2).
- Urine output <0.5 ml/kg/hr for >2 hrs.
- Acute mental status change.
- Staff "worried" sign.
- Code Blue Activation (Cardiac Arrest):
- Unresponsive, pulseless, apneic/agonal breathing.
- Aim: Prompt intervention to prevent deterioration or manage arrest.
⭐ Acute change in mental status or vital signs (e.g., SBP <90, HR >130, RR >30) are key RRS triggers.
BLS & Initial Response - The First Critical Moves
- Scene Safety: Check area. Patient responsive? (Tap & shout).
- Call for Help: Activate emergency response (Code Blue), fetch AED.
- Assess: Simultaneously check carotid pulse & breathing (<10 sec).
- CPR (if no pulse/gasping): Follow C-A-B.
- Compressions: 100-120/min, depth 5-6 cm. Full recoil. Minimize interruptions.
- Airway: Head-tilt/chin-lift or jaw thrust.
- Breathing: 30 compressions : 2 breaths.
- Defibrillation: Attach AED/defibrillator ASAP. Follow prompts.
⭐ Minimize chest compression interruptions to <10 seconds; crucial for maintaining Coronary Perfusion Pressure (CPP).

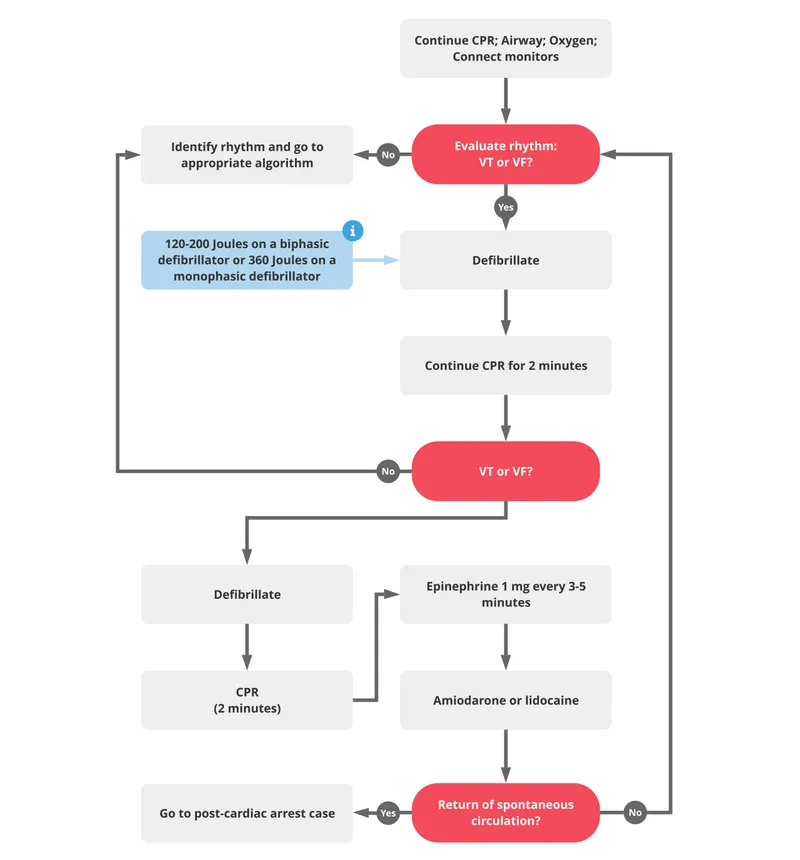
ACLS: Shockable Rhythms & Defib - VF/VT Victory
- Rhythms: Ventricular Fibrillation (VF), pulseless Ventricular Tachycardia (pVT).
- Immediate: Defibrillate! 📌 "Vee Fib? Dee Fib!"
- Energy: Biphasic 120-200J; Monophasic 360J.
- Algorithm Cycle: Shock → CPR (2 min) → Rhythm Check. Repeat.
- Medications (during CPR, if VF/pVT persists):
- Epinephrine 1mg IV/IO: Every 3-5 min (after 2nd shock).
- Amiodarone: 300mg IV/IO bolus (after 3rd shock), may repeat 150mg once.
- Lidocaine (if amiodarone unavailable): 1-1.5mg/kg IV/IO, then 0.5-0.75mg/kg.
⭐ For VF/pVT, immediate defibrillation is key. First shock with biphasic defibrillator: 120-200J (or manufacturer specific; if unknown, use maximum available).
ACLS: Non-Shockable & Reversibles - PEA/Asystole Puzzle
- PEA (Pulseless Electrical Activity) & Asystole: Non-shockable.
- Immediate Actions:
- High-quality CPR.
- Epinephrine 1 mg IV/IO every 3-5 minutes.
- NO defibrillation.
- Key: Identify & treat reversible causes (H's & T's).
⭐ In PEA/Asystole, always prioritize high-quality CPR and aggressively search for/treat reversible causes (H's & T's); Hypoxia and Hypovolemia are common culprits.
Reversible Causes (H's & T's): 📌
- H's: Hypovolemia, Hypoxia, H+ (acidosis), Hypo/Hyperkalemia, Hypothermia.
- T's: Tension pneumo, Tamponade, Toxins, Thrombosis (pulm/coronary).

Post-ROSC & Team Dynamics - Stabilize & Synthesize
- Post-ROSC Care (Stabilize):
- Optimize ABCs: Secure airway; target SpO₂ 94-98%, PaCO₂ 35-45 mmHg.
- Hemodynamics: MAP >65 mmHg; SBP >90 mmHg.
- Treat reversible causes (Hs & Ts).
- Neurological care:
⭐ Targeted Temperature Management (TTM) at 32-36°C for at least 24 hours is recommended for comatose adult patients with ROSC after cardiac arrest.
- Glucose control: Target 140-180 mg/dL.
- Team Dynamics & Synthesis:
- Clear roles, closed-loop communication.
- Structured debriefing: Learn, support, synthesize for ongoing care.
High‑Yield Points - ⚡ Biggest Takeaways
- Early recognition of deterioration (MEWS/NEWS) triggers Rapid Response Team (RRT) activation.
- Master the ABCDE approach for all emergencies.
- Immediate defibrillation for VF/pulseless VT; epinephrine every 3-5 min.
- Systematically address reversible causes (Hs and Ts) in cardiac arrest.
- Deliver high-quality CPR: rate 100-120/min, depth 5-6 cm, full recoil, minimal interruptions.
- Use amiodarone or lidocaine for refractory shockable rhythms.
- Implement post-cardiac arrest care protocols for optimal outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

