VRT Fundamentals - Dizzy No More!
- Vestibular Rehabilitation Therapy (VRT): Exercise-based program to improve symptoms of dizziness and imbalance from vestibular dysfunction.
- Goal: Promote central nervous system (CNS) compensation for vestibular deficits.
- Mechanisms:
- Adaptation: Modifies Vestibulo-Ocular Reflex (VOR) gain.
- Substitution: Enhances use of alternative sensory inputs (visual, somatosensory).
- Habituation: Reduces sensitivity to provocative stimuli through repeated exposure.
- Indications: Stable peripheral or central vestibular lesions (e.g., BPPV after canalith repositioning, unilateral/bilateral vestibular hypofunction, post-acoustic neuroma surgery).
- Contraindications: Unstable/fluctuating vestibular lesions, acute severe vertigo requiring medical management.
⭐ Cawthorne-Cooksey exercises form the historical basis of many VRT programs and are often customized for individual patient needs_._
Brain's Balancing Act - How VRT Works
- Leverages neuroplasticity: brain's adaptive capacity.
- Key Mechanisms of Central Compensation:
- Adaptation: Improves Vestibulo-Ocular Reflex (VOR) gain; crucial for gaze stability.
- Habituation: Reduces response to dizziness-inducing stimuli through repeated, controlled exposure.
- Substitution: Utilizes visual and somatosensory cues to replace lost vestibular function.
- Sensory Re-weighting: Shifts reliance towards more accurate or available sensory inputs.
⭐ Central compensation, the core of VRT, can begin within days post-vestibular insult, highlighting the brain's rapid adaptive potential. oka
VRT Toolkit - Moves & Methods
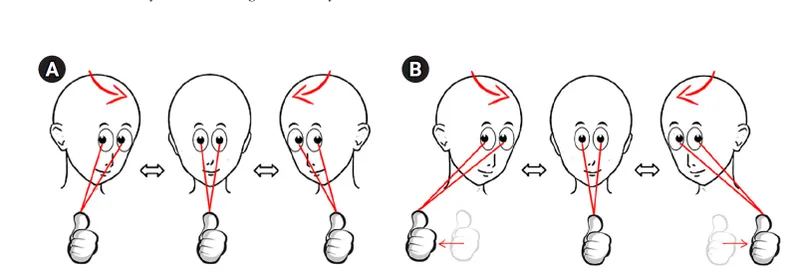
- Gaze Stability Exercises: Enhance focus during head motion.
- VOR x1: Head moves, target still.
- VOR x2: Head & target move oppositely.
- Habituation Exercises: Desensitize to provoking stimuli.
- Repeated exposure to dizziness triggers.
- Example: Brandt-Daroff exercises.
- Balance Training (Postural Stability): Improve steadiness.
- Static: Standing on varied surfaces, eyes open/closed.
- Dynamic: Walking with head turns, tandem gait.
- Canalith Repositioning Maneuvers (CRMs): For BPPV.
- Epley (posterior canal).
- Semont (posterior canal).
- Barbecue roll (horizontal canal).
⭐ Brandt-Daroff exercises are habituation exercises used for residual dizziness post-CRM or when CRMs are not tolerated by the patient for BPPV management.
Condition-Specific VRT - Tailored Tactics
- BPPV:
- CRMs: Epley (post. canal), Semont; Gufoni, BBQ roll (horiz. canal).
- Brandt-Daroff exercises for residual dizziness (habituation).
⭐ Epley maneuver is primary treatment for posterior canal BPPV.
- UVH (e.g., Vestibular Neuritis):
- Gaze Stability: VOR x1, VOR x2 exercises improve VOR.
- Balance & Gait Training: Static/dynamic. Adaptation exercises.
- BVH (e.g., Ototoxicity):
- Substitution: Enhance visual & somatosensory cues.
- Gaze Stability: Use remembered/imaginary targets.
- Balance Training: Sensory augmentation; crucial fall prevention.
- Meniere's Disease (Inter-critical):
- Balance training & habituation for motion sensitivity.
- Avoid VRT during acute attacks.
- PPPD:
- Habituation: To provocative visual stimuli & self-motion.
- Sensory re-weighting, balance exercises, relaxation.
High‑Yield Points - ⚡ Biggest Takeaways
- VRT promotes gaze stability, postural control, and habituation via CNS plasticity.
- Includes Cawthorne-Cooksey exercises, gaze stabilization (VOR x1, x2), and balance training.
- Indicated for stable vestibular hypofunction (unilateral/bilateral), post-BPPV repositioning, and some central lesions.
- CRMs (Epley) are first-line for BPPV; VRT manages residual dizziness.
- Success depends on patient adherence, customized program, and early start.
- Significant improvement often seen in 4-8 weeks of consistent therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

