PUD Essentials - Defining the Damage
- Definition: Peptic Ulcer Disease (PUD) is a defect in the gastric or duodenal mucosa extending through the muscularis mucosae, typically ≥ 5 mm in diameter.
- Locations:
- Duodenal Ulcers (DU): Commonest; usually 1st part of duodenum (D1), anterior wall.
- Gastric Ulcers (GU): Often lesser curvature; Type I most common.
- Pathophysiology: Imbalance between mucosal aggressive factors (acid, pepsin, H. pylori, NSAIDs) and defensive mechanisms (mucus-bicarbonate layer, prostaglandins, blood flow, epithelial regeneration).
- ⭐ > Most common cause of PUD is H. pylori infection, followed by NSAID use.
- Other causes: Zollinger-Ellison Syndrome (gastrinoma), stress ulcers (Cushing's - ↑ intracranial pressure; Curling's - burns).
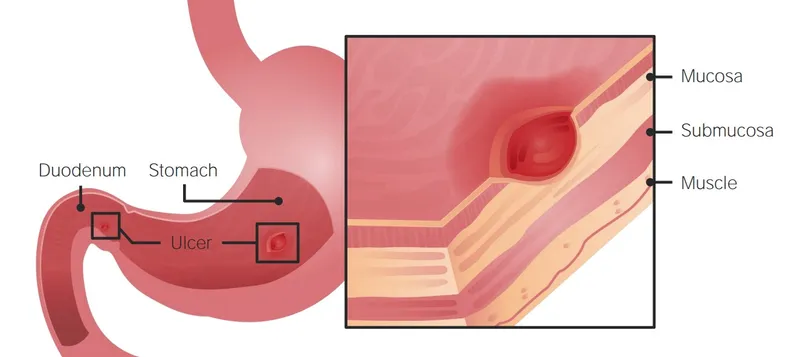
Pathophysiology & Symptoms - The Ulcer's Tale
- Pathophysiology: Imbalance: Aggressive factors (acid, pepsin, H. pylori, NSAIDs) overwhelm mucosal defensive factors (mucus, bicarbonate, prostaglandins, blood flow).
- H. pylori: Spiral-shaped; urease (NH₃ → local ↑pH → ↑gastrin → ↑acid). Virulence: CagA, VacA.
- NSAIDs: Inhibit COX-1 → ↓prostaglandins → ↓mucosal defense & repair.
- ZES: Gastrinoma → hypergastrinemia → ↑↑acid.
- Symptoms:
- Epigastric pain: Burning, gnawing. Timing with meals key.
⭐ Duodenal ulcer pain classically improves with meals (food buffers acid), while gastric ulcer pain worsens (food stimulates acid).
- Gastric Ulcer (GU): Pain ↑ with meals. Nausea, vomiting, weight loss.
- Duodenal Ulcer (DU): Pain ↓ with meals, recurs 2-3 hrs postprandial. Night pain common.
- Alarm: Bleeding (melena/hematemesis), anemia, weight loss, persistent vomiting, dysphagia.
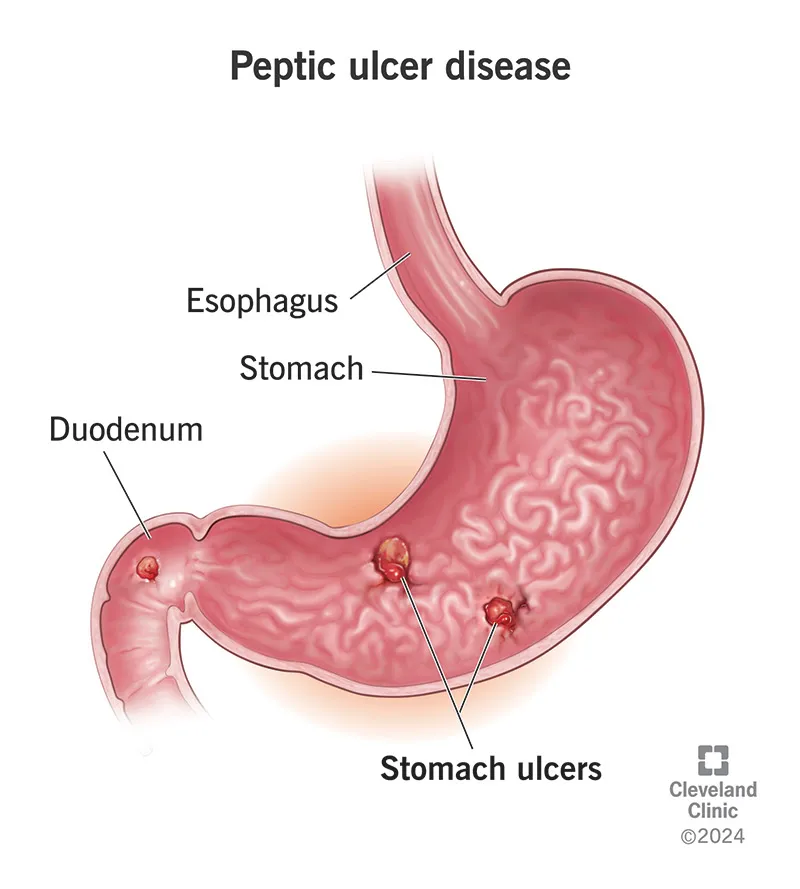
Diagnosis & H. pylori - Unmasking the Culprit
- Endoscopy (OGD): Gold standard. Biopsy for H. pylori & malignancy (gastric ulcers).
- Barium Meal: If endoscopy contraindicated.
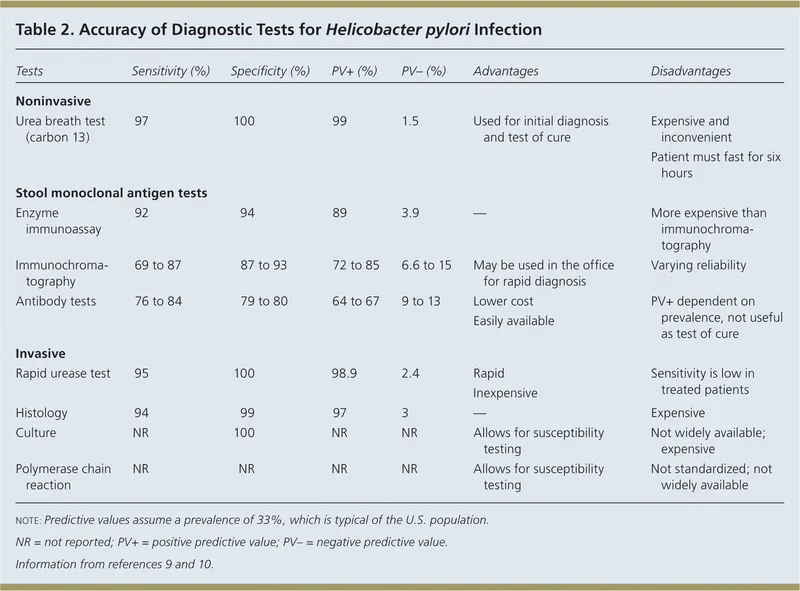
H. pylori Tests:
- Invasive (via Endoscopy):
- Rapid Urease Test (RUT): Quick, common.
- Histology: High sensitivity/specificity.
- Culture: For resistance.
- Non-invasive:
- Urea Breath Test (UBT): Diagnosis & eradication confirmation (stop PPI/Abx 4 wks prior).
- Stool Antigen Test (SAT): Similar to UBT.
- Serology (IgG): Exposure only, not for eradication check.
⭐ Upper GI endoscopy with biopsy is the gold standard for diagnosing PUD and allows for H. pylori testing and malignancy exclusion in gastric ulcers.
Treatment & Complications - Mending & Monitoring
- H. pylori Eradication (Key):
- Triple Therapy: PPI + Clarithromycin + Amoxicillin for 14 days.
- Quadruple Therapy (Bismuth/Non-Bismuth) for resistance/failure.
- Acid Suppression:
- Proton Pump Inhibitors (PPIs): e.g., Omeprazole 20-40mg OD.
- H2 Receptor Antagonists (H2RAs).
- Lifestyle: Avoid NSAIDs, smoking, alcohol.
- Surgery (Rare): For refractory ulcers or complications (e.g., vagotomy, antrectomy).
Key Complications (see flowchart):
- Key Complications (details):
- Bleeding (most common): Endoscopic Rx, IV PPI.
- Perforation: Surgical emergency.
- Gastric Outlet Obstruction (GOO): Dilation/surgery.
- Penetration: Into adjacent organs.
- Monitoring:
- Symptom relief.
- Gastric ulcer: repeat endoscopy (r/o malignancy).
- H. pylori test-of-cure (UBT/SAT).
⭐ Standard first-line triple therapy for H. pylori eradication includes a PPI + Clarithromycin + Amoxicillin for 14 days.
High‑Yield Points - ⚡ Biggest Takeaways
- H. pylori and NSAIDs are primary causes of Peptic Ulcer Disease (PUD).
- Duodenal ulcers: pain relieved by meals; Gastric ulcers: pain worsened by meals.
- Urea breath test or stool antigen test for H. pylori eradication confirmation.
- Standard triple therapy (PPI + two antibiotics) for H. pylori eradication is crucial.
- Major complications include bleeding (most common), perforation, and gastric outlet obstruction.
- Suspect Zollinger-Ellison syndrome with multiple or refractory ulcers.
- Endoscopy is diagnostic gold standard and allows for biopsy_._
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

